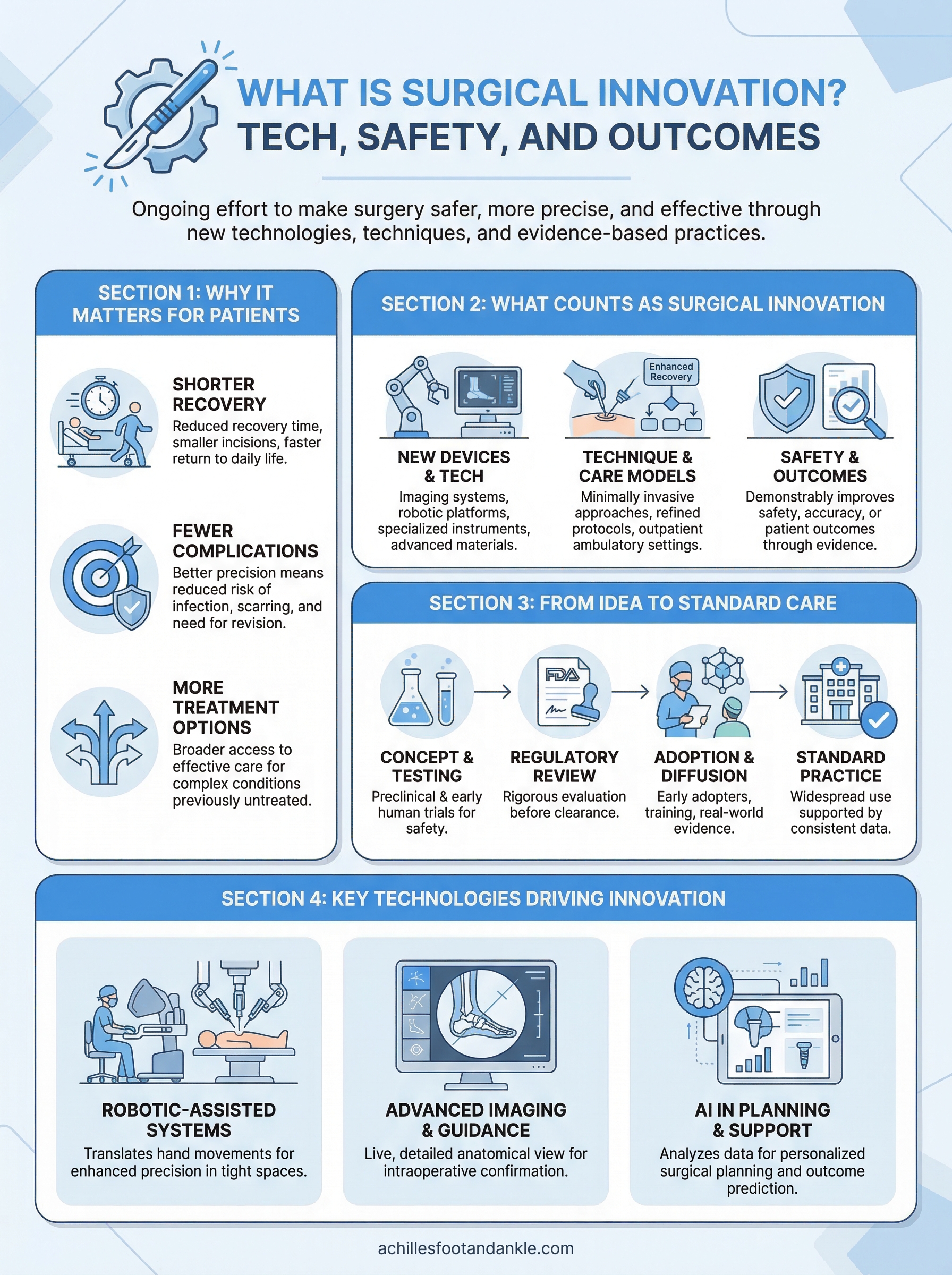
If you’ve ever wondered what is surgical innovation, the short answer is this: it’s the ongoing effort to make surgery safer, more precise, and more effective through new technologies, techniques, and evidence-based practices. But the full picture is far more nuanced, and it matters to anyone facing a surgical procedure, whether it’s a complex reconstruction or a minimally invasive correction.
At Achilles Foot and Ankle Center, surgical innovation isn’t an abstract concept. It’s something our team applies daily across our thirteen Central Virginia locations and our Foot and Ankle Ambulatory Surgery Center, the only one of its kind in the region. From fluoroscopy-guided injections and advanced digital imaging to minimally invasive surgical techniques and reconstructive procedures, we invest in the tools and training that translate innovation into real patient outcomes.
