Every cut, surgical incision, or diabetic ulcer on your foot triggers the same biological sequence, a repair process your body runs automatically, whether the wound is minor or limb-threatening. Understanding the wound healing stages and timeline gives you a clear picture of what’s normal, what’s delayed, and when to get professional help.
At Achilles Foot and Ankle Center, our team treats foot and ankle wounds daily, from post-surgical recovery to complex diabetic ulcers that resist healing. Our Advanced Wound Care and Limb Salvage program exists specifically because wounds below the knee face unique challenges: reduced blood flow, pressure from walking, and higher infection risk in patients with diabetes or peripheral neuropathy.
This guide breaks down the four biological phases of wound healing, hemostasis, inflammation, proliferation, and maturation, with specific timelines for each stage. You’ll learn what your body is doing at every point in the process, what can go wrong, and the signs that a wound needs clinical attention rather than more time.
Why wound healing stages matter
Knowing the wound healing stages and timeline isn’t just academic knowledge. It directly changes how you respond to a wound on your foot or ankle. When you understand what your body is supposed to do at each phase, you can recognize when healing is progressing normally, when it’s stalled, and when the situation has moved past home care. That awareness can be the difference between a wound that closes cleanly in two weeks and one that becomes a chronic ulcer.
How the stages guide treatment decisions
Every treatment decision a clinician makes connects to a specific healing phase. Applying a debridement procedure makes sense during inflammation to remove dead tissue but would disrupt fragile new tissue during proliferation. Compression therapy supports the maturation phase but can be counterproductive if applied to a wound still fighting active infection.
