Charcot foot can transform a minor injury into a serious, limb-threatening condition, often without any pain to warn you. This progressive disorder weakens bones in the foot to the point where they fracture and collapse, potentially leading to severe deformity or amputation. Understanding Charcot foot risk factors is the first step toward protecting yourself or someone you care about from this devastating complication.
Not everyone faces the same level of risk. Certain medical conditions, particularly long-standing diabetes and peripheral neuropathy, dramatically increase susceptibility. Other factors, like previous foot injuries, obesity, and even kidney disease, can compound that risk in ways many patients don’t expect. Recognizing these vulnerabilities early gives you and your medical team the opportunity to intervene before permanent damage occurs.
At Achilles Foot and Ankle Center, our podiatrists regularly diagnose and treat Charcot foot across our Central Virginia locations. We’ve seen firsthand how early identification of risk factors changes outcomes for our patients, especially those managing diabetes or chronic neuropathy. This article breaks down exactly who faces the greatest risk for Charcot foot, why these factors matter, and what warning signs to watch for, so you can take action before a small problem becomes a major one.
Why Charcot foot risk factors matter
Understanding your vulnerability to Charcot foot can mean the difference between keeping your mobility and facing amputation. This condition progresses rapidly once it starts, often causing irreversible bone damage within weeks if left untreated. When you know your risk level, you and your doctor can monitor your feet more closely, catch early warning signs, and intervene before fractures cascade into deformity. Most patients who develop Charcot foot had identifiable risk factors for months or years before their diagnosis, yet many never received targeted screening or education about what to watch for.
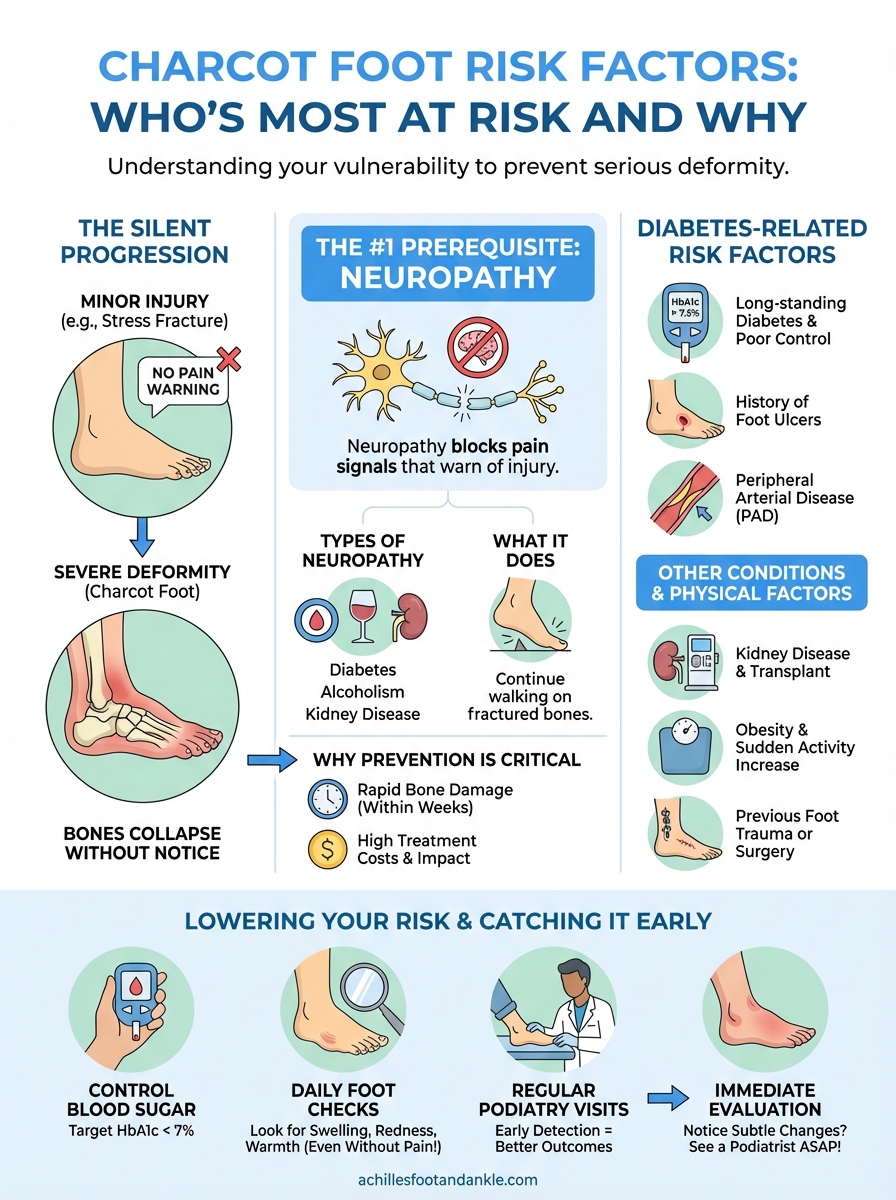
The silent progression that makes prevention critical
Charcot foot develops without the pain signals that normally alert you to injury. You might walk on a fractured bone for days or weeks because neuropathy blocks the warning system your body relies on for protection. This lack of sensation allows minor trauma to spiral into major structural collapse before you even realize something is wrong. Your foot may swell, redden, or feel warm to the touch, but these subtle changes often get mistaken for infection or a simple sprain until X-rays reveal extensive bone damage that could have been prevented.

