Diabetes affects roughly 37 million Americans, and one of its most underestimated consequences happens from the ankles down. Nerve damage and reduced blood flow can turn a small blister or cut into a serious infection, sometimes before you even feel it. That’s why foot care tips for diabetics aren’t optional extras; they’re a daily necessity. The good news? Most diabetic foot complications are preventable with the right habits.
At Achilles Foot and Ankle Center, our podiatrists treat diabetic foot problems across Central Virginia every day, from early-stage neuropathy to advanced wound care and limb salvage. We’ve seen what works and what gets overlooked. This article breaks down five daily habits that protect your feet, keep small issues from becoming big ones, and help you stay active and on your feet for the long run.
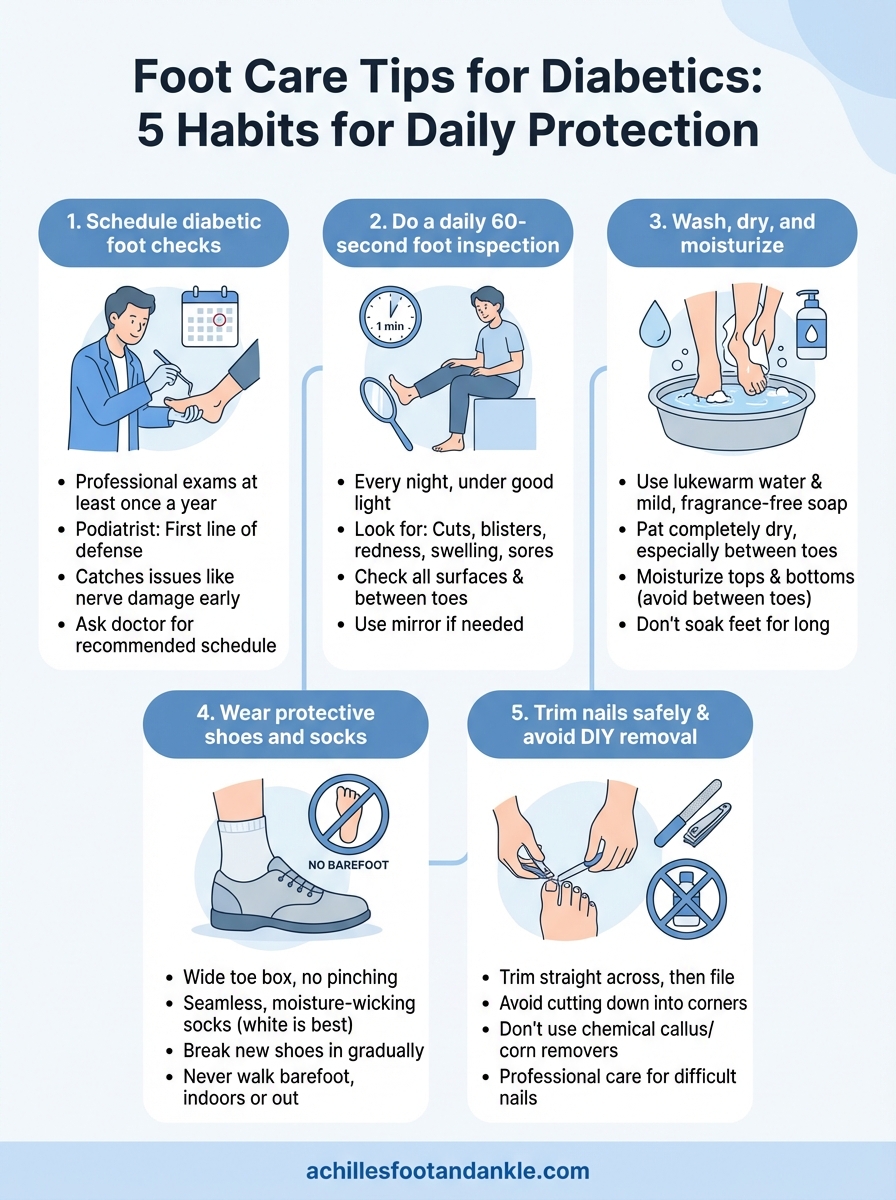
1. Schedule diabetic foot checks with a podiatrist
A podiatrist is your first line of defense against serious diabetic foot complications. Even if your feet feel fine right now, nerve damage can mask pain signals entirely, which means problems can develop without any obvious warning. Professional exams catch what daily self-checks miss.
Why diabetic foot exams prevent small issues from escalating
When circulation is reduced, your body struggles to heal even minor cuts, blisters, or calluses. A podiatrist identifies these issues before they worsen, checking for nerve function loss, circulation problems, and structural changes that you cannot assess on your own. Early detection at this stage makes treatment significantly faster and simpler.
Undetected foot ulcers are the leading cause of diabetes-related lower-limb amputations in the United States, and the majority of those amputations are preventable with routine professional care.
How often to get foot checks and what changes that schedule
Most people with diabetes need a professional foot exam at least once a year. If you already have neuropathy, poor circulation, or a history of foot ulcers, your podiatrist may recommend visits every one to three months. Your overall blood sugar control also affects how frequently you should be seen, so ask your doctor directly.
What to expect during a diabetic foot visit
Your podiatrist will assess several areas during a standard diabetic foot exam:
- Skin and nail condition for wounds, infections, or thickening
- Nerve sensation using a simple filament test
- Blood flow through pulse checks or Doppler testing
- Joint alignment and gait for pressure point risks
The visit typically takes under 30 minutes, and you’ll leave with specific recommendations tailored to your current foot health.
When to call for a same-day appointment
Following these foot care tips for diabetics also means knowing when not to wait. Contact your podiatrist the same day you notice an open sore, unusual swelling, warmth, or skin discoloration. These signs can escalate fast when blood flow is compromised. Achilles Foot and Ankle Center offers same-day appointments for urgent diabetic foot concerns across Central Virginia.