Understanding which stage your wound is in lets your care team choose the right intervention at the right time, rather than applying a one-size-fits-all approach.
When you describe your wound accurately to a provider, including how long it has been present and what it currently looks like, you help them place it in the correct phase immediately. That accuracy speeds up the path to the right treatment.
Why foot and ankle wounds carry higher stakes
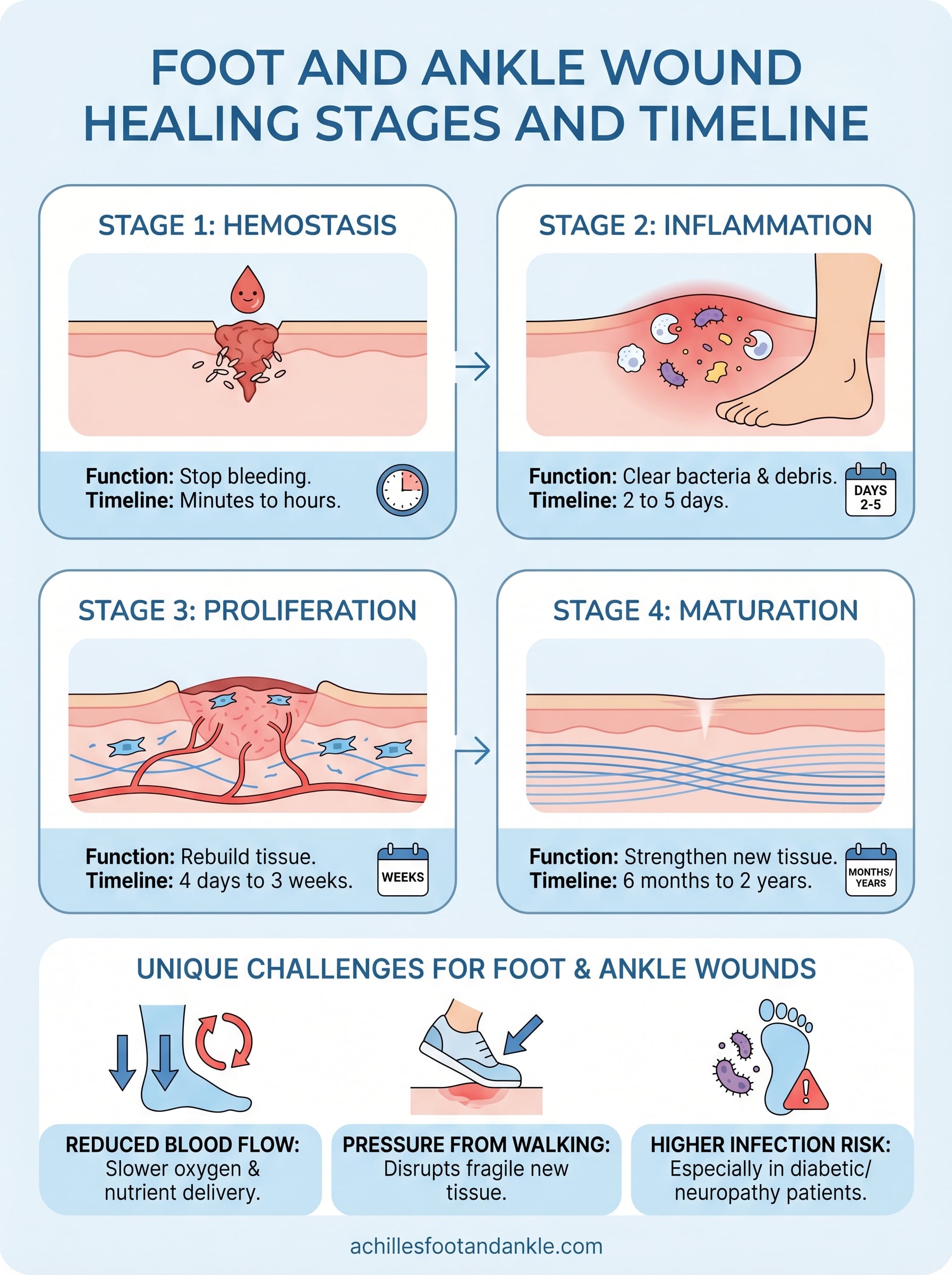
Wounds on the foot and ankle face mechanical and circulatory challenges that wounds on other parts of the body do not. Every step you take puts direct pressure on healing tissue. Blood circulation to the lower extremities is naturally weaker, which slows the delivery of the oxygen and nutrients that each healing phase depends on. Patients with diabetes or peripheral arterial disease face even greater risk because nerve damage can mask pain signals, allowing wounds to worsen before they get noticed.
The foot’s anatomy also means that an untreated wound sits close to tendons, joints, and bone. Infection that spreads in that environment can reach bone faster than in other regions of the body, turning a surface wound into a limb-threatening condition.
What happens when a wound gets stuck
A wound that stops progressing through the normal stages is called a chronic wound. These wounds stall most often in the inflammatory phase, trapped in a cycle of tissue damage and incomplete repair. Chronic wounds are a leading cause of lower limb amputation in the United States, particularly in diabetic patients.
Recognizing a stalled wound early gives clinicians the window to intervene with advanced therapies before the damage becomes irreversible. That window closes faster in the foot and ankle than almost anywhere else on the body.
The four stages of wound healing
Your body follows the same four-stage repair sequence for every wound, from a minor blister to a complex surgical incision. The complete wound healing stages and timeline covers four distinct biological phases, each with a specific job and a predictable time frame.