The progression happens faster than most people expect. A small stress fracture in someone with normal sensation would cause immediate pain and trigger protective behavior like limping or resting. In a patient with high-risk factors, that same fracture continues accumulating force with every step, causing additional bones to break and joints to dislocate. Within four to six weeks, the foot’s architecture can collapse to the point where reconstruction becomes the only option beyond amputation.
Early recognition of risk factors and subtle symptoms can prevent 80% of Charcot foot complications, yet most cases still get diagnosed after significant deformity has occurred.
The financial and physical consequences of late diagnosis
Treatment costs escalate dramatically as Charcot foot progresses through its stages. Catching the condition during the acute inflammatory phase typically requires immobilization in a total contact cast for several months, which is inconvenient but preserves your foot structure. Missing that window often means facing reconstructive surgery with hardware implantation, extended non-weight-bearing periods, and potential complications that can stretch treatment timelines beyond a year. Some patients require multiple revision surgeries when initial interventions fail to stabilize a severely deformed foot.
Beyond the financial burden, late-stage Charcot foot transforms daily life in ways that extend far beyond the affected limb. You may lose your ability to work, drive, or maintain independence during prolonged treatment phases. The emotional toll of facing potential amputation, combined with the physical challenge of months in a wheelchair or walker, affects mental health and family dynamics. Your overall health often declines as immobility contributes to weight gain, cardiovascular deconditioning, and depression.
Knowing your Charcot foot risk factors empowers you to take protective action before any of these consequences materialize. Regular self-examination becomes second nature when you understand what you’re watching for. You schedule podiatry appointments at appropriate intervals rather than waiting until something feels wrong. This proactive approach, guided by awareness of your specific vulnerabilities, gives you the best chance of maintaining healthy, functional feet for life.
The one risk factor Charcot foot needs: neuropathy
Neuropathy serves as the essential prerequisite for Charcot foot development. Without nerve damage that blocks pain signals, your body’s natural protective mechanisms would stop you from walking on injured bones before serious damage occurs. Every documented case of Charcot foot involves some degree of peripheral neuropathy that stripped away the sensory feedback your feet normally provide. This explains why the condition remains relatively rare despite millions of people having diabetes or other risk factors, because neuropathy must be present before Charcot foot risk factors can actually trigger the destructive cascade.
What neuropathy does to your protective reflexes
Your nervous system typically guards against injury through an immediate pain response that forces you to stop harmful activities. When you step on a sharp object or twist your ankle, pain signals travel from your foot to your brain in milliseconds, triggering automatic protective behaviors like limping, weight shifting, or complete avoidance of the injured area. This feedback loop prevents minor injuries from becoming major ones by giving damaged tissues time to heal.
Neuropathy disrupts this protective system by damaging the sensory nerves that carry pain, temperature, and pressure information from your feet to your brain. You might fracture a bone during routine walking and feel nothing more than mild discomfort or warmth. Without pain to guide you, you continue placing full weight on compromised bones and joints, causing fractures to propagate, joints to dislocate, and the foot’s structure to collapse. The injury that should have prompted immediate medical attention instead goes unnoticed until visible deformity appears.