Still, innovation without guardrails creates risk. New technology has to earn its place in the operating room through rigorous testing, ethical oversight, and measurable improvements in patient safety. That tension, between pushing boundaries and protecting patients, sits at the heart of every meaningful advance in surgery. It’s a responsibility we take seriously, and one that shapes how we evaluate and adopt new approaches in our own practice.
This article breaks down what surgical innovation actually involves: the technologies driving it, the safety standards that govern it, and the outcomes that justify it. Whether you’re a patient exploring treatment options or simply curious about where surgery is headed, you’ll leave with a clear, grounded understanding of the field, and how it connects to the care you receive at the foot and ankle level.
Why surgical innovation matters for patients
When you understand what is surgical innovation, the next logical question is: why should it matter to you as a patient? The answer is direct. Surgical outcomes, meaning how well you heal, how quickly you recover, and how much risk you carry into an operating room, depend heavily on whether the surgeon treating you uses current, evidence-backed techniques or outdated ones. Innovation is not about novelty for its own sake. It’s about giving you better odds.
Shorter recovery, less disruption to daily life
One of the most concrete benefits of modern surgical innovation is reduced recovery time. Minimally invasive procedures typically require smaller incisions than traditional open surgery, which means less tissue damage, less postoperative pain, and a faster return to normal activity. For someone managing a job, a family, or a physically demanding lifestyle, those differences are not minor. They’re the difference between weeks on the couch and days.
Advanced instruments also contribute here. Higher-precision tools allow surgeons to complete procedures that once required large exposures through targeted access. When your surgeon can do more with less disruption to surrounding tissue, your body has considerably less healing work to do afterward.
Smaller incisions and targeted approaches are not just cosmetic advantages – they directly reduce infection risk, scarring, and total recovery time.
Better precision means fewer complications
Surgical complications carry real costs: additional procedures, longer hospital stays, delayed healing, and in some cases, permanent harm. Advanced imaging, robotic assistance, and real-time guidance systems have each contributed to reducing those risks. When a surgeon can see exactly where instruments are relative to critical structures, the margin for error shrinks.
This matters most in anatomically complex regions. Foot and ankle surgery involves a dense arrangement of tendons, nerves, blood vessels, and small bones packed into a compact space. Even slight deviations from the intended surgical path can affect function or sensation long after the procedure. Technologies that improve intraoperative visibility and accuracy directly protect you from outcomes that would require further intervention.
More treatment options for complex conditions
Before many modern innovations existed, patients with certain conditions faced a limited set of choices: live with the pain, try conservative measures, or undergo a major open procedure with significant recovery demands. Surgical innovation has expanded that set substantially. Today, conditions that once had no good surgical solution can often be addressed through targeted, lower-risk interventions with predictable recovery timelines.
For patients with chronic conditions like diabetic foot complications or advanced joint degeneration, that expansion is meaningful. More people now qualify for surgery who previously were not good candidates due to health or anatomical constraints, and those who do undergo procedures carry a better risk profile heading in. Innovation effectively broadens access to effective care, not just the quality of care for those who already had it.
Your decision-making also improves as a result. When multiple surgical options exist, your surgeon can match the approach to your specific anatomy, health status, and recovery goals rather than defaulting to a single standard technique. Personalized surgical planning, which is itself a product of ongoing innovation, changes what a conversation with your care team can look like and what outcomes you can realistically expect.
What counts as surgical innovation
Understanding what is surgical innovation requires drawing a clear line between what genuinely qualifies and what does not. Not every new device or modified technique meets the bar. Surgical innovation refers to a meaningful change in surgical practice, whether through a new tool, a new technique, or a new care model, that demonstrably improves safety, accuracy, or patient outcomes. The change has to offer something that existing methods cannot, either in precision, risk reduction, or scope of treatment.
New devices and technologies
The most visible category of surgical innovation involves hardware and technology, including imaging systems, robotic platforms, and specialized instruments. A new imaging system qualifies if it gives surgeons real-time anatomical information they could not access before, reducing guesswork during the procedure. Robotic-assisted platforms qualify when they translate surgeon movements into more controlled, finer-scale actions than the human hand alone can achieve consistently. The key criterion is functional improvement, not just novelty.
A new device only counts as an innovation if it changes what is surgically possible or measurably reduces the risk of doing something already possible.
Implant design also falls into this category. Advances in materials, such as lower-profile plates or biocompatible synthetic grafts, have opened up options for patients with small anatomy or previous implant failures. When a new material or form factor allows fixation that was previously impossible or too risky, that is a genuine innovation.
