Many Medicare beneficiaries assume their insurance covers basic foot care like nail trimming and callus removal, only to receive an unexpected bill. The truth is, Medicare foot care guidelines are specific about what qualifies for coverage and what doesn’t. Understanding these rules before your appointment can save you from out-of-pocket surprises and help you get the care you actually need.
Medicare typically considers routine foot care a non-covered service. However, there are important exceptions. If you have a systemic condition like diabetes or peripheral vascular disease that puts your feet at risk, Medicare may cover services that would otherwise be excluded. The key lies in knowing which diagnoses qualify, what documentation your provider needs, and how often you can receive covered care.
At Achilles Foot and Ankle Center, we help patients across Central Virginia navigate these coverage questions every day. Our team works with Medicare and understands the specific criteria required for reimbursement approval. This guide breaks down the eligibility requirements, covered conditions, and frequency limits so you know exactly what to expect from your benefits.
Why Medicare foot care guidelines matter
Your foot health directly impacts your mobility, independence, and quality of life. When you understand medicare foot care guidelines before scheduling an appointment, you can plan for covered services and avoid paying hundreds of dollars for treatments you thought insurance would handle. Many beneficiaries discover too late that their routine nail trimming or callus care doesn’t meet Medicare’s criteria, leaving them with bills ranging from $50 to $200 per visit.
Financial protection through proper planning
Medicare’s coverage rules exist to distinguish between cosmetic maintenance and medically necessary care. If you have diabetes, peripheral arterial disease, or other qualifying conditions, you can receive covered foot care services that prevent serious complications. Without knowing these guidelines, you might skip important preventive visits because you assume Medicare won’t pay, or you might schedule unnecessary appointments expecting full coverage.
Understanding coverage criteria before your visit helps you budget accurately and get the care you need without financial surprises.
The documentation your podiatrist provides determines whether Medicare approves or denies your claim. Your provider must show that your foot condition stems from a systemic disease and that you cannot safely care for your feet yourself. This means proper diagnosis codes, detailed notes about your underlying conditions, and clear evidence of medical necessity in your records.
Health outcomes and complication prevention
Knowing when you qualify for covered care helps you access preventive services at the right intervals. Patients with diabetes who receive regular podiatric care reduce their amputation risk by up to 85% compared to those who skip visits due to cost concerns. When you understand frequency limits, you can schedule appointments strategically to maximize your benefits and maintain optimal foot health throughout the year.
What Medicare covers vs routine foot care
Medicare Part B draws a clear line between medical treatment and cosmetic maintenance when it comes to foot care. The distinction determines whether you pay nothing beyond your deductible and coinsurance or whether you cover the full cost out of pocket. Understanding this difference before your appointment prevents billing confusion and helps you plan your budget accordingly.
