Charcot foot can quietly destroy the bones and joints in your foot, often without the warning signal of pain. Left untreated, it leads to severe deformity and potential amputation. The good news: with proper intervention, you can protect your foot and maintain your mobility.
A total contact cast for Charcot foot remains one of the most effective treatments available. This specialized cast distributes pressure evenly across your entire foot, allowing damaged bones to heal while preventing further collapse. At Achilles Foot and Ankle Center, our podiatrists have extensive experience fitting and managing total contact casts for patients throughout Central Virginia facing this challenging condition.
This article covers everything you need to know, how total contact casting works, expected healing timelines, daily care requirements, and what recovery actually looks like. Whether you’ve just received a Charcot diagnosis or you’re exploring treatment options, this guide will help you understand the path forward.
Why total contact casting matters in Charcot foot
Your foot contains 26 bones that work together as a complex support structure. When Charcot foot strikes, this structure begins to crumble from within. The condition typically affects people with diabetic neuropathy, where nerve damage masks the pain signals that would normally stop you from walking on a damaged foot.
Walking on weakened bones accelerates the destruction. Each step applies force to an already compromised structure, causing progressive collapse that reshapes your foot into abnormal positions. This deformity creates pressure points that lead to ulcers, infections, and in severe cases, the need for amputation.
The critical window for intervention
You face a narrow timeframe to prevent permanent damage once Charcot foot becomes active. The acute phase lasts several months, during which your bones remain soft and vulnerable to further destruction. Continue walking normally during this period and you risk irreversible deformity.
A total contact cast for Charcot foot addresses this urgent need by completely removing weight-bearing stress from vulnerable areas. Standard boots, shoes, or removable walkers fail because patients naturally put weight on their feet throughout the day. The non-removable nature of the TCC eliminates this risk, giving bones the consistent protection they need to heal properly.
Without proper offloading through immobilization, most Charcot feet progress to severe deformity requiring complex reconstructive surgery or amputation.
What happens without proper casting
Studies show that patients who delay casting or use removable devices face significantly worse outcomes. Your foot continues to collapse, creating rocker-bottom deformity, midfoot prominence, or ankle instability. These changes aren’t just cosmetic concerns; they fundamentally alter how you walk and where pressure concentrates.
Pressure points from deformity lead to chronic wounds that resist healing. These ulcers provide an entry point for bacteria, turning a bone problem into a life-threatening infection. The pathway from untreated Charcot foot to amputation remains disturbingly common among patients who don’t receive aggressive early treatment.
The total contact cast prevents this cascade of complications. By distributing pressure evenly across your entire foot surface, the cast eliminates the concentrated forces that cause ulcers. The rigid immobilization stops movement between damaged bone fragments, allowing natural healing processes to stabilize your foot architecture.
Medical research consistently demonstrates that early casting reduces amputation risk and preserves foot function. Patients who receive prompt TCC treatment maintain their ability to walk independently and avoid the surgical reconstruction that late-stage Charcot foot often requires. The temporary inconvenience of several months in a cast prevents a lifetime of disability and chronic medical problems.
How a total contact cast supports healing
The total contact cast for Charcot foot works through two fundamental mechanisms: complete pressure redistribution and rigid immobilization. Unlike standard casts that focus on a single injury site, the TCC molds to every contour of your foot, creating contact with your entire plantar surface. This design spreads your body weight across the maximum possible area instead of concentrating force on vulnerable spots.