Changes in technique and care model
Technique-based innovation does not require a new device at all. A modified surgical approach that reduces tissue disruption, repositions incision placement for better healing, or shortens tourniquet time represents a real advance, even if the instruments used are the same. Surgeons develop and refine these approaches through accumulated case experience, outcomes tracking, and peer collaboration.
Care model changes also count. Enhanced recovery protocols, for example, restructure what happens before, during, and after surgery to reduce complications and speed rehabilitation. Shifting certain procedures from inpatient hospital settings to outpatient ambulatory surgery centers is itself an innovation when it lowers infection exposure and shortens the overall care episode. These process-level changes often deliver patient benefits that rival those from new technology alone.
How surgical innovations move from idea to standard care
Part of understanding what is surgical innovation means knowing how a new technique or device actually earns its place in an operating room. The path from a surgeon’s idea to widespread clinical use is structured and deliberate. It involves staged testing, regulatory oversight, and real-world evidence gathering, each step designed to confirm that an innovation genuinely improves outcomes before it becomes routine.

From concept to clinical testing
Most surgical innovations start in a preclinical phase where researchers evaluate a new device or technique in controlled laboratory settings or animal models. This stage tests basic safety and mechanical function before any patient is involved. Once preclinical data looks promising, the innovation moves into early-phase human trials, typically starting with small groups of carefully selected patients who receive close monitoring throughout the process.
Early-phase trials are not about proving an innovation works at scale; they are about confirming it does not cause unexpected harm before broader exposure.
These trials generate the safety and efficacy data that researchers and regulators need to justify moving forward. Outcomes tracked at this stage include complication rates, healing timelines, and any adverse events that did not appear in preclinical testing.
Regulatory review and approval
In the United States, the FDA reviews new surgical devices and technologies before they reach standard clinical use. The review process varies depending on how different a device is from existing approved options. Novel devices with no predicate face the most rigorous review, including clinical trial data requirements. Devices that are substantially equivalent to something already on the market may qualify for a faster clearance pathway, though they still require documented evidence of comparable safety and performance.
Surgeons and institutions also rely on professional society guidelines to evaluate whether an innovation has enough evidence behind it to justify adoption. Organizations like the American College of Surgeons periodically publish consensus statements that help practitioners determine when a new approach has crossed from experimental to evidence-supported.
Adoption into standard practice
Even after regulatory clearance, an innovation often goes through a diffusion period where early adopters build case volume, publish outcomes data, and train colleagues. This phase matters because real-world results sometimes reveal limitations that controlled trials did not surface. Widespread adoption happens when accumulated clinical evidence consistently supports the innovation’s safety and benefit profile, and when training infrastructure exists to help more surgeons implement it reliably.
Technologies driving surgical innovation today
Understanding what is surgical innovation in practical terms means looking at the specific technologies currently reshaping what surgeons can do in the operating room. These are not theoretical advances waiting in a lab. They are tools being used in procedures right now, and they are changing what outcomes you can reasonably expect from surgery.

Robotic-assisted surgical systems
Robotic platforms are among the most significant technology shifts in modern surgery. These systems do not operate independently. Instead, they translate a surgeon’s hand movements into smaller, more precise actions at the instrument tip, filtering out natural hand tremor and allowing access to tight anatomical spaces that would be difficult to reach otherwise. For procedures requiring fine manipulation near nerves or vessels, that level of control matters considerably.
The practical benefit for you as a patient is reduced tissue disruption and more consistent surgical accuracy across cases. Surgeons using robotic systems can also work in positions that would cause fatigue during long open procedures, which sustains precision throughout the entire operation rather than just at the start.
Robotic assistance does not replace surgical judgment – it extends the precision of that judgment into spaces and scales the human hand alone cannot reliably reach.
Advanced imaging and intraoperative guidance
Modern surgical guidance relies on real-time imaging tools that give your surgeon a live, detailed view of anatomy during the procedure rather than working from preoperative scans alone. Fluoroscopy, intraoperative CT, and ultrasound guidance all fall into this category. Each allows the surgical team to confirm positioning and alignment in the moment, reducing the chance that postoperative imaging reveals a correction that fell short.
In foot and ankle surgery specifically, intraoperative imaging is particularly valuable. The dense packing of small bones, tendons, and nerves in that region means that real-time confirmation is often the difference between a procedure that restores full function and one that requires revision.