2. Do a daily 60-second foot inspection
A daily inspection takes less than a minute and is one of the most practical foot care tips for diabetics you can adopt. Look at your feet every night before bed, ideally in good lighting.

What to look for during your daily check
Check both feet for cuts, blisters, redness, swelling, or sores. Pay close attention to skin color changes, unusual warmth, or odor, which can signal infection even when you feel no pain at all.
Because diabetic nerve damage can eliminate pain entirely, a visual check is often the only way to catch a problem before it worsens.
How to check your feet if you have limited mobility
Use a long-handled mirror to view your soles if bending is difficult. A family member or caregiver can also help you inspect areas that are hard to see, including the heels and between the toes.
How to track changes with simple notes and photos
Take a quick photo of any new mark or discoloration with your phone. Keeping a simple log helps your podiatrist compare changes between visits and respond faster if something is progressing.
Red flags that mean you should call your doctor today
Contact your podiatrist immediately if you notice an open wound, black or blue skin, unusual swelling, or streaking redness. These symptoms can escalate quickly when circulation is reduced, so same-day care is often necessary.
3. Wash, dry, and moisturize the right way
Daily hygiene is one of the most overlooked foot care tips for diabetics, yet it directly shapes your infection risk and skin condition. A consistent routine protects the skin barrier your feet depend on.
The safest way to wash your feet without burns or irritation
Use lukewarm water only, since neuropathy can prevent you from sensing burns. Wash gently with mild, fragrance-free soap, and keep soak time under five minutes to avoid breaking down skin.
How to dry thoroughly, especially between toes
Pat your feet completely dry with a soft towel after washing. Give extra attention to the spaces between your toes, where retained moisture creates the ideal environment for fungal infections.
Skipping this step is one of the most common causes of athlete’s foot and bacterial infections in diabetic patients.
Pay close attention to any area that stays damp or red, as that signals a problem worth mentioning to your podiatrist.
How to moisturize without raising infection risk
Apply a fragrance-free moisturizer to the tops and bottoms of your feet daily. Skip the area between your toes, since lotion there traps moisture and raises infection risk.
What to do about cracks, itching, odor, or peeling skin
These symptoms point to underlying skin problems that need professional evaluation. Contact your podiatrist if you notice:
- Cracked heels that deepen or bleed
- Persistent itching or peeling between toes
- Odor that continues after washing
Avoid home remedies, since compromised skin in diabetic patients can progress to infection fast.
4. Wear protective shoes and socks every day
Footwear is one of the most practical foot care tips for diabetics that people overlook daily. Bare feet, loose shoes, or rough seams can create pressure points and wounds that your nerves may never register.
A simple checklist for proper shoe fit and toe room
Your shoes need a wide toe box with at least a thumb’s width of space at the front. Check that no part of the shoe pinches or creates uneven pressure along the sides or heel.

- Toe box: wide enough for all toes to lie flat
- Heel: snug without slipping
- Insole: smooth with no raised seams
How to choose socks that manage moisture and reduce rubbing
Pick seamless, moisture-wicking socks made from cotton or wool blends. Avoid tight elastic bands, which restrict circulation in an already compromised system.
White socks make it easier to spot early drainage or blood from a wound you might not feel.
How to buy and break in shoes without causing blisters
Shop for shoes later in the day when your feet are at their most swollen. Break new shoes in gradually over one to two weeks, wearing them for short periods before committing to a full day.
Common footwear mistakes to avoid at home and outdoors
Never walk barefoot indoors or outside, since floors hide sharp objects. Avoid sandals, flip-flops, and open-toe shoes that leave skin exposed or create friction along the edges.
5. Trim nails safely and avoid DIY corn and callus removal
Nail trimming and skin care require extra caution when you have diabetes. Small cuts from improper technique or chemical treatments can open the door to infections that heal slowly or not at all.
How to trim toenails to reduce ingrown nails and cuts
Cut your nails straight across and file any sharp edges gently with an emery board. Avoid cutting down into the corners, which increases the risk of ingrown nails and skin breaks.
Cutting nails too short is one of the most frequent causes of diabetic foot infections that begin as minor wounds.
- Trim in good light so you can see the full nail edge clearly
- File after cutting to smooth any rough points that can snag on socks
Tools and hygiene basics to lower infection risk
Use clean, sharp nail clippers each time you trim. Wipe your tools with rubbing alcohol before and after use to prevent bacteria from entering any small nicks in the skin.
What not to use on calluses, corns, and thick nails
Skip medicated corn pads and liquid callus removers entirely. These products contain acids that damage surrounding healthy skin, which puts you at direct risk for ulcers and slow-healing wounds.
When professional nail and callus care matters most
As one of the essential foot care tips for diabetics, professional trimming matters most when nails are thick, curved, or too painful to manage safely on your own. A podiatrist removes calluses and trims nails with sterile tools and clinical precision, reducing your risk at every visit.
Protect your feet starting today
These five foot care tips for diabetics work because they’re simple enough to do every day and specific enough to catch problems early. Daily inspection, proper hygiene, the right footwear, safe nail care, and regular podiatrist visits form a routine that directly reduces your risk of serious complications, most of which are preventable with consistent effort.
Staying consistent with these habits gives your feet the best chance of staying healthy even when circulation and nerve function are compromised. Small daily actions add up to real protection over time, and most take under a minute to complete.
Your podiatrist is your strongest partner in this process. If you haven’t scheduled a diabetic foot exam recently, or if something caught your attention during your last self-check, don’t wait. Book a same-day diabetic foot appointment with the team at Achilles Foot and Ankle Center and get the professional evaluation your feet need today.






