A mallet toe definition comes down to one specific joint: the distal interphalangeal (DIP) joint at the tip of the toe bends downward and stays there. This creates a permanent curl at the end of the toe, often pressing the tip into the ground or against the inside of your shoe. It’s a condition that gets confused with hammertoe and claw toe regularly, but the joint involved and the shape of the deformity are distinctly different, and knowing the difference matters for treatment.
At Achilles Foot and Ankle Center, our podiatrists across Central Virginia diagnose and treat mallet toes at every stage, from early flexibility issues to rigid deformities that require surgical correction. We see this condition frequently in our clinics, and one thing stands out: most patients wait too long to get it evaluated, often because they assumed it was just a minor cosmetic issue.
This article breaks down exactly what mallet toe is, what causes it, the symptoms to watch for, and the full range of treatment options, from conservative approaches to surgery, so you can make an informed decision about your next step.
Why mallet toe matters
A mallet toe that starts out flexible and painless can quietly become a rigid, painful deformity over months or years. Many people dismiss it early because the toe still bends, there’s no open wound, and it doesn’t interfere much with walking yet. That delay is exactly what turns a straightforward conservative treatment into a more complex and costly surgical case.
It progresses from flexible to rigid
When a mallet toe is still flexible, the joint responds to manual pressure and straightens temporarily. At this stage, splinting, padding, and footwear adjustments can often correct the deformity or slow its progression significantly. Once the joint stiffens and the deformity becomes rigid, those conservative options lose their effectiveness and surgery becomes the more likely path forward.
The earlier you address a mallet toe, the more treatment options remain available to you.
The shift from flexible to rigid does not follow a fixed timeline. Footwear choices, activity level, and underlying conditions such as diabetes or arthritis can all accelerate the process considerably, which is why regular monitoring matters once you notice the first signs.
The complications go beyond discomfort
Understanding the full mallet toe definition includes recognizing what happens when the condition goes untreated. The bent tip of the toe creates constant pressure and friction against the inside of your shoe, which leads to corns, calluses, and in more serious cases, open wounds. For patients with diabetes or circulation problems, those wounds carry a real risk of infection and significantly delayed healing that can threaten the toe itself.
Pain during walking is another consequence that builds gradually. What starts as mild soreness at the tip of the toe can develop into pain that alters your gait entirely, eventually straining your knees, hips, and lower back as your body compensates with every step. That chain of secondary problems is a primary reason podiatrists take this condition seriously from the very first visit.
How to identify mallet toe
Understanding the full mallet toe definition starts by looking at the tip of the toe. A mallet toe creates a visible downward curl at the DIP joint (the last joint before the toenail), while the rest of the toe stays relatively straight. This distinguishes it clearly from hammertoe, which bends at the middle joint, and claw toe, which bends at multiple joints at once.