Patients with advanced neuropathy often discover Charcot foot only after noticing their shoe fits differently or someone else points out obvious swelling.
Types of neuropathy that increase your risk
Diabetic peripheral neuropathy represents the most common pathway to Charcot foot, affecting roughly 50% of people who have had diabetes for 25 years or longer. This specific nerve damage typically starts in the toes and gradually progresses up the foot and leg in a stocking pattern. Other conditions can produce similar sensory loss, including chronic alcoholism, vitamin B12 deficiency, Charcot-Marie-Tooth disease, and certain autoimmune disorders. Regardless of the underlying cause, any neuropathy severe enough to eliminate protective pain sensation in your feet creates the foundation for Charcot foot to develop when combined with additional trauma or stress.
Diabetes-related risk factors that raise your odds
Diabetes doesn’t automatically guarantee you’ll develop Charcot foot, but specific diabetes-related factors significantly increase your vulnerability beyond just having the diagnosis. The duration of your diabetes and how well you’ve controlled your blood sugar over the years determine your actual risk level more than your current blood glucose reading. Patients who’ve lived with diabetes for 10 years or longer face substantially higher odds, especially if they’ve developed diabetic neuropathy during that time. Your risk compounds when multiple diabetes complications exist simultaneously, creating a perfect storm for Charcot foot development.
Duration of diabetes and glycemic control
Every year you live with diabetes increases your cumulative exposure to elevated blood sugar levels that damage nerves and blood vessels in your feet. Research shows Charcot foot rarely develops in patients who’ve had diabetes for fewer than five years, but becomes progressively more common after the 10-year mark. Your long-term blood sugar control, measured through HbA1c tests, directly correlates with neuropathy severity and subsequent Charcot foot risk. Patients with consistently high HbA1c levels (above 7.5%) over many years suffer more nerve damage than those maintaining tighter control, making poor glycemic management one of the most modifiable Charcot foot risk factors under your direct influence.
Maintaining an HbA1c below 7% throughout your life with diabetes can reduce neuropathy progression by up to 60%, substantially lowering your Charcot foot risk.
Type 1 diabetes carries slightly higher Charcot foot risk than Type 2 because patients typically develop it earlier in life, accumulating more total years of exposure to glucose fluctuations. Your pancreas produces no insulin in Type 1 diabetes, making blood sugar management more volatile and challenging even with excellent self-care.
Diabetes complications that multiply your risk
Previous diabetic foot ulcers signal severely compromised foot health and dramatically elevate your Charcot foot susceptibility. Ulcers demonstrate that you’ve already experienced neuropathy severe enough to allow tissue damage without pain, the exact mechanism Charcot foot requires. Peripheral arterial disease (PAD), another common diabetes complication, restricts blood flow to your feet and impairs bone healing capacity after fractures occur. When you combine neuropathy with reduced circulation, even minor trauma can trigger the bone destruction cascade that characterizes Charcot foot development.
Diabetic kidney disease (nephropathy) correlates with increased Charcot foot incidence, possibly because similar metabolic processes damage both organs simultaneously. Retinopathy creates vision problems that prevent you from noticing early foot swelling or changes that might otherwise prompt medical attention.
Other conditions and factors linked to Charcot foot
While diabetes causes the majority of Charcot foot cases, several other medical conditions and physical factors can create similar vulnerability. Any disease or circumstance that damages your peripheral nerves or compromises your foot’s structural integrity qualifies as a potential trigger. Understanding these alternative pathways helps you recognize your risk even if you don’t have diabetes, and alerts your healthcare team to monitor your feet more closely when multiple charcot foot risk factors converge in your medical history.
Non-diabetic conditions that damage nerves
Chronic alcohol abuse ranks as the second most common cause of the neuropathy required for Charcot foot development. Heavy drinking over many years destroys peripheral nerves through both direct toxic effects and nutritional deficiencies, particularly thiamine (vitamin B1) depletion. Your risk increases substantially if you’ve consumed excessive alcohol for a decade or longer, especially when combined with poor nutrition that accelerates nerve damage.