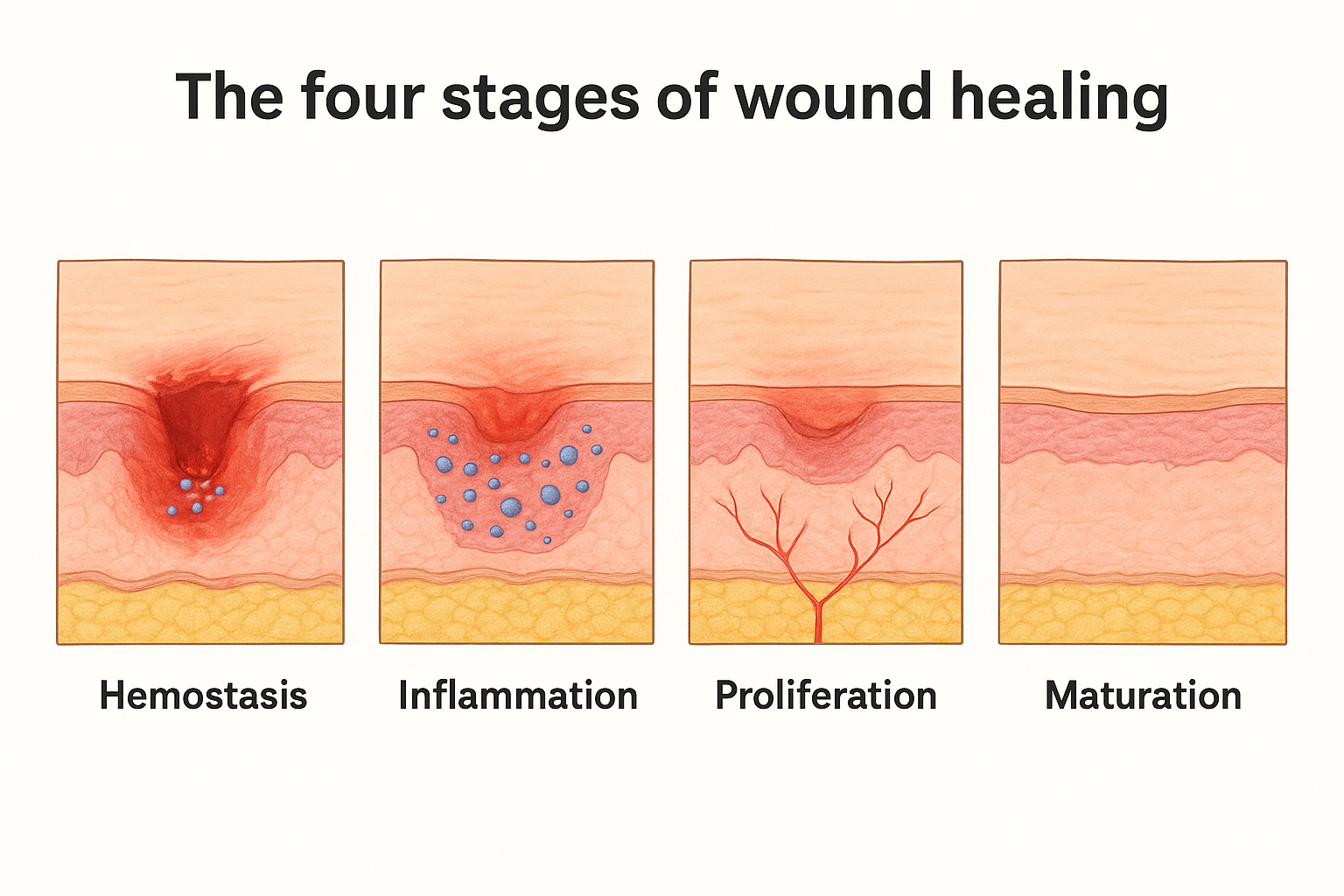
| Stage | Name | Primary Function | Typical Duration |
|---|---|---|---|
| 1 | Hemostasis | Stop bleeding | Minutes to hours |
| 2 | Inflammation | Clear bacteria and debris | 2 to 5 days |
| 3 | Proliferation | Rebuild tissue | 4 days to 3 weeks |
| 4 | Maturation | Strengthen new tissue | 6 months to 2 years |
Hemostasis and inflammation
Hemostasis triggers within seconds of injury. Platelets aggregate, blood vessels constrict, and a fibrin clot seals the wound to stop blood loss. This stage completes in minutes to hours for most wounds, setting the foundation for everything that follows.
Inflammation begins as hemostasis winds down and typically lasts two to five days. White blood cells flood the wound site to destroy bacteria and remove dead tissue. Redness, swelling, and warmth during this phase are normal responses, not signs that something has gone wrong.
Inflammation that persists beyond seven days in a foot wound often signals infection or an underlying condition that requires clinical evaluation.
Proliferation and maturation
Proliferation is when your body builds new tissue. Fibroblasts deposit collagen, new blood vessels grow into the wound bed, and the wound edges contract inward. This phase runs from four days to three weeks, often overlapping with the tail end of inflammation.
Maturation involves collagen remodeling to increase the tensile strength of the new tissue your body just built. The repaired area can look and feel different from surrounding skin for months as this process runs. For deep or large wounds, maturation can take six months to two years to complete.
Wound healing timeline by wound type
The wound healing stages and timeline vary significantly by wound type and depth. A shallow scrape on your heel closes in days, while a diabetic foot ulcer can require months of consistent care. Knowing what’s typical for your wound helps you set realistic expectations and catch delays early.
