Heel pain that burns, shoots, or tingles along the inside of your foot doesn’t always point to the diagnosis you’d expect. Many patients arrive at our Central Virginia clinics convinced they have plantar fasciitis, only to learn that their real problem is nerve-related. Baxter’s nerve entrapment symptoms can closely mimic other common heel conditions, which is why this particular issue often goes undiagnosed for months or even years.
The inferior calcaneal nerve, commonly called Baxter’s nerve, runs along the inner heel and can become compressed by surrounding soft tissue or bone. When it does, the resulting pain, numbness, or burning sensation is easy to confuse with a handful of other diagnoses. Recognizing where the pain occurs, what it feels like, and when it shows up matters because the wrong diagnosis leads to the wrong treatment, and that means prolonged discomfort with no clear end in sight.
At Achilles Foot and Ankle Center, our podiatrists evaluate and treat nerve entrapment conditions across our thirteen locations in Central Virginia, using advanced diagnostic tools like ultrasound guidance and digital imaging to pinpoint the source of heel pain accurately. This article breaks down the specific signs of Baxter’s nerve entrapment, the pain patterns, the sensations, and the clinical features that separate it from plantar fasciitis and other look-alike conditions, so you can have a more informed conversation with your doctor about what’s really going on with your heel.
Why Baxter’s nerve symptoms often get missed
Most patients with Baxter’s nerve entrapment symptoms never hear that term from their first provider. Instead, they receive a plantar fasciitis diagnosis, begin standard treatments, and wait for improvement that never comes. The nerve is small, the pain it produces overlaps with several more familiar diagnoses, and most general practitioners are not routinely trained to test for inferior calcaneal nerve compression. Those factors combine to create a pattern where real nerve entrapment quietly continues while patients work through treatments designed for an entirely different problem.
The "plantar fasciitis first" assumption
When a patient walks into a clinic with heel pain that’s worst in the morning, the clinical reflex almost always points to plantar fasciitis first. That’s a reasonable starting point because plantar fasciitis is genuinely common. But that same predictability creates a diagnostic blind spot. Providers apply standard protocols, patients do stretches and use orthotics, and some improvement can occur because those interventions also reduce tension near the entrapment site. The underlying nerve compression, however, stays unresolved, and the pain either lingers at a low level or eventually climbs back to where it started.
When standard plantar fasciitis treatments provide only partial relief and heel pain keeps returning, nerve entrapment should enter the conversation, not remain an afterthought.
Anatomical location makes accurate pinpointing difficult
Baxter’s nerve travels through a narrow corridor between the heel bone and the inner foot’s soft tissue, an area packed with overlapping structures. When pain originates there, patients typically describe a diffuse inner heel ache rather than a pinpoint tender spot. That vague description fits multiple diagnoses, which makes isolation hard during a short appointment. Physical examination findings can appear completely normal on surface inspection, since most cases show no visible swelling, redness, or deformity.