Artificial intelligence in surgical planning and support
AI tools are entering surgical practice primarily through preoperative planning and outcome prediction. These systems analyze imaging data and patient history to help surgeons anticipate anatomical challenges before the first incision. Some platforms also assist with implant sizing and positioning calculations, reducing the reliance on intraoperative estimation. The result is a more deliberate, data-informed surgical plan that your care team builds around your specific anatomy rather than a generalized template.
New techniques and care models beyond devices
When people ask what is surgical innovation, they often focus on machines and hardware. But technique refinements and care model changes drive just as much progress as any device does. A surgeon who modifies how they approach a procedure, reduces tourniquet time, or repositions an incision for better tissue healing is innovating, even when the instruments in hand have not changed at all.
Technique-level advances that reduce tissue disruption
Minimally invasive surgical techniques have evolved significantly over the past two decades, and their development did not always require new tools. Surgeons have refined approaches that accomplish the same correction through smaller, more strategically placed incisions, reducing the volume of tissue disturbed and shortening the inflammatory response your body generates after the procedure. Less inflammation means less swelling, less pain, and a faster return to weight-bearing and activity.
These refinements emerge from accumulated case volume and systematic outcomes tracking. When surgeons document results consistently, patterns point toward modifications worth testing. That iterative process, grounded in real patient data rather than assumptions, is how technique-level innovation develops independently of device advancement.
Enhanced recovery protocols
Enhanced recovery after surgery (ERAS) protocols restructure the entire care episode, not just what happens in the operating room. These evidence-based pathways standardize decisions about preoperative preparation, anesthetic choices, fluid management, and postoperative pain control to reduce complications and speed rehabilitation. Your recovery starts before the procedure does, with specific instructions that prime your body to heal more efficiently.
Structured recovery pathways consistently reduce hospital length of stay and complication rates compared to uncoordinated, case-by-case approaches.
Pain management within these protocols has shifted significantly toward multimodal strategies that reduce reliance on opioids. Regional nerve blocks, anti-inflammatory agents, and non-opioid analgesics used in combination give you effective pain control while avoiding the side effects and risks that come with heavier narcotic use after surgery.
Ambulatory surgery models
Moving procedures from inpatient hospital settings to dedicated outpatient ambulatory surgery centers is itself a care model innovation with documented patient benefits. You spend less time in a high-acuity hospital environment, which reduces your exposure to hospital-acquired infections and lowers the total cost of your care episode. Focused surgical facilities also allow teams to develop deeper procedural expertise through higher volumes of the same procedure types, which translates directly into better consistency and outcomes for you.
Safety, ethics, and informed consent
Any honest account of what is surgical innovation has to address where it can go wrong. New techniques and devices carry genuine promise, but they also introduce risks that established methods do not. The ethical obligation in surgical innovation is to move fast enough to benefit patients who need better options now, while moving carefully enough to protect patients from harm caused by insufficient evidence. Balancing those two pressures requires a structured ethical framework, not case-by-case judgment calls.
The ethical framework around adopting new procedures
Surgeons and institutions face a real tension when a new procedure shows early promise but lacks long-term outcome data. Professional ethics require that innovations be adopted through an accountable process, not simply because a surgeon finds a new approach interesting or because a device company promotes it aggressively. Most institutions use formal review processes, including surgical review boards and ethics committees, to evaluate whether a new technique has sufficient evidence to justify use outside a research context.
Adopting an innovation without structured oversight shifts the risk of unproven methods entirely onto the patient, often without their full awareness.
Patient safety reporting also plays a role here. Surgeons who track and disclose complications from new approaches contribute to the collective evidence base, which helps the broader medical community understand where a technique works and where it fails. That transparency is part of what keeps innovation honest.
Your role in informed consent
Informed consent is not a formality; it is the mechanism through which you exercise real control over what happens to your body. When a surgeon proposes a procedure that involves a newer technique or implant, you have the right to know whether the approach is established standard care or involves elements with a shorter track record. Asking directly is both appropriate and expected.
Specific questions worth raising include how many times your surgeon has performed this particular approach, what the published complication rates show, and whether alternative methods exist with longer outcome histories. Your surgeon should be able to answer these questions clearly and without deflecting. If the answers are vague or the conversation feels rushed, that itself is information worth acting on before you agree to a procedure.
Understanding the distinction between well-validated techniques and newer approaches gives you the foundation to make decisions that align with your actual risk tolerance and recovery goals.
How outcomes get measured and monitored
Knowing what is surgical innovation only gets you so far if no one is systematically tracking whether that innovation actually delivers. Outcome measurement is what transforms surgical advancement from theory into verified practice. Without it, surgeons, institutions, and patients have no reliable way to distinguish genuine progress from well-marketed experimentation. Rigorous monitoring is the mechanism that keeps surgical innovation accountable to real results.