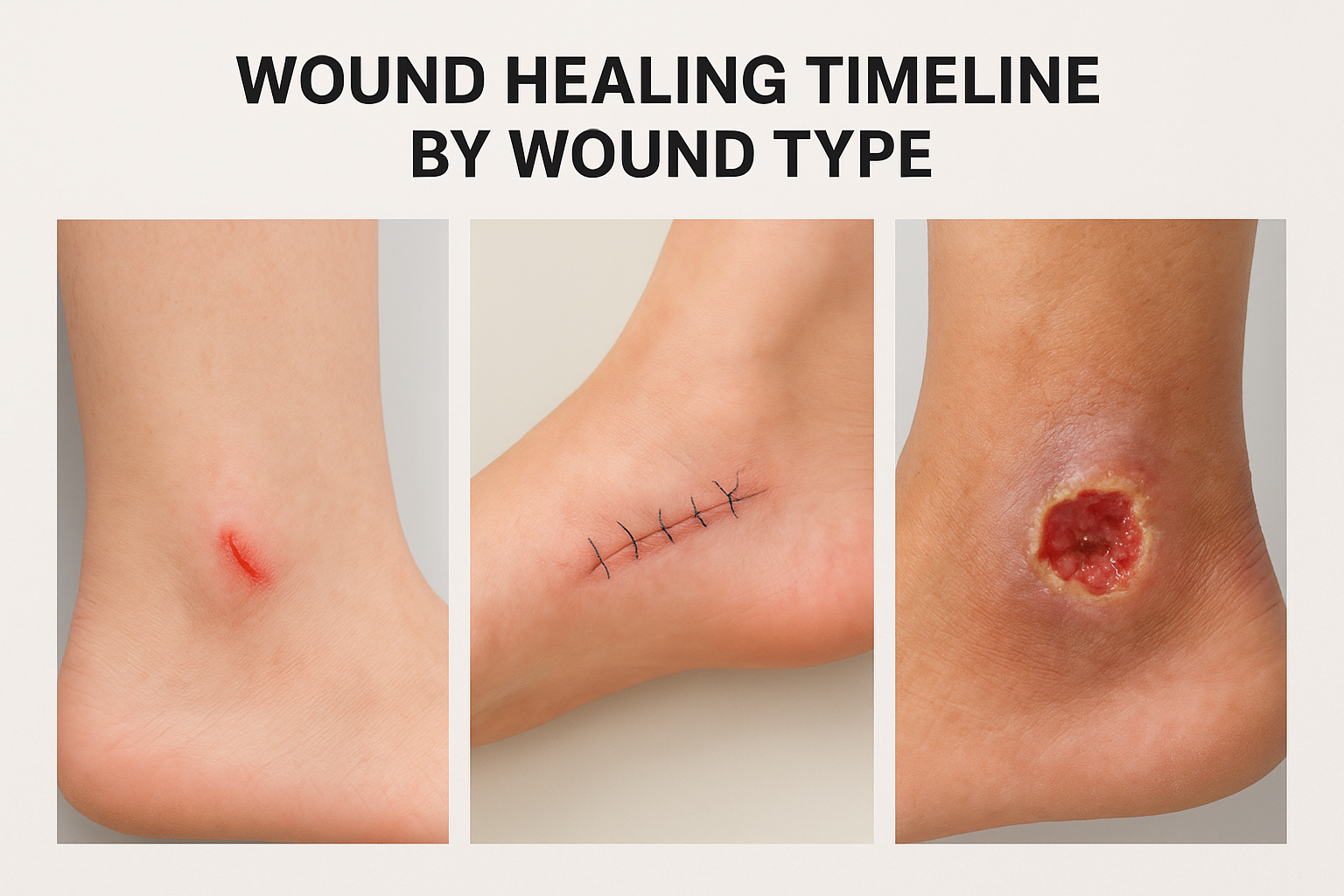
Minor cuts, blisters, and abrasions
Shallow wounds affecting only the outer skin layers typically complete all four healing phases within ten to fourteen days. Your body stops bleeding in minutes, clears the inflammatory phase by day three or four, and finishes active tissue repair by the end of the second week.
Friction blisters and minor burns follow a similar timeline, provided you keep the wound clean and shielded from further pressure. These wounds rarely need clinical attention unless they open, become infected, or appear on high-load areas like your heel or the ball of your foot.
If a minor foot wound has not visibly closed after two weeks, have it evaluated rather than waiting longer.
Surgical incisions
A clean surgical incision from procedures like bunion correction or Achilles tendon repair follows a predictable but layered timeline. Outer skin typically closes within two to three weeks, while internal structures, including tendon and bone, continue remodeling for six to twelve months.