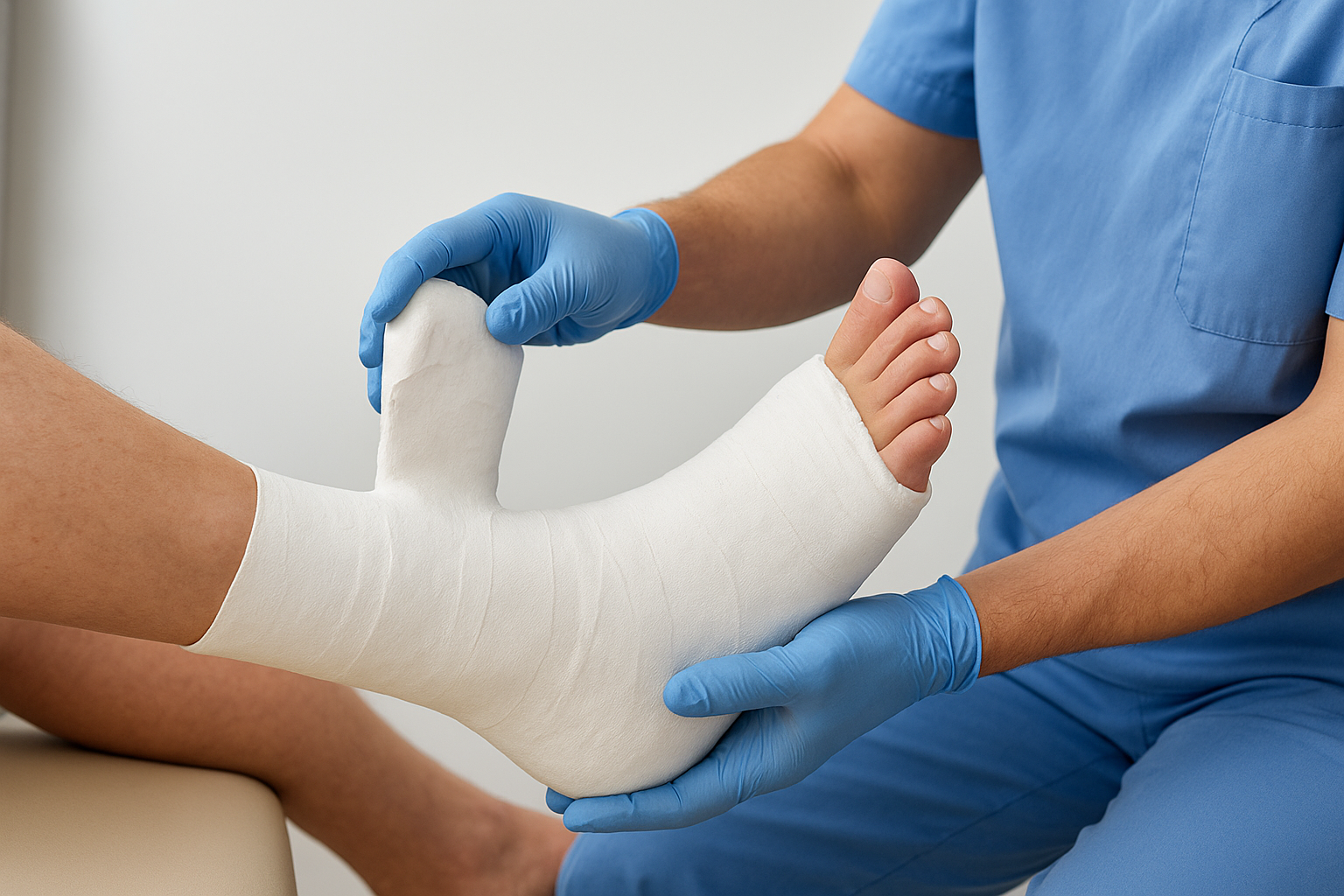
Pressure redistribution across your entire foot
Your podiatrist creates a custom-molded shell that maintains intimate contact with your skin from toes to below the knee. This total surface contact transforms how force travels through your foot. Instead of 300 pounds of pressure hitting a small deformed area, that same force distributes across hundreds of square inches.
The cast achieves this through careful padding and molding techniques. Your doctor applies thin foam over bony prominences, then wraps plaster or fiberglass while maintaining compression. As the material hardens, it conforms precisely to your foot’s current shape, eliminating air gaps that would allow movement or concentrated pressure points.
The average total contact cast reduces peak plantar pressure by 84% compared to walking in regular footwear, giving damaged bones the protection they need to consolidate.
Complete immobilization benefits
Movement between bone fragments prevents healing and perpetuates destruction. The TCC’s rigid structure eliminates this micromotion entirely. Your ankle and foot remain locked in a neutral position, preventing the twisting and flexing that would disturb fragile repair processes happening inside your foot.
Because you cannot remove the cast, your foot receives 24-hour protection without interruption. This consistency proves critical during the acute Charcot phase when bones remain soft and pliable. Even brief periods of unprotected weight-bearing can reverse weeks of healing progress, making the non-removable aspect essential rather than merely convenient.
The cast stays in place continuously, only coming off during scheduled appointments where your doctor examines healing progress and applies a fresh cast if needed.
Who benefits from a TCC and who should avoid it
The total contact cast for Charcot foot works best for patients with active Charcot neuroarthropathy during the acute inflammatory phase. Your doctor confirms this diagnosis through physical examination showing warmth, swelling, and redness combined with imaging evidence of bone destruction or fragmentation. Patients with diabetes-related neuropathy make up the majority of candidates, though anyone with nerve damage affecting their feet can develop this condition.