Kidney disease, whether from diabetes or other causes, allows metabolic waste products to accumulate in your bloodstream and damage nerves throughout your body. Patients on dialysis or with advanced chronic kidney disease face elevated Charcot foot risk, particularly if they’ve also undergone kidney transplantation. The immunosuppressive medications required after transplant surgery can impair bone healing and increase fracture susceptibility, compounding the neuropathy that already exists from kidney failure.
Organ transplant recipients taking corticosteroids and immunosuppressants face three times the normal risk of developing Charcot foot during the first two years post-transplant.
Physical and mechanical risk factors
Previous foot trauma or surgery creates localized weakness that makes your bones more vulnerable to collapse. You might develop Charcot foot years after a severe ankle fracture, foot surgery, or traumatic injury that altered your foot’s normal architecture. These old injuries leave behind structural compromises that become apparent only when combined with neuropathy that prevents you from protecting the weakened area.

Obesity significantly increases the mechanical stress your feet absorb with every step, multiplying fracture risk when neuropathy blocks pain signals. Carrying excess body weight forces your foot bones to bear loads they weren’t designed to handle, particularly if you’ve gained substantial weight rapidly. Sudden increases in activity level, like starting a new exercise program or changing jobs to one requiring extended standing, can also trigger Charcot foot in patients with underlying neuropathy who suddenly subject their feet to unaccustomed mechanical demands.
How to lower your risk and catch it early
Reducing your Charcot foot vulnerability requires addressing the modifiable risk factors you can control while staying alert for early warning signs that demand immediate medical attention. Your most powerful prevention tool is consistent management of the underlying conditions that cause neuropathy, particularly tight blood sugar control if you have diabetes. Catching Charcot foot during its earliest stages, when your foot shows subtle changes before significant bone damage occurs, dramatically improves your treatment outcomes and preserves your mobility.
Control your blood sugar and manage underlying conditions
Maintaining your HbA1c below 7% represents the single most effective strategy for slowing neuropathy progression and reducing charcot foot risk factors over your lifetime. Work with your endocrinologist to optimize your diabetes medications, adjust your insulin regimen as needed, and implement consistent monitoring habits that prevent dangerous blood sugar fluctuations. If you struggle with glycemic control despite medication, ask about continuous glucose monitors or insulin pumps that provide more precise management than traditional methods.
Address other contributing conditions with equal urgency. Limit alcohol consumption to prevent or reverse alcohol-related neuropathy, supplement vitamin B12 if you’re deficient, and work with your nephrologist to optimize kidney function through medication and dietary changes. Losing excess weight reduces mechanical stress on your foot bones and often improves diabetes control simultaneously, creating a dual protective effect against Charcot foot development.
Perform daily foot checks and monitor for warning signs
Inspect both feet every evening for subtle changes that might indicate early Charcot foot, including mild swelling, redness, warmth, or areas that appear different from the day before. Use a mirror to examine your soles if you can’t see them directly, or ask a family member to check for you. Temperature differences between your feet, even if both feel normal to you, can signal the inflammation that precedes bone collapse.
Any unexplained swelling, warmth, or redness in your foot requires immediate evaluation by a podiatrist, even without pain, because these symptoms may represent acute Charcot foot in its most treatable stage.
Schedule regular podiatry appointments every three to six months if you have diabetes and neuropathy, allowing your doctor to detect problems you might miss during self-examinations. Report any new foot injuries immediately rather than waiting to see if they heal on their own.
Next steps for protecting your feet
Understanding charcot foot risk factors means taking immediate action based on your current situation. If you have diabetes with neuropathy, schedule a comprehensive foot examination with a podiatrist today, even if your feet currently appear normal. This baseline assessment establishes a personalized monitoring protocol tailored to your specific vulnerabilities and catches developing problems before symptoms appear.
Notice any swelling, redness, warmth, or shape changes in either foot? You need immediate evaluation regardless of whether you feel pain. These subtle indicators might represent acute Charcot foot in its most treatable stage, where proper immobilization can prevent permanent deformity and preserve your mobility.
At Achilles Foot and Ankle Center, we help patients across Central Virginia through early intervention and comprehensive risk assessment. Our experienced team uses advanced imaging technology to identify Charcot foot before catastrophic collapse occurs. Schedule a same-day appointment if you’re experiencing any foot changes or need a preventive evaluation.