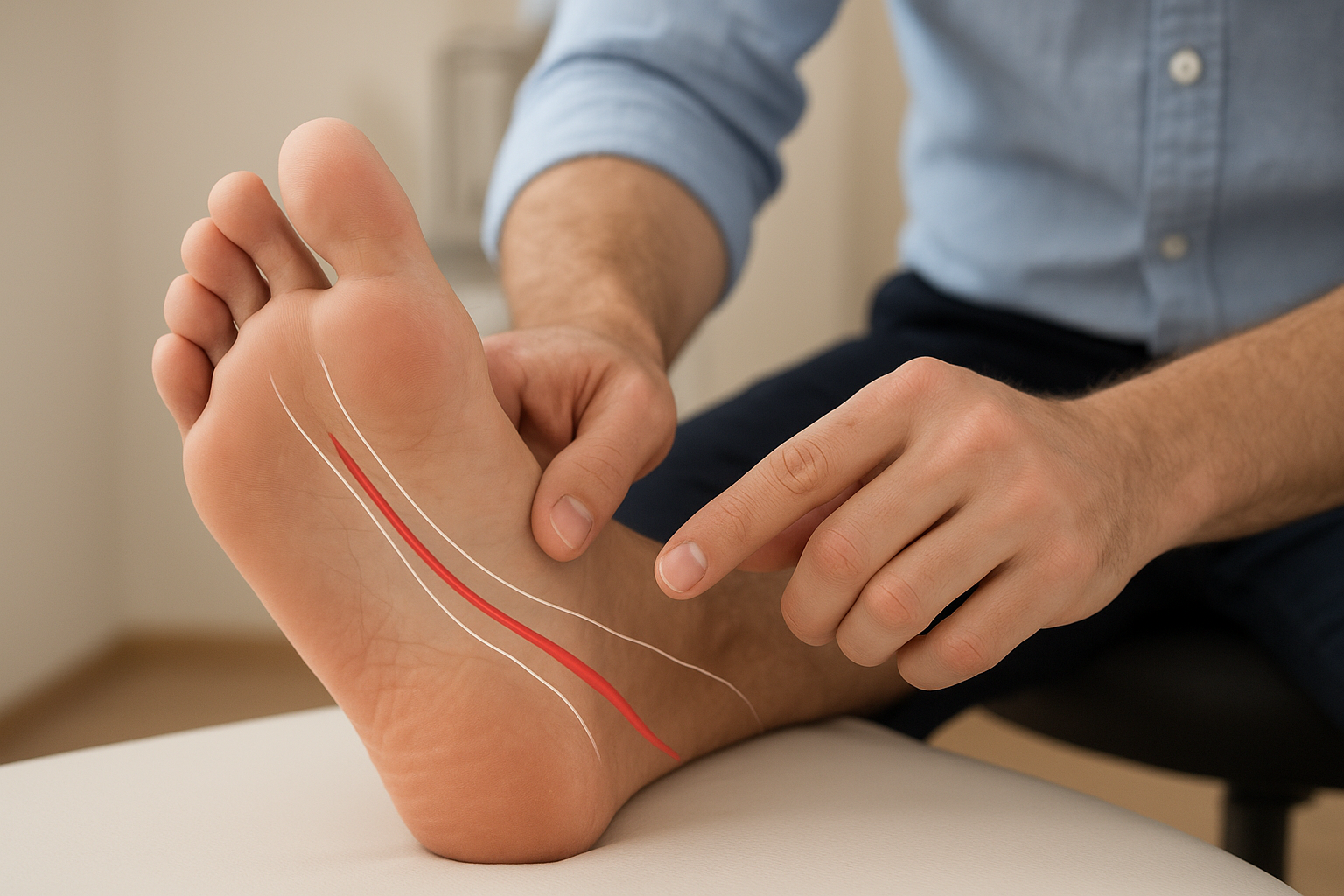
Without deliberate palpation along the nerve’s path or targeted imaging, a routine exam rarely digs far enough to find the actual compression site. Clinicians who aren’t specifically evaluating for inferior calcaneal nerve involvement may press the heel broadly, note tenderness, and attribute the finding to fascial irritation. The distinction requires a focused approach that a general visit doesn’t always allow time for.
Symptom patterns that shift over time
Another reason these cases slip through is that the sensations don’t stay constant. Early on, you might notice a dull inner heel ache that fades after warming up. Over weeks or months, that ache can shift into a burning sensation, intermittent numbness, or a pressure feeling against the base of your heel. Because the experience changes, you might assume your foot is gradually getting better or reacting to footwear changes rather than recognizing a nerve pattern. Tracking exactly when and where each sensation appears is something most patients don’t think to document before their appointment, which means the provider receives a fragmented history that doesn’t clearly point toward a nerve origin.
How to tell if your heel pain is nerve-related
Heel pain from a nerve source behaves differently than pain from a damaged ligament or inflamed fascia. When nerve tissue is compressed or irritated, the sensations it produces carry a distinct character that structural problems typically don’t replicate. Recognizing these differences before your appointment gives you and your clinician a clearer starting point and helps avoid another round of treatments aimed at the wrong diagnosis.
Signs that suggest nerve involvement
Structural heel pain, like plantar fasciitis, tends to cause a deep, achy soreness concentrated at the base of the heel near the fascia’s attachment point. Nerve-related pain adds a different quality on top of that, or sometimes instead of it entirely. You might notice burning, electrical-type shooting sensations, or a feeling that the skin along the inside of your heel is numb or abnormally sensitive to light touch. These sensations often extend beyond the heel itself, traveling into the arch or spreading toward the outer edge of the foot, which rarely happens with isolated fascia irritation.
If your heel pain includes any burning, numbness, or tingling sensation, nerve involvement becomes a strong possibility worth investigating with a specialist.
Questions to ask yourself about your symptoms
Paying close attention to a few specific patterns helps separate nerve-related pain from mechanical causes. Think about how your symptoms behave over the course of a day, because Baxter’s nerve entrapment symptoms often persist or intensify further into activity rather than easing off after an initial warm-up period. Also consider whether you notice any sensation changes, since numbness and tingling almost never come from plantar fascia irritation alone and point more directly toward a nerve source.
- Does the pain burn or shoot rather than just ache deeply?
- Do you notice numbness or reduced sensation anywhere on your heel or arch?