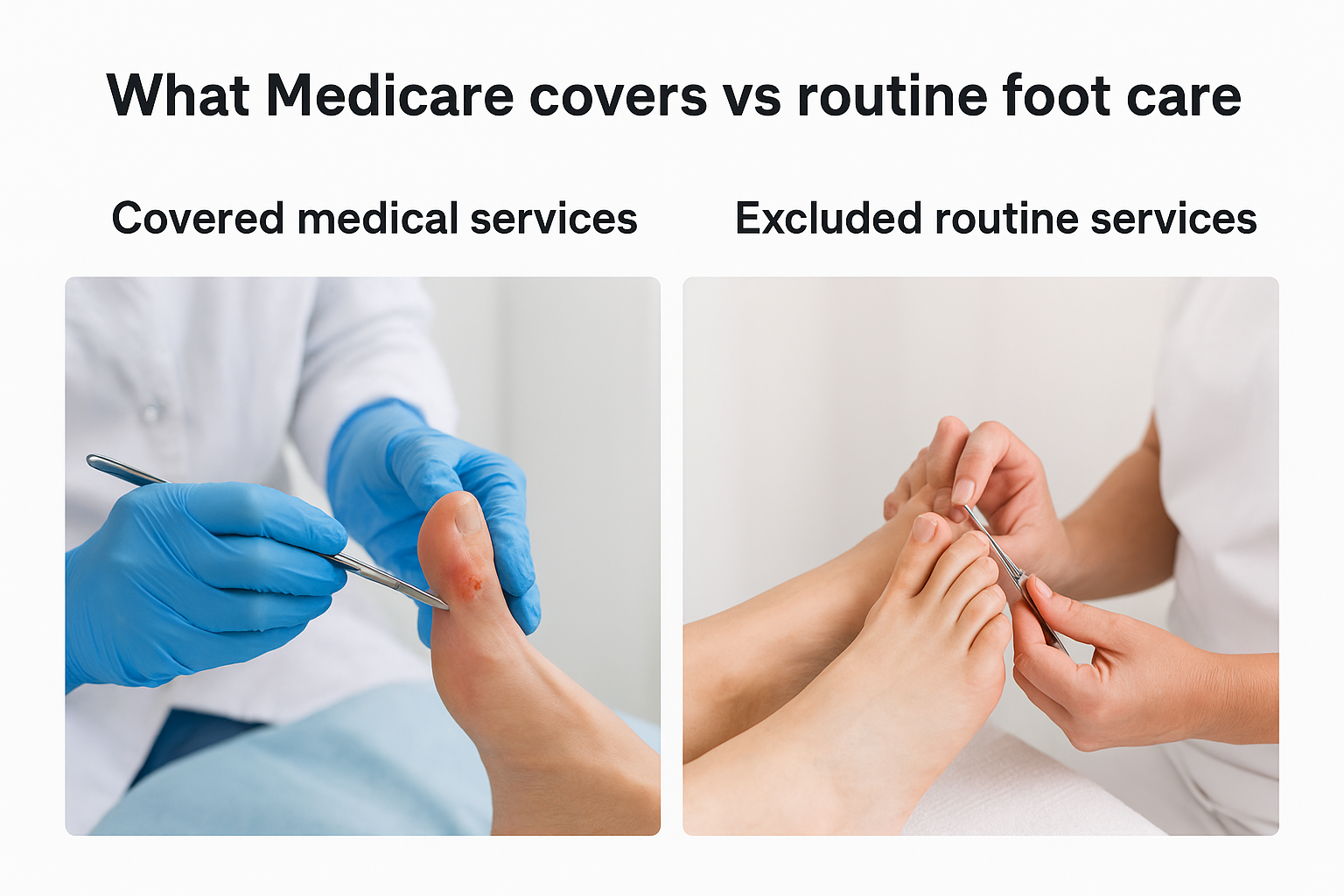
Covered medical services
Medicare pays for foot care when your condition results from or contributes to a systemic disease that affects your entire body. This includes treatment for infections, ulcers, wounds, and complications from diabetes or circulatory problems. Your podiatrist can bill Medicare for debridement of infected tissue, treatment of plantar warts, and management of fungal infections that pose health risks.
Medicare covers foot care services when they treat or prevent complications from qualifying medical conditions, not for general maintenance.
Diagnostic procedures like X-rays, ultrasounds, and nerve conduction studies receive coverage when your doctor needs them to evaluate your condition. Medicare also pays for therapeutic shoes and inserts if you have diabetes with specific foot complications documented in your medical records.
Excluded routine services
Standard nail trimming, callus removal, and general hygiene fall outside medicare foot care guidelines for coverage. You pay the full fee for these services unless your provider documents that you cannot safely perform them yourself due to a qualifying condition. Cosmetic procedures like treatment for corns or bunions that don’t cause functional problems also remain your responsibility.