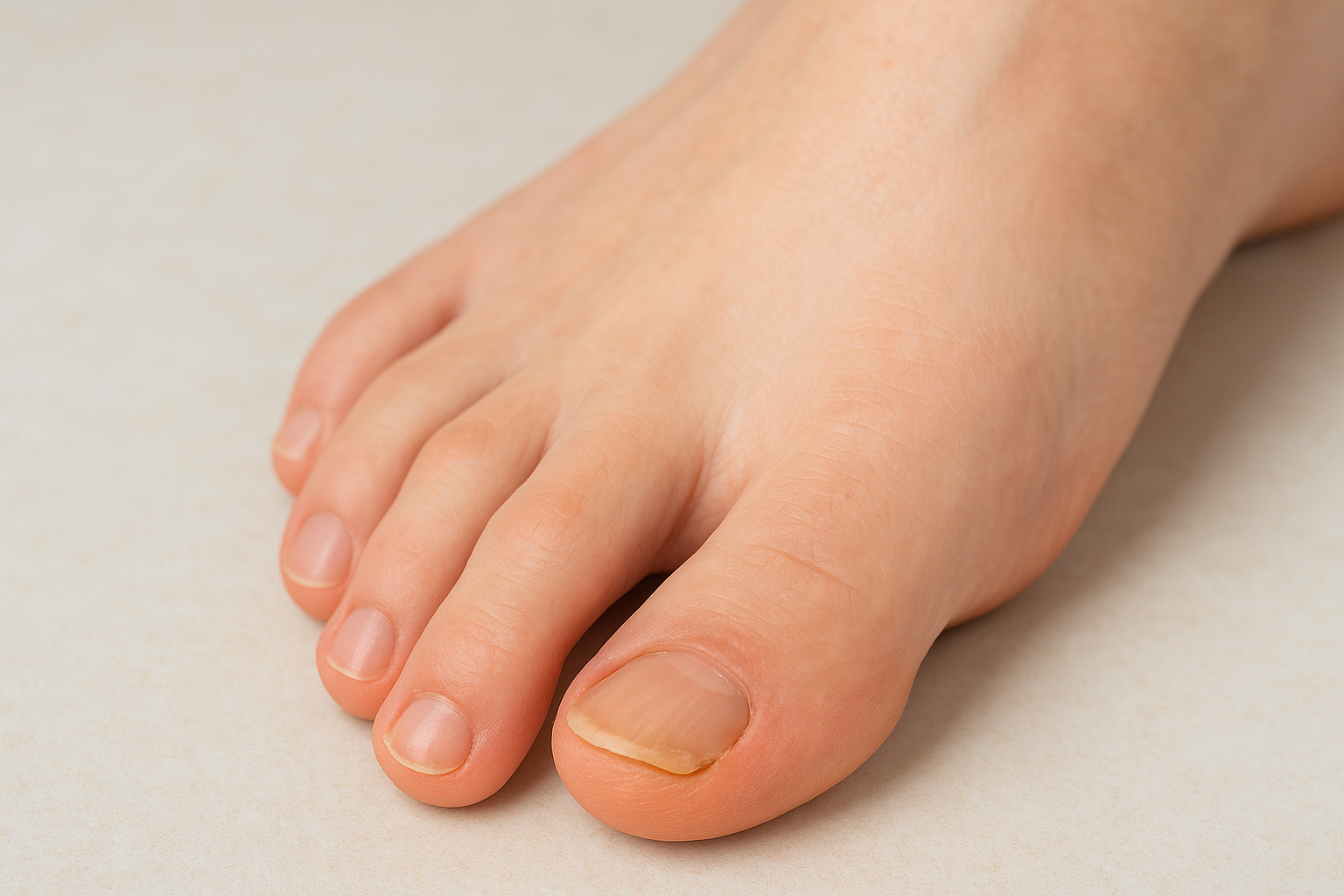
The physical appearance
When you examine the affected toe, you’ll notice the tip pointing downward rather than lying flat. The toenail often presses into the ground when you stand barefoot, and the skin at the tip can develop thickened, hardened tissue from repeated friction inside your shoe. The second toe is most commonly affected, but mallet toe can develop on any of the four smaller toes.
Symptoms you may feel
Pain and tenderness at the tip of the toe are the most reported symptoms, particularly during walking or in closed shoes. A corn often forms directly on the tip where shoe contact is greatest, which is a reliable indicator that something structural is happening with that joint.
If your toe tip is consistently sore after a normal day of walking, that symptom warrants professional evaluation rather than more padding.
Redness and swelling around the DIP joint can also appear, especially after extended physical activity, as inflammation builds in the affected area.
What causes mallet toe and who gets it
The full mallet toe definition includes understanding why the DIP joint bends downward in the first place. In most cases, the cause comes down to an imbalance between the tendons and muscles that control the toe, which forces the joint into a downward position over time.
The structural and lifestyle causes
Footwear is the most common contributing factor. Shoes that crowd the toes, especially narrow-toed shoes or high heels that push the foot forward, force the toes into a bent position for hours at a time. Over years, that repeated pressure gradually shortens the tendons and locks the joint in a flexed position. Toe injuries, including stubbed toes and fractures that do not heal in proper alignment, can also trigger the deformity.
Wearing shoes with adequate toe box depth is one of the most practical ways to reduce your risk of developing mallet toe.
Who is most at risk
People with longer second toes face a higher mechanical risk because the toe has more contact with the front of the shoe. Arthritis weakens the joint structures and accelerates deformity formation, and diabetic neuropathy is a significant risk factor because nerve damage reduces your ability to feel the early warning signs. Women develop mallet toe more frequently than men, largely due to prolonged use of constrictive footwear.
How podiatrists diagnose mallet toe
Diagnosis starts with a physical examination of your foot and ankle. Your podiatrist will look at the affected toe while you’re both standing and seated, checking the shape and position of the DIP joint and testing whether the deformity is still flexible or has become rigid. That distinction directly shapes which treatment path makes the most sense for your case.
The physical examination
Your podiatrist will apply gentle manual pressure to the tip of the toe to see whether the joint straightens at all. A flexible mallet toe responds to that pressure; a rigid one does not. They’ll also inspect the surrounding skin for corns, calluses, or open wounds that indicate how long the deformity has been active and how much friction your shoe has been generating.
The flexibility or rigidity of the DIP joint is one of the most clinically significant findings in any mallet toe evaluation.