- Does the discomfort stay the same or worsen the longer you stay active?
- Has your heel pain failed to respond to consistent plantar fasciitis treatment over several weeks?
Answering yes to more than one of these questions gives your clinician useful information when deciding which diagnostic steps to prioritize next.
What Baxter’s nerve entrapment pain feels like
The pain from Baxter’s nerve entrapment symptoms doesn’t follow a single script. Some patients describe a deep, persistent ache that settles into the inner heel like pressure building from the inside out. Others report sharp, sudden sensations that interrupt normal walking without any obvious trigger. What most people agree on is that the pain feels different from a typical heel ache, and that difference is often what finally sends them to a specialist after months of inconclusive treatment.
The burning and electrical sensations
Burning is the most commonly reported quality with Baxter’s nerve compression. Unlike the dull soreness that comes from fascia irritation, nerve pain carries a heat-like quality that patients frequently describe as a low-grade fire along the inside edge of the heel. That burning can stay relatively constant throughout the day or spike when pressure hits a particular spot during your gait cycle. In addition to burning, some patients report brief electrical-type flashes that shoot through the heel without warning, often lasting only a second or two but sharp enough to interrupt your stride.
The burning or electrical quality of nerve pain is one of the clearest distinguishing features that separates Baxter’s nerve compression from typical mechanical heel conditions.
Tingling and numbness can accompany the burning sensations or appear on their own. You might notice a reduced sensitivity to light touch along the heel’s inner surface, or an abnormal prickling feeling that persists even when you’re off your feet. These sensory changes happen because the compressed nerve is struggling to transmit signals normally through its path between the heel bone and surrounding soft tissue.
How intensity changes throughout the day
Unlike plantar fasciitis, which typically spikes with your first steps in the morning and then eases as your foot warms up, Baxter’s nerve pain often follows a different arc. You may feel manageable discomfort early in the day that gradually worsens with continued standing or walking. By the end of an active day, the burning and pressure can become significant enough to change how you distribute your weight, which places additional strain on surrounding structures over time.
Where the pain shows up on the heel and foot
Location is one of the most useful clues when evaluating Baxter’s nerve entrapment symptoms. The inferior calcaneal nerve runs along a specific path, and when compression occurs, the resulting pain tends to follow that path rather than spreading randomly. Understanding exactly where to expect discomfort helps you communicate your symptoms precisely and gives your clinician a better target during physical examination.
The inner heel as the primary pain site
The most common location for Baxter’s nerve compression pain is the medial heel, which is the inner side of the heel bone closest to your arch. Patients often point to a spot slightly forward and inward from the center of the heel, which is where the nerve passes through a tight channel between the abductor hallucis muscle and the quadratus plantae muscle. This location differs from plantar fasciitis, which typically concentrates at the bottom of the heel near the fascia’s attachment to the bone.