Ideal candidates for total contact casting
You qualify for TCC treatment if you have adequate blood flow to your foot, intact skin without open wounds, and the ability to use crutches or a wheelchair during the initial weeks. Patients who maintain good glucose control and follow medical instructions closely see the best outcomes because healing requires consistent compliance over several months.
The cast protects you if your foot remains structurally intact enough to benefit from conservative treatment. Early-stage Charcot responds particularly well, where bone softening and inflammation exist but severe deformity hasn’t yet developed. Your podiatrist also considers your overall health status, ensuring you can tolerate the cast and attend regular follow-up appointments.
Patients who receive a total contact cast within the first three months of Charcot onset achieve significantly better functional outcomes compared to those who delay treatment.
Situations requiring alternative treatments
You cannot receive a TCC if you have active foot ulcers or infections that need daily wound care and monitoring. The sealed nature of the cast prevents access to wounds, potentially allowing bacterial growth in an enclosed environment. Patients with severe peripheral arterial disease also face exclusion because inadequate circulation prevents proper healing regardless of offloading.
Certain medical conditions make casting impractical or dangerous. Significant leg swelling from heart failure or kidney disease causes the cast to become loose as fluid levels fluctuate throughout the day. Your doctor chooses different approaches if you have severe osteoporosis, previous amputation affecting balance, or cognitive issues that prevent safe walking with a cast. Skin conditions like severe dermatitis or fragile skin prone to breakdown also require alternative immobilization methods.
Healing time for Charcot foot in a TCC
Healing Charcot foot takes significantly longer than treating a standard fracture. You need three to six months of continuous casting before your bones stabilize enough to consider transitioning to other devices. Some patients require even longer periods depending on the severity of bone destruction and how quickly inflammation resolves in their specific case.
Your podiatrist determines healing progress through temperature monitoring and imaging studies rather than calendar dates. The affected foot starts several degrees warmer than your unaffected side during active Charcot. As healing occurs, this temperature difference gradually decreases. Your doctor measures skin temperature at each appointment, tracking this reduction as a key indicator of bone consolidation.
Typical timeline from cast to recovery
Most patients spend 12 to 16 weeks in their first series of total contact casts, with cast changes every one to three weeks. Your doctor removes and replaces the cast regularly to check skin integrity, assess swelling changes, and monitor healing progress through physical examination and radiographs.
After initial casting ends, you transition to a removable boot or custom walking brace for an additional three to six months. This gradual progression allows your bones to strengthen while reducing your risk of re-injury. The total treatment timeline from diagnosis to returning to regular protective footwear typically spans eight to twelve months.
Rushing the transition from casting to normal footwear increases your risk of recurrent collapse by over 60%, potentially requiring you to restart the entire immobilization process.
Factors that extend or shorten healing
Your blood sugar control directly impacts healing speed. Patients who maintain consistent glucose levels within target ranges heal faster because elevated blood sugar impairs bone remodeling and delays inflammation resolution. Smoking also extends healing time significantly by restricting blood flow to your foot.
Compliance with weight-bearing restrictions affects outcomes dramatically. Patients who follow instructions precisely and avoid premature weight-bearing see faster consolidation. Your age, nutritional status, and presence of other medical conditions like kidney disease or immune disorders also influence how quickly your bones stabilize in the total contact cast for Charcot foot.
What to expect with cast care and follow-ups
Living with a total contact cast requires daily vigilance and regular medical monitoring. Your cast stays on continuously between appointments, meaning you cannot remove it for bathing or any other reason. This 24-hour immobilization protects your foot but demands attention to potential problems that could develop underneath the rigid exterior.
Daily care requirements
You must keep your cast completely dry at all times. Water weakens the cast material and creates moisture against your skin, leading to maceration and infection. Cover your entire cast with waterproof protection during showers, using a specialized cast cover or multiple layers of plastic bags sealed tightly above the cast’s upper edge.
Watch for warning signs that require immediate medical attention. Contact your podiatrist if you notice increasing pain (unusual since neuropathy typically prevents sensation), foul odors coming from inside the cast, visible drainage staining through the cast material, or fever. These symptoms suggest skin breakdown or infection developing where you cannot see it. Your cast should feel snug but never tight enough to cause numbness, tingling, or color changes in your toes.
Never ignore unusual sensations or smells from your cast, even if they seem minor, because problems hidden underneath can progress rapidly without proper intervention.
Follow-up appointment schedule
Your doctor schedules cast changes every one to three weeks depending on how much swelling decreases and your individual healing response. During these appointments, your podiatrist carefully removes the old cast, examines every inch of your skin for pressure areas or breakdown, measures foot temperature, and takes new radiographs to assess bone healing progress.