Who qualifies for routine foot care coverage
You qualify for Medicare-covered routine foot care only when you have a systemic condition that makes self-care impossible or dangerous. Your diagnosis must appear on Medicare’s approved list of conditions, and your podiatrist must document why you cannot safely trim your own nails or remove calluses. Personal inability to reach your feet or poor vision alone does not meet the criteria without an underlying medical condition.
Qualifying medical conditions
Medicare recognizes specific systemic diseases that justify covered foot care. Diabetes with evidence of nerve damage or poor circulation tops the list, followed by peripheral arterial disease that reduces blood flow to your feet. You also qualify if you have chronic venous insufficiency, lymphedema affecting your legs, or severe arthritis that prevents you from bending to reach your feet.
Your qualifying condition must directly cause or worsen your inability to perform safe foot care at home.
Neurological disorders like peripheral neuropathy, multiple sclerosis, or stroke with residual effects meet medicare foot care guidelines when they impair your sensation or mobility. Your provider documents how your condition creates a substantial risk of injury or infection if you attempt self-care.
Required documentation standards
Your podiatrist must note your qualifying diagnosis and explain the connection between your condition and your need for professional foot care. The medical record should include evidence of diminished sensation, poor circulation test results, or physical limitations that prevent safe self-care. This documentation determines whether Medicare approves or denies your claim for routine maintenance services.
How often Medicare pays and frequency limits
Medicare foot care guidelines set specific limits on how frequently you can receive covered routine foot care services. Understanding these restrictions helps you schedule appointments strategically and avoid denials for visits that exceed the allowed frequency. Your podiatrist must space your treatments according to Medicare’s approved intervals, which vary based on your qualifying condition and medical needs.

Standard visit frequency for covered care
You can receive covered routine foot care approximately every 60 to 90 days when you have a qualifying systemic condition. Medicare does not pay for visits scheduled more frequently unless your doctor documents a specific medical change or complication that requires immediate attention. Your provider determines the exact timing based on your nail growth rate, callus formation, and overall foot health status.
Medicare allows more frequent visits only when medical necessity supports the increased treatment schedule.
Calendar year vs benefit period limits
Medicare counts your visits within calendar year cycles, not based on when you first received treatment. If you need routine foot care starting in November, you won’t get extra visits in January just because a new year began. Your podiatrist tracks these intervals carefully to ensure each claim meets coverage criteria and you receive maximum benefits without paying for denied services.
How to get covered care and avoid surprises
You take control of your foot care expenses by verifying your eligibility and communicating clearly with your provider before each appointment. Start by confirming that your podiatrist accepts Medicare assignment, which means they agree to accept Medicare’s approved amount as full payment. This single step prevents balance billing and keeps your costs predictable.
Verify your qualifying condition status
Your podiatrist’s office should review your medical records before scheduling routine foot care to confirm you have a qualifying systemic condition documented. Ask the billing staff whether your diagnosis meets medicare foot care guidelines for coverage and if your last visit falls within the allowed frequency limits. This conversation takes five minutes but saves you from paying $75 to $200 for services you thought insurance would cover.
Always confirm your coverage status before scheduling routine foot care appointments to avoid unexpected bills.
Request advance beneficiary notices when needed
If your visit might not meet coverage criteria, your provider must give you an Advance Beneficiary Notice (ABN) explaining the potential denial. You sign this form acknowledging you may pay the full cost if Medicare rejects the claim. Receiving this notice before treatment lets you decide whether to proceed with out-of-pocket payment or reschedule when you meet coverage requirements.