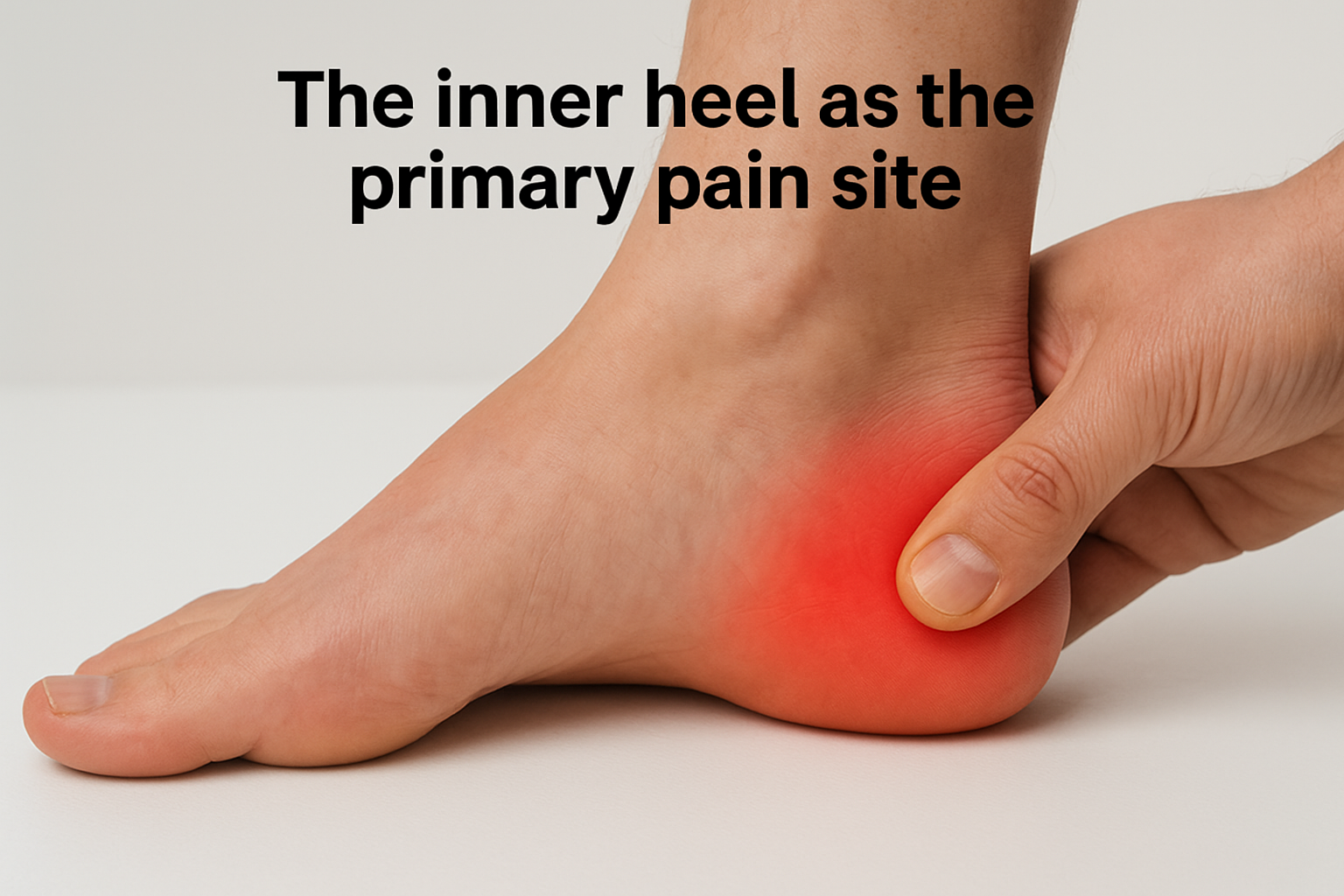
If pressing firmly along the inner edge of your heel, just below the ankle bone, reproduces your pain or a tingling sensation, that response strongly suggests nerve involvement rather than fascial irritation.
Tenderness in this zone can feel deceptively similar to a bruise or a deep bone ache, which is part of why the nerve origin gets overlooked. Applying pressure directly to the nerve’s path, rather than the broad heel pad, is what typically recreates the sensation most precisely.
How pain spreads into the arch and outer foot
Baxter’s nerve also supplies sensation to the lateral aspect of the heel, meaning the outer edge, and in some cases discomfort radiates there as well. You may notice that your pain doesn’t stay confined to one point but instead travels along the bottom of the foot toward the arch or spreads toward the outer heel border. This spread pattern reflects the nerve’s distribution and differs from plantar fasciitis, which tends to stay anchored near the heel’s base rather than radiating outward.
Some patients also report that the entire heel feels dense or heavy, as though pressure is building within the foot rather than sitting on the surface. That internal quality of the sensation is a characteristic sign of nerve compression affecting the structures deep inside the heel.
Signs and symptoms that point to Baxter’s nerve
When evaluating whether heel pain comes from nerve compression, certain features carry more diagnostic weight than others. Baxter’s nerve entrapment symptoms tend to cluster into two categories: what you feel on your own throughout the day, and what a clinician can detect during a hands-on examination. Knowing both sides of the picture helps you describe your experience accurately and gives your provider the information needed to move toward a correct diagnosis faster.
Sensory symptoms you notice on your own
The sensory signs are often the first clue that something nerve-related is happening. You may notice a burning quality that sits along the inner heel, a prickling sensation that lingers even when you sit down, or brief sharp jolts that fire through the base of the foot during normal walking. These sensory events don’t follow a predictable schedule, which is part of what makes them frustrating and hard to describe.
If your heel produces tingling or numbness at rest, rather than only during activity, a nerve source is far more likely than a structural one.
Reduced skin sensitivity along the inner heel or outer border of the foot is another self-detectable sign. You might test this by lightly running a finger across different areas of your heel and noticing whether one zone feels duller or more muted than the other side. Asymmetry in sensation between feet, even subtle asymmetry, is a meaningful finding worth reporting to your clinician.
Physical signs your clinician looks for
During a clinical examination, a trained podiatrist looks for specific responses that indicate inferior calcaneal nerve involvement. Focused pressure applied directly along the nerve’s path at the inner heel, rather than broad heel compression, often reproduces the exact burning or shooting sensation you experience during activity. That pinpoint reproduction is a strong indicator of nerve compression rather than fascial irritation.