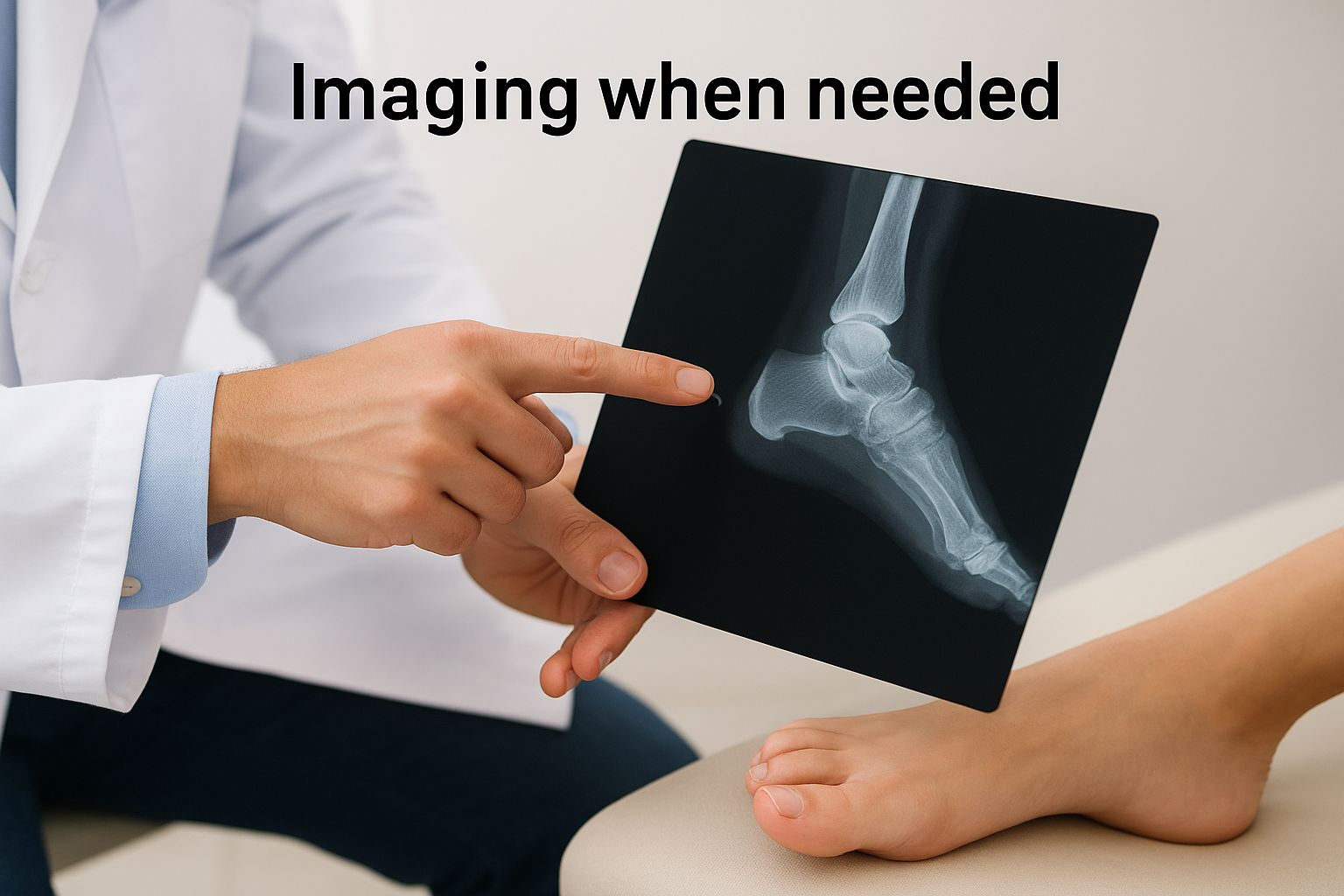
Imaging when needed
When the mallet toe definition in your case involves significant pain, suspected bone changes, or a prior injury, your podiatrist will order X-rays to get a clearer picture. X-rays reveal joint alignment, bone quality, and any arthritic changes that are not visible during a physical exam alone. This information helps your podiatrist plan the most appropriate treatment before recommending any specific procedure.