Patient-reported outcome measures
Patient-reported outcome measures (PROMs) capture what matters most to you: your pain levels, your functional recovery, and your ability to return to normal activity. These standardized surveys collect your subjective experience at defined time points before and after surgery, creating a structured record that reflects outcomes from the patient’s perspective rather than just clinical test results. When aggregated across many cases, PROMs reveal patterns that objective measures like imaging or range-of-motion tests can miss entirely.
PROMs consistently uncover recovery gaps that clinical assessments alone overlook, which is why leading surgical programs treat them as a core data point, not an optional add-on.
For foot and ankle procedures specifically, validated scoring tools like the Foot and Ankle Ability Measure (FAAM) and the American Orthopaedic Foot and Ankle Society (AOFAS) scales give care teams a consistent framework for comparing your outcomes against published benchmarks. That comparison tells your surgeon whether your recovery is tracking appropriately and flags early if intervention or adjustment is warranted.
Registry data and long-term surveillance
Surgical registries collect outcome data across large patient populations over extended follow-up periods, giving researchers and clinicians a far broader view than any single surgeon’s case volume can provide. These registries track complication rates, revision frequencies, implant survival, and functional outcomes over years, revealing how a new technique or device performs once it moves beyond carefully controlled trial conditions into general clinical use.
Your care team uses this population-level data to contextualize your individual results and to make informed decisions about whether a procedure’s track record justifies continued use. Registries also generate the evidence base that professional societies draw on when updating clinical guidelines. When enough registry data shows a technique underperforming or carrying unexpected risks, standard of care shifts accordingly, which protects future patients from harm that early adopters may have experienced before the pattern became clear.
What surgical innovation looks like in foot and ankle care
Understanding what is surgical innovation becomes most relevant when you connect it to the specific procedures and conditions you might actually face. Foot and ankle surgery presents unique challenges that make innovation particularly important here. The region contains 26 bones, 33 joints, and more than 100 tendons, muscles, and ligaments in a compact space that bears your full body weight with every step. Precision matters more in this environment than almost anywhere else in orthopedic surgery.
Minimally invasive approaches to structural corrections
Minimally invasive techniques have transformed how surgeons address common structural conditions like bunions, hammertoes, and flatfoot deformity. Where traditional open procedures required large incisions and extensive soft tissue dissection, current approaches use percutaneous or small-portal entry points that accomplish the same bone corrections with far less disruption to surrounding structures. Your recovery reflects that difference in a direct and measurable way.
For foot and ankle conditions specifically, minimally invasive corrections typically allow earlier weight-bearing and a faster return to footwear than equivalent open procedures.
Surgeons at dedicated ambulatory surgery centers perform these procedures in focused outpatient settings that reduce your exposure to hospital-associated risks while allowing the care team to develop deep, procedure-specific expertise through consistent case volume. That concentration of experience produces more reliable outcomes than low-volume general surgical environments can.
Advanced fixation and implant options
Implant technology for foot and ankle reconstruction has advanced considerably in the past decade. Low-profile titanium hardware, absorbable fixation devices, and synthetic bone graft substitutes give your surgeon more options to match fixation strategy to your specific bone quality, anatomy, and activity level. Patients who were previously poor candidates for certain procedures due to small bone size or prior implant complications now have viable surgical pathways available to them.
Intraoperative guidance tools, including fluoroscopy and real-time ultrasound, give surgeons immediate confirmation of hardware placement and alignment during the procedure rather than relying solely on postoperative imaging to evaluate results. When your surgical team can verify positioning before closing, the likelihood of requiring a revision procedure drops significantly. These combined advances reflect how ongoing innovation directly shapes the quality of care you receive at the foot and ankle level.
Key takeaways and next steps
Understanding what is surgical innovation gives you a sharper lens for evaluating the care you receive. Innovation encompasses new technologies, refined techniques, and restructured care models, each held accountable by rigorous safety standards, ethical oversight, and systematic outcome measurement. Progress in this field directly shapes your recovery time, your complication risk, and the range of treatment options available to you.
At the foot and ankle level, those advances translate into minimally invasive corrections, precise intraoperative guidance, and implant options matched to your specific anatomy. The result is care that is more targeted and more predictable than it was even a decade ago.
If you are dealing with a foot or ankle condition and want to explore what current surgical techniques can offer you, the next step is a conversation with a specialist. Book an appointment today and find out which evidence-backed options fit your situation by scheduling through our same-day appointments page.