Weakness in the small muscles of the foot can also appear over time, since Baxter’s nerve supplies the abductor digiti minimi. Your clinician may test toe and foot muscle function alongside sensory testing to build a complete picture of how far the nerve involvement has progressed.
Baxter’s nerve vs plantar fasciitis symptoms
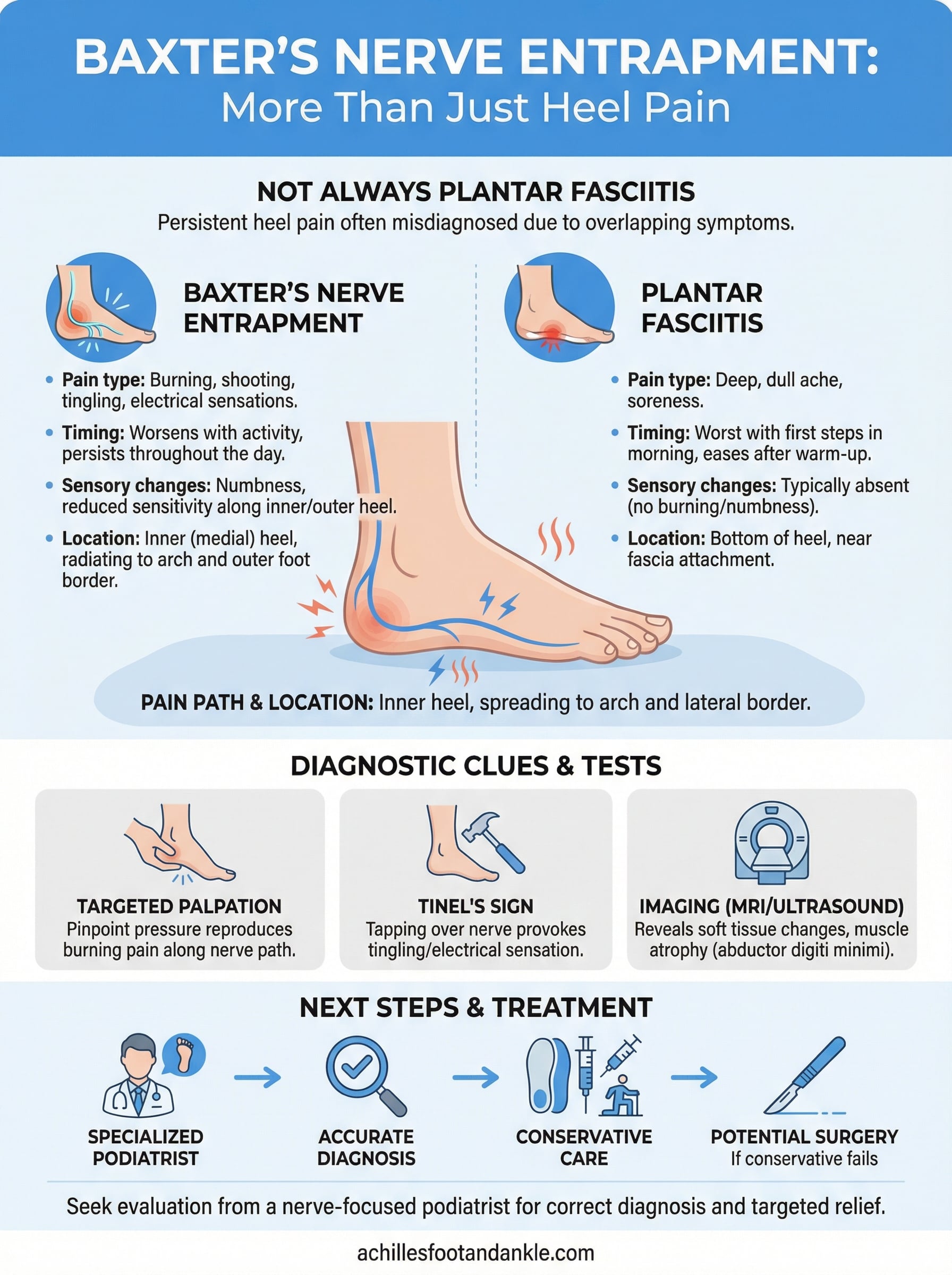
Separating these two conditions matters because their treatments differ significantly, and applying plantar fasciitis protocols to a nerve compression problem delays real recovery. Both conditions cause inner heel pain, both can worsen with activity, and both often feel worst after periods of rest. Despite those overlaps, the character of the pain and the sensory changes that accompany it reveal important differences that guide a more accurate diagnosis.