Expect thorough skin inspections at each visit. Your doctor checks between your toes, around bony prominences, and along the cast edges where friction or pressure might have occurred. If your skin looks healthy and swelling has decreased since the previous cast, your podiatrist applies a fresh total contact cast for Charcot foot with adjusted padding to accommodate your changing foot volume.
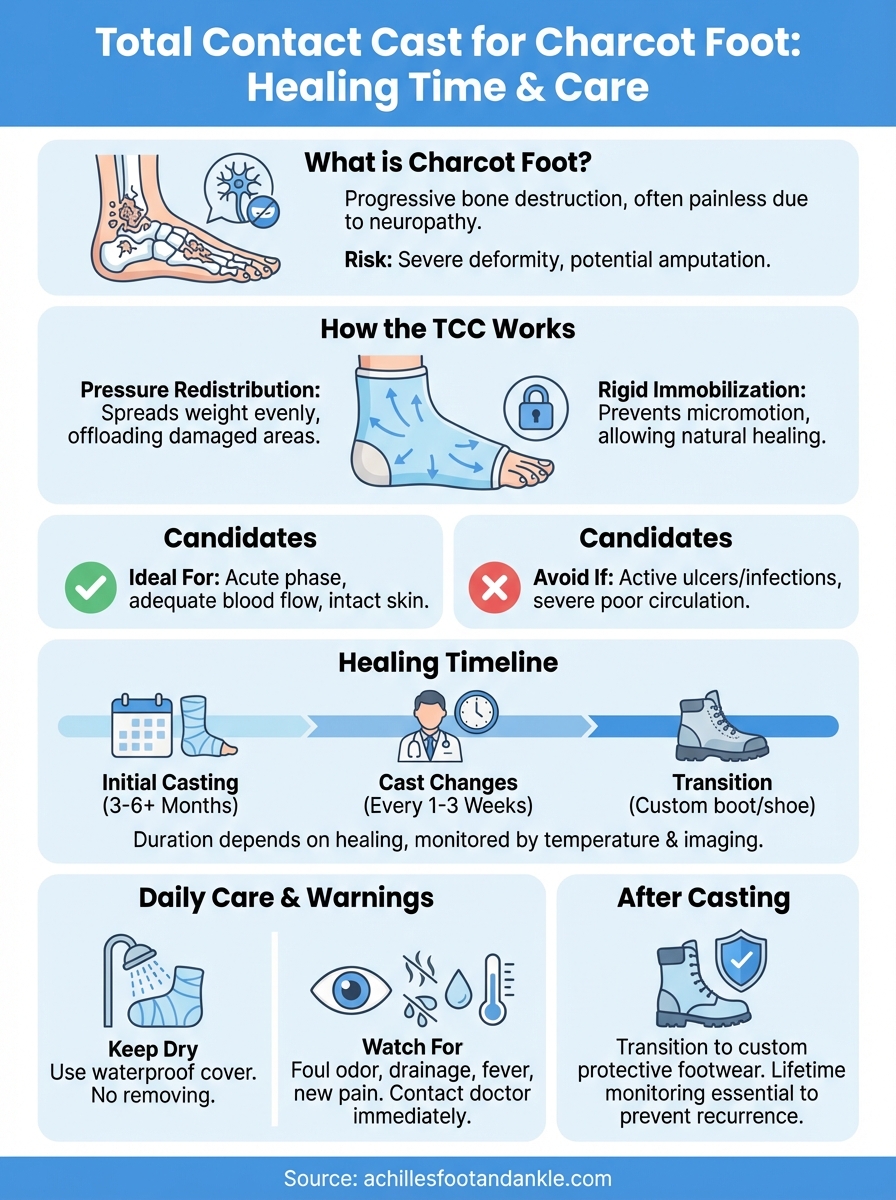
Next steps after you finish casting
After completing your total contact cast for Charcot foot treatment, your journey continues with protective footwear and ongoing monitoring. Your podiatrist transitions you to custom molded shoes or specialized boots that provide continued pressure redistribution while allowing increased mobility. These devices protect your foot from future breakdown while you gradually rebuild strength and confidence in walking.
Regular follow-up appointments remain essential even after casting ends. Your doctor monitors for signs of recurrent inflammation, checks your skin integrity, and adjusts your footwear as needed. Most patients require protective footwear permanently to prevent future Charcot episodes and maintain the stability gained through months of immobilization.
Early intervention makes all the difference in preserving your mobility and preventing complications. If you notice unusual warmth, swelling, or changes in your foot shape, schedule an appointment with our Central Virginia podiatry team right away. Quick action protects your foot and your independence.