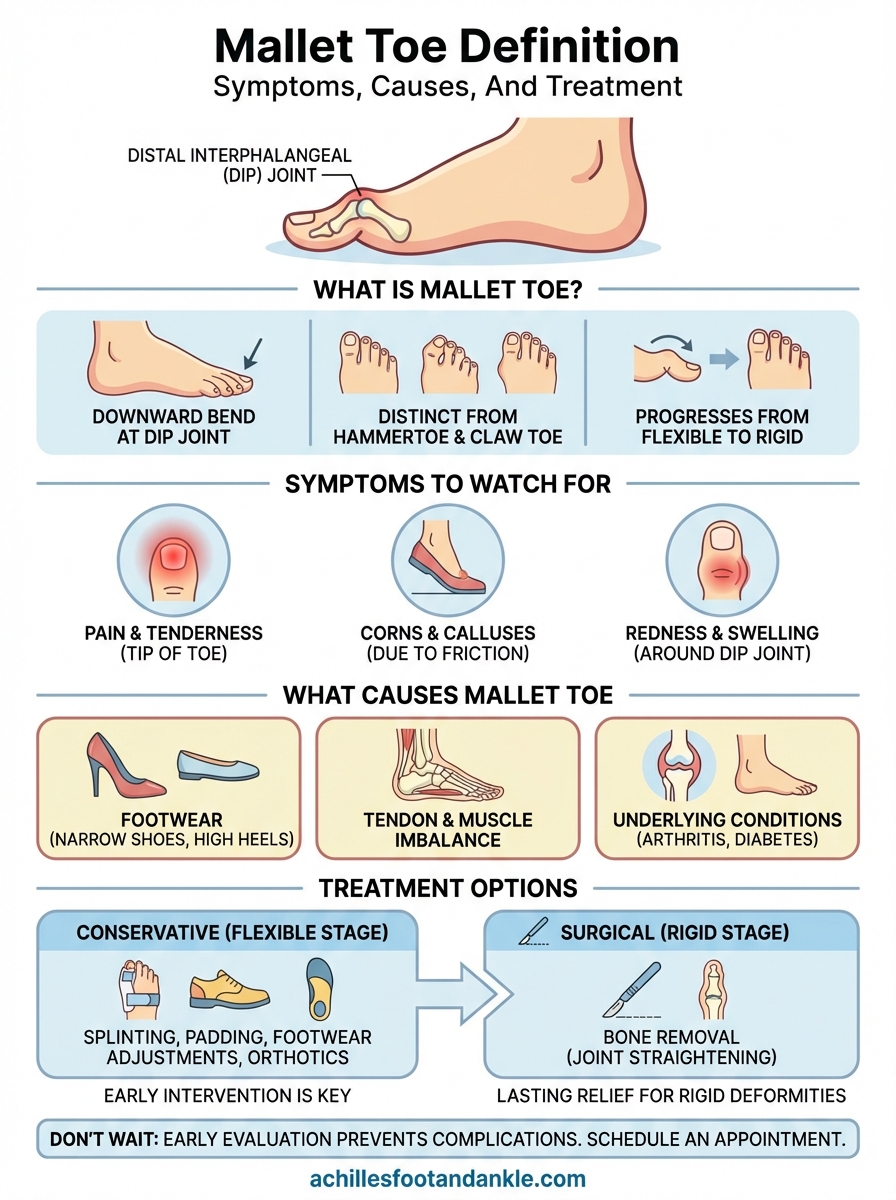
Treatment options for mallet toe
The full mallet toe definition includes knowing that treatment depends entirely on where the deformity stands in its progression. Your podiatrist will match the approach to whether the joint is flexible or rigid, since that single factor determines which options remain available.
Conservative treatments
When your mallet toe is still flexible, non-surgical options are both practical and effective. Padded splints and toe sleeves reduce friction and hold the DIP joint in a straighter position during daily activity. Custom orthotics redistribute pressure across the foot and relieve load from the affected toe. Your podiatrist may also recommend specific stretching exercises to maintain flexibility in the joint and delay further stiffening. Switching to shoes with a deeper toe box removes the repetitive pressure that drives the deformity forward.
Catching a mallet toe in the flexible stage gives you the widest range of treatment choices and the best chance of avoiding surgery.
Surgical correction
Surgery becomes the most reliable path to lasting relief once the deformity stiffens into a rigid position. The most common procedure removes a small section of bone at the DIP joint to allow the toe to straighten. Recovery typically involves protected weight-bearing and a gradual return to normal footwear, with most patients resuming full activity within a few weeks.
When to see a podiatrist
The clearest signal that you need a professional evaluation is persistent pain at the tip of your toe that does not improve after a day of rest. If you notice a visible downward curl forming at the DIP joint, that’s the mallet toe definition in action, and early evaluation gives you the most treatment options before the joint stiffens.
Don’t wait for an open wound or a corn that won’t heal before making an appointment. Diabetic patients especially should treat any toe deformity as urgent, since reduced circulation and nerve damage make complications develop faster than most people expect. Your podiatrist can assess whether the joint is still flexible and match a treatment plan to where you stand right now, before the window for conservative care closes.
Schedule a same-day appointment at Achilles Foot and Ankle Center and get your toe evaluated before the deformity progresses further.