How plantar fasciitis pain behaves
Plantar fasciitis produces pain that originates at the bottom of the heel where the fascia attaches to the calcaneus, and it follows a fairly predictable pattern. The sharpest pain typically hits with your first steps after waking up or after prolonged sitting. Once your foot warms up and the fascia stretches, that pain often fades to a manageable background ache. Burning, tingling, and numbness are not standard features of plantar fasciitis, and their absence is one of the cleaner ways to distinguish fascial irritation from nerve involvement.
If your morning heel pain eases within the first several minutes of walking, plantar fasciitis remains a stronger candidate than Baxter’s nerve entrapment.
Where Baxter’s nerve entrapment symptoms diverge
Baxter’s nerve entrapment symptoms follow a pattern that doesn’t align with the warm-up improvement you see with fascia problems. Pain and burning tend to persist or worsen with continued activity rather than fading after the first few minutes of movement. You may also notice that the discomfort sits slightly higher on the inner heel, closer to where the nerve travels between the abductor hallucis and quadratus plantae muscles, rather than directly at the heel’s base.
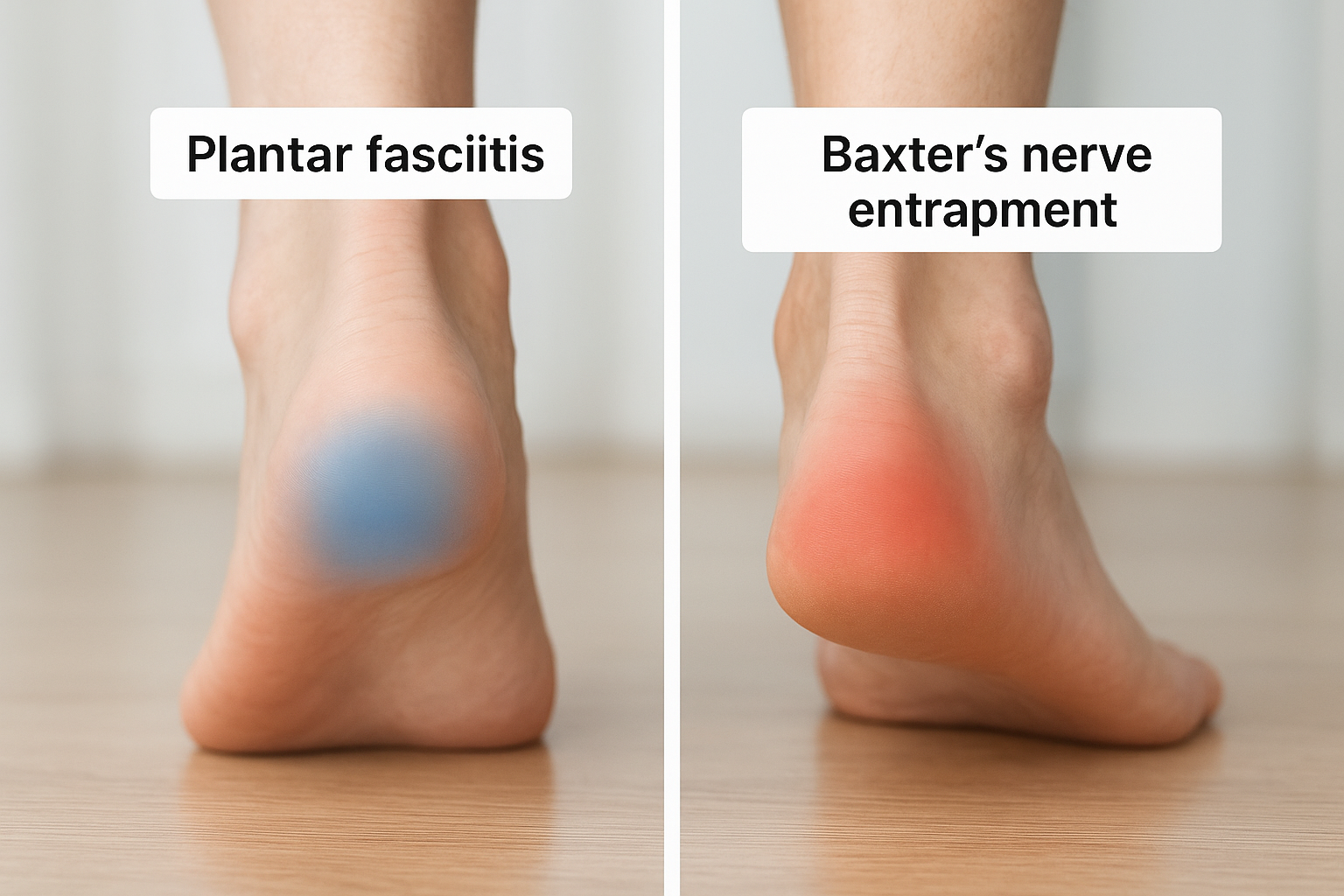
Sensory changes mark the clearest dividing line between the two conditions. Numbness, tingling, or a reduced sensitivity to touch along the inner heel or outer foot border does not occur with straightforward plantar fasciitis. When those sensory symptoms appear alongside heel pain, they shift the diagnosis toward nerve compression and away from structural fascial irritation. Reporting these details precisely during your appointment helps your clinician choose the right diagnostic path from the start.