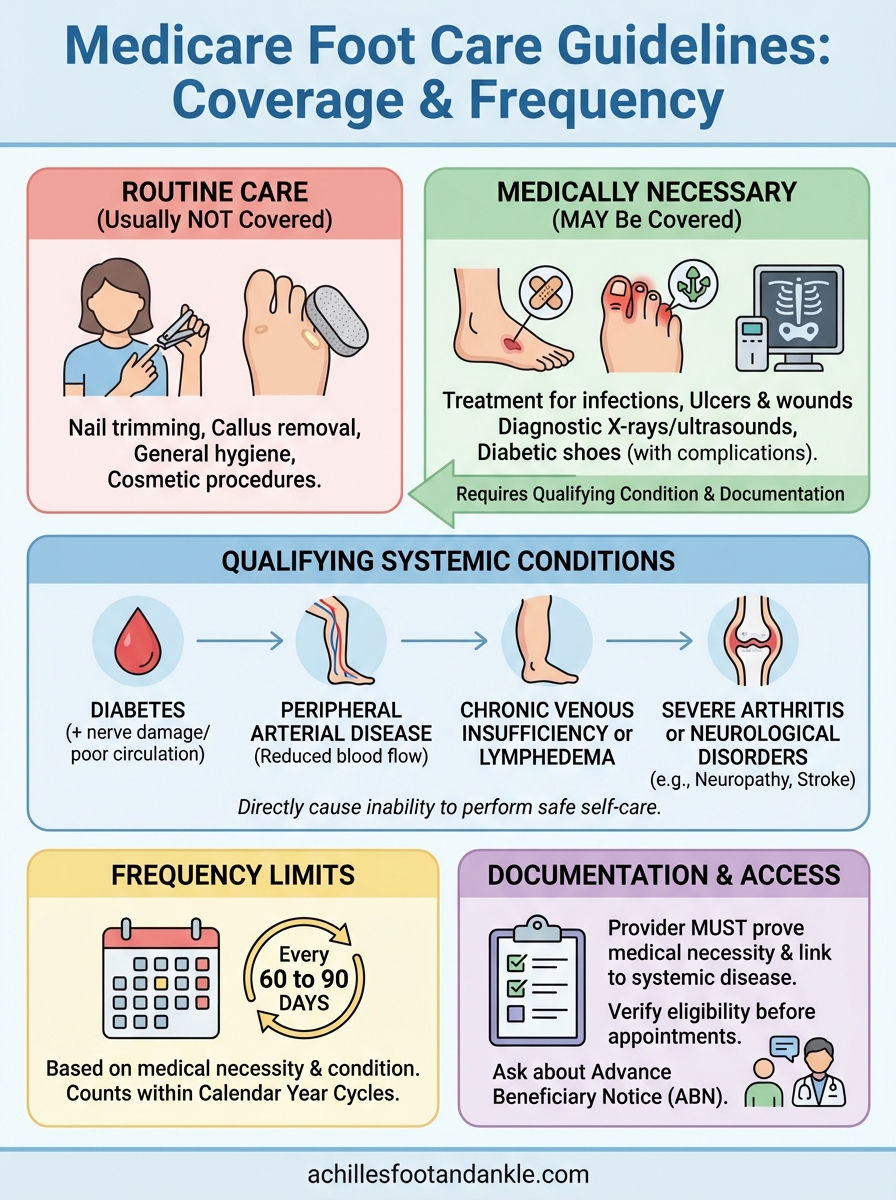
Key takeaways and when to call a podiatrist
Understanding medicare foot care guidelines protects you from unexpected bills and ensures you receive covered services when you qualify. You need a documented systemic condition like diabetes or peripheral vascular disease to receive routine foot care coverage, and your visits must stay within the allowed frequency limits of every 60 to 90 days. Your podiatrist handles the required documentation that proves medical necessity and connects your foot care to your qualifying diagnosis.
Contact a podiatrist immediately if you develop foot wounds, ulcers, or infections that don’t heal within a few days. Changes in sensation, color, or temperature in your feet signal circulation problems that need professional evaluation. Pain that persists beyond normal healing time or sudden swelling in your feet also requires medical attention regardless of your coverage status.
At Achilles Foot and Ankle Center, our team accepts all major insurance plans including Medicare and helps you understand your coverage before each visit. Schedule a same-day appointment when you need urgent foot care or want to discuss your eligibility for covered podiatry services.