Your activity level, suture technique, and post-operative care all influence how quickly each phase progresses. Sticking to your surgeon’s weight-bearing and wound care instructions directly affects how well the repaired tissue holds up long-term.
Diabetic foot ulcers and chronic wounds
Diabetic ulcers run on a completely different timeline from acute wounds. Depending on depth, circulation, and infection history, these wounds can take twelve weeks or longer to close with consistent clinical care.
Without targeted treatment, many diabetic ulcers stall in the inflammatory phase and never advance. Your risk of bone infection and serious complications rises substantially the longer the wound stays open.
What affects healing time and slows it down
The wound healing stages and timeline your body follows can shift dramatically based on factors both inside and outside your control. Some delays happen at the cellular level, while others come from daily habits or wound care choices. Understanding what slows healing helps you take the right steps and gives your care team better information to work with.
Systemic conditions that interrupt the healing process
Diabetes is the single most significant systemic factor that disrupts wound healing in the foot and ankle. High blood glucose damages small blood vessels and impairs the white blood cell function your body depends on during the inflammatory phase. Peripheral neuropathy, common in diabetic patients, removes the pain signals that would otherwise alert you to pressure or early infection. Peripheral arterial disease compounds the problem by reducing oxygen delivery to tissue that needs it to rebuild.
Poor circulation below the knee is one of the most preventable contributors to wound complications, and managing it actively changes patient outcomes.
Other conditions that extend healing time include autoimmune disorders, chronic kidney disease, malnutrition, and obesity. Medications like corticosteroids and some chemotherapy drugs also suppress the inflammatory response your body needs to clear debris and begin repair.
Wound environment and external factors
Wound contamination and infection are the most direct external causes of delayed healing. Bacteria in the wound bed compete with your body’s repair cells, pulling the wound back into the inflammatory phase repeatedly. Repeated pressure on a healing foot wound, from walking without protective footwear, causes similar disruption by tearing fragile new tissue before it can mature.
Smoking reduces circulation and oxygen levels in tissue, slowing every phase of the repair sequence. Dehydration and poor nutrition deprive your body of the collagen-building materials proliferation depends on.
When to seek foot and ankle wound care
Most foot wounds benefit from professional evaluation earlier than people expect. The wound healing stages and timeline can shift quickly in the lower extremities, and waiting for a wound to "get better on its own" is a risk that carries real consequences when circulation or sensation is already compromised.
Warning signs that require immediate attention
Some symptoms signal that your wound has moved past the point of safe home management. Increasing redness, warmth, or swelling after the first five days indicates the inflammatory phase is not resolving, which often points to infection. Discharge that turns thick, discolored, or develops an odor requires same-day evaluation.
A wound that is larger or deeper than when you first noticed it needs immediate professional care, not a longer wait.
Watch for these specific warning signs:
- Fever or chills alongside a foot wound, which suggest infection has spread beyond the skin
- Wound edges that separate or pull apart rather than closing
- Visible tendon, bone, or fat tissue in the wound bed
- Numbness or loss of sensation near the wound site
- Any wound present for more than two weeks with no visible progress
Wounds that need ongoing clinical management
Some wounds require structured clinical care from the start, not just when complications arise. If you have diabetes, peripheral arterial disease, or a history of chronic wounds, any break in skin on your foot warrants professional assessment within the first 24 to 48 hours. These conditions make it nearly impossible to predict how fast each healing phase will progress without monitoring.
Advanced wound care programs give your care team the tools to track tissue changes, adjust treatment by phase, and intervene before a delay becomes a permanent setback.
Conclusion
The wound healing stages and timeline your body follows are predictable, but foot and ankle wounds add variables that make monitoring non-negotiable. From hemostasis to maturation, each phase depends on the one before it, and any disruption can push a manageable wound toward a serious complication. Conditions like diabetes, poor circulation, and peripheral neuropathy make that risk substantially higher in the lower extremities.
Your best tool is early action. Recognizing warning signs within the first week, getting a wound evaluated before it stalls, and following a structured care plan all improve your outcome more than waiting ever will. A wound that closes cleanly in two weeks does not have to become a wound you manage for two years. Professional wound care gives you that outcome by matching the right treatment to the right phase at the right time. Schedule a same-day appointment with Achilles Foot and Ankle Center and get your wound assessed today.