Other conditions that can mimic these symptoms
Baxter’s nerve entrapment symptoms don’t exist in isolation on a short list of possibilities. Several other conditions produce similar inner heel pain, burning, and sensory changes, which is why reaching the right diagnosis sometimes takes multiple appointments and a methodical process of elimination. Understanding what else can generate these sensations helps you build a fuller picture of your situation before your next clinical evaluation.
Tarsal tunnel syndrome
Tarsal tunnel syndrome involves compression of the tibial nerve as it passes through a narrow channel behind the inner ankle bone, and its symptoms overlap considerably with Baxter’s nerve involvement. Both conditions can produce burning, tingling, and numbness along the inner foot, and both tend to worsen with prolonged standing or walking. The key distinction lies in the distribution of the sensory changes: tarsal tunnel syndrome typically spreads numbness and tingling across the entire sole of the foot, while Baxter’s nerve compression tends to concentrate those sensations closer to the heel and its outer border.
If burning or tingling covers your entire foot rather than staying near the heel, tarsal tunnel syndrome becomes a more likely candidate than isolated inferior calcaneal nerve compression.
Heel fat pad syndrome and stress fractures
Heel fat pad syndrome develops when the cushioning layer beneath your heel bone thins or shifts, producing a deep, bruise-like pain directly under the center of the heel. That pain can feel similar to nerve compression, but it typically lacks the burning or tingling qualities and responds to simple cushioning interventions. Calcaneal stress fractures present another mimic, generating sharp heel pain that worsens with activity and can feel vaguely similar to nerve-related discomfort during weight-bearing.
Your clinician can differentiate these conditions using a combination of targeted physical examination and imaging studies. Stress fractures often show up on MRI before they appear on plain X-ray, while fat pad atrophy is typically identifiable through careful palpation and history-taking. Separating these diagnoses from Baxter’s nerve involvement requires a structured clinical approach rather than relying on symptom descriptions alone, since the sensations produced by each condition share enough overlap to mislead an incomplete evaluation.
How clinicians test for Baxter’s nerve entrapment
Diagnosing Baxter’s nerve entrapment symptoms requires a hands-on clinical evaluation that goes beyond a general heel examination. A podiatrist trained in nerve conditions approaches the assessment with specific maneuvers designed to isolate the inferior calcaneal nerve rather than simply confirming that your heel hurts when pressed broadly. Knowing what to expect during this evaluation helps you participate more actively in the process and communicate your response to each test with more precision.
Targeted palpation along the nerve’s pathway
Your clinician begins by pressing firmly along the medial heel, tracing the nerve’s course between the abductor hallucis and quadratus plantae muscles. This targeted palpation differs from general heel compression because the clinician is looking for a very specific response at the nerve’s location rather than widespread tenderness across the heel pad. If that pressure reproduces your familiar burning or shooting sensation, the result provides a meaningful clinical indicator pointing toward nerve compression rather than fascial irritation.
Reproducing your exact symptom with pinpoint pressure along the nerve’s path is one of the strongest clinical indicators of Baxter’s nerve entrapment available without imaging.
Your clinician will also compare the tenderness pattern on your symptomatic side versus your unaffected foot, since asymmetry in how each heel responds to the same pressure adds useful diagnostic weight to the overall picture.
Tinel’s sign and muscle strength assessment
Tinel’s sign involves tapping directly over the compressed nerve to provoke a tingling or electrical sensation traveling into the foot. A positive Tinel’s response at the inner heel suggests that the inferior calcaneal nerve is irritated at that specific point, and it helps distinguish nerve compression from other structural heel problems.
Your clinician will also test the strength of the abductor digiti minimi, the small muscle that Baxter’s nerve supplies at the outer edge of the foot. Measurable weakness in that muscle compared to the opposite side indicates that nerve compression has progressed to a point where motor function is affected, which factors into both your diagnosis and the recommended treatment approach.
What imaging and nerve tests can show
Imaging and nerve testing play a supporting role in confirming a clinical diagnosis of Baxter’s nerve entrapment. Physical examination typically guides the initial diagnosis, but imaging adds precision when the picture remains unclear or when your clinician needs to rule out overlapping conditions before deciding on treatment. Understanding what each test can and cannot detect helps you set realistic expectations for the diagnostic process.
MRI and ultrasound findings
MRI is the most valuable imaging tool for evaluating Baxter’s nerve entrapment symptoms because it can reveal soft tissue changes that plain X-rays miss entirely. On MRI, your clinician looks for fatty infiltration or atrophy within the abductor digiti minimi muscle, which signals that the nerve supplying it has been compressed long enough to affect the muscle itself. That finding confirms nerve involvement even when the compression site doesn’t appear dramatically abnormal on imaging.
Muscle atrophy visible on MRI indicates that nerve compression has been present long enough to affect motor function, which often influences how aggressively your clinician approaches treatment.
Diagnostic ultrasound offers a different advantage because it allows real-time assessment of the nerve’s path and the surrounding soft tissue. Your clinician can visualize the channel where compression occurs, identify any thickening or structural abnormality near the nerve, and use ultrasound guidance to place a diagnostic injection precisely at the site. A significant reduction in your pain following that injection strongly confirms the diagnosis by demonstrating that the inferior calcaneal nerve is the source of the problem.
Electrodiagnostic testing
Nerve conduction studies and electromyography, commonly called EMG, measure how well electrical signals travel through the nerve and into the muscles it supplies. In cases of Baxter’s nerve compression, these tests may detect slowed conduction velocity or abnormal muscle responses in the outer foot. However, electrodiagnostic testing produces false negatives in a meaningful number of cases, so a normal result doesn’t eliminate nerve entrapment as the diagnosis. Your clinician interprets these findings alongside your symptoms, physical examination responses, and imaging results rather than relying on any single test in isolation.
What to do next and common treatment options
If your symptoms align with what this article has described, the most important next step is getting a proper diagnosis from a podiatrist who specifically evaluates for nerve compression, not just general heel pain. Attempting to treat Baxter’s nerve entrapment symptoms with generic plantar fasciitis protocols on your own will not address the nerve compression, and repeated failed treatments often allow the condition to progress further before you receive accurate care.
Conservative treatment approaches
Most cases respond well to non-surgical interventions when identified at an earlier stage, which gives you a strong reason to seek evaluation sooner rather than waiting for symptoms to intensify. Your podiatrist will typically begin with approaches designed to reduce compression around the nerve and decrease local inflammation.
Starting with conservative care gives most patients meaningful relief without requiring surgical intervention, provided the nerve has not sustained prolonged damage.
Common conservative options include:
- Custom orthotics that redistribute pressure away from the nerve’s path at the inner heel
- Corticosteroid injections placed under ultrasound guidance directly at the compression site
- Activity modification to reduce repetitive pressure on the heel during the recovery period
- Physical therapy focusing on stretching the intrinsic foot muscles and reducing tightness in the structures surrounding the nerve
- Supportive footwear that offloads the medial heel and reduces mechanical stress throughout your gait cycle
When surgery becomes the right option
Some patients reach a point where conservative measures have been exhausted without sufficient relief, and at that stage, surgical release of the nerve becomes a legitimate option. The procedure involves releasing the tight tissue that compresses the inferior calcaneal nerve, which directly addresses the mechanical source of entrapment rather than managing symptoms around it.
Recovery timelines vary depending on how long the nerve compression has been present and whether muscle atrophy has developed. Your podiatrist will evaluate the extent of nerve involvement using the imaging and clinical findings gathered during your diagnostic workup to determine whether conservative care remains appropriate or whether surgical intervention gives you the better path forward.
A simple way to move forward
Recognizing Baxter’s nerve entrapment symptoms puts you in a much stronger position than most patients who spend months treating the wrong problem. You now know what the pain feels like, where it shows up, how it differs from plantar fasciitis, and what a proper clinical evaluation involves. That knowledge matters because it helps you describe your experience accurately and ask the right questions during your appointment rather than walking out with another round of generic heel pain treatment.
Your next step is straightforward. If your heel pain burns, tingles, or hasn’t responded to standard treatment, seeing a podiatrist who specifically evaluates for nerve compression is the most direct path to answers. Achilles Foot and Ankle Center serves patients across thirteen Central Virginia locations, with advanced diagnostic tools and same-day availability when you need it. Book a same-day appointment and get a clear diagnosis rather than another round of guessing.






