Heel pain has a way of catching you off guard. One morning you step out of bed and feel a sharp stab under your foot, and suddenly every step is a reminder that something’s wrong. The good news is that learning how to prevent heel pain before it starts, or before it circles back, is more straightforward than most people think once you understand what actually triggers it.
Most heel pain comes from repetitive stress rather than a single injury. Tight calf muscles, worn-out shoes, and rapid jumps in activity quietly push structures like the plantar fascia and Achilles tendon past their limits. That means small, consistent adjustments to your daily routine can do more to protect your heels than any quick fix.
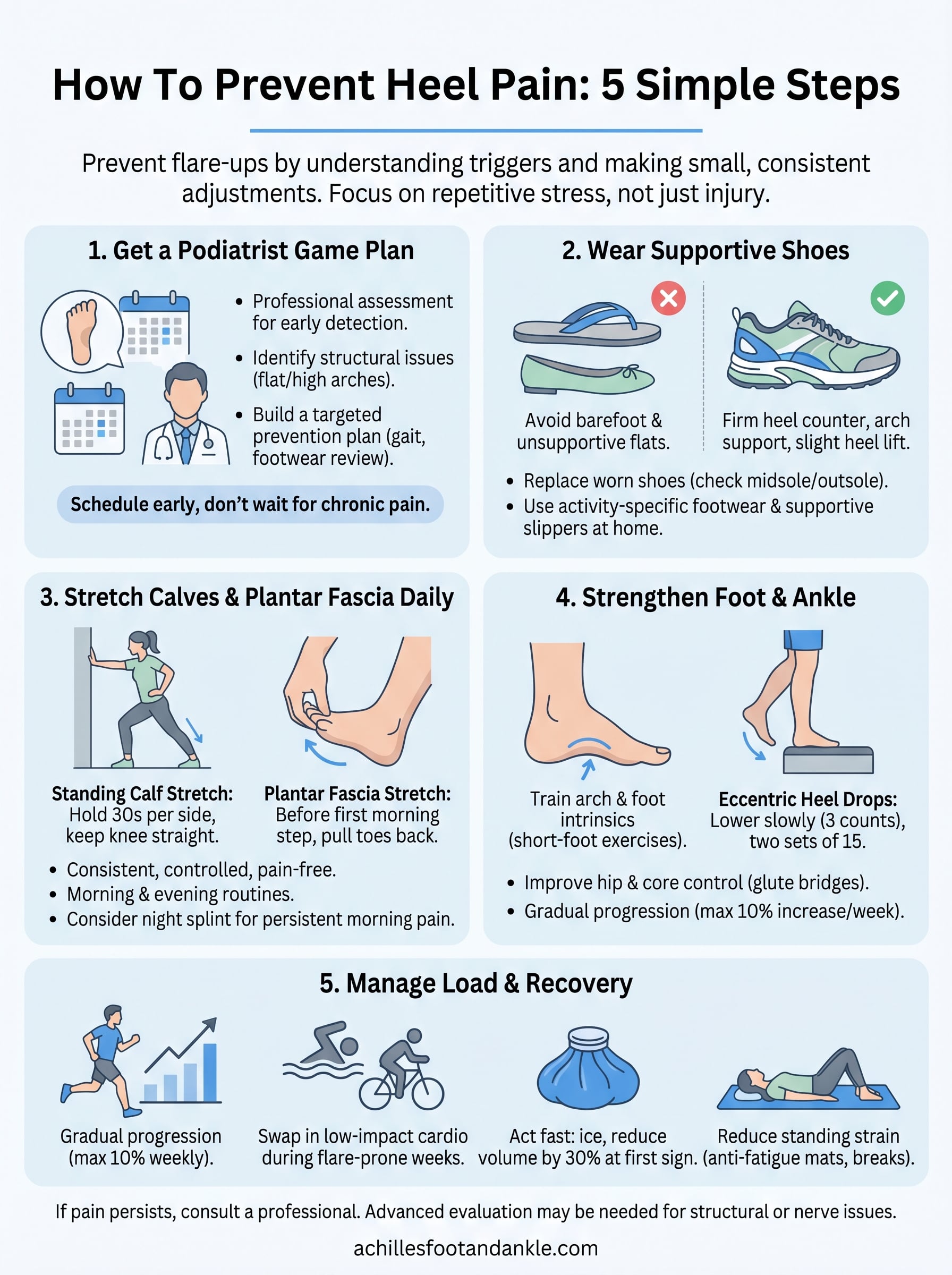
At Achilles Foot and Ankle Center, our podiatrists across Central Virginia treat heel pain every single day, and we’d much rather help you avoid it altogether. Below, we break down five practical steps you can start using right now to keep your heels healthy and free from flare-ups.
1. Get a podiatrist game plan before it becomes chronic
Most people wait until heel pain becomes unbearable before they see a podiatrist. That delay is exactly what turns a manageable overuse issue into a months-long recovery that disrupts your work, workouts, and daily routine. Starting with a professional assessment is the smartest move you can make if you want to understand how to prevent heel pain from becoming a recurring problem.
What to do now
Schedule a podiatry evaluation at the first sign of recurring discomfort, even if the pain feels minor. A podiatrist can identify structural issues like flat arches, high arches, or leg-length discrepancies that you cannot spot on your own, and they can build a targeted prevention plan before damage has a chance to compound.
Your appointment should include a gait assessment, a footwear review, and a baseline check of your current flexibility and strength. These findings give you something concrete to act on instead of guessing at the cause.
Why this prevents recurring heel pain
Plantar fasciitis and Achilles tendinopathy, the two most common drivers of heel pain, both develop gradually over weeks. By the time the pain becomes sharp and consistent, the tissue has usually been under significant stress for a long time. A podiatrist can catch that stress early and redirect it with the right combination of stretching guidance, load management, and footwear corrections.
Getting ahead of heel pain with a professional assessment is the single most effective step in any prevention strategy.
Watch for common patterns that signal the cause
Pay close attention to when and where your pain shows up. Pain that is worst with your first steps in the morning typically points to plantar fasciitis. Pain at the back of the heel that builds during or after activity usually signals Achilles tendon irritation. Pain in both heels simultaneously can sometimes point to a systemic condition like arthritis or a nerve issue.
Tracking these patterns before your appointment gives your podiatrist a clearer picture and speeds up the process of identifying the root cause.
When to book a visit at Achilles Foot and Ankle Center
Book an appointment if heel pain lasts longer than one week, keeps returning after short rest periods, or starts to change the way you walk. At Achilles Foot and Ankle Center, same-day appointments are available across thirteen Central Virginia locations, so you do not have to wait long to get a clear diagnosis and a prevention plan you can actually follow.
2. Wear supportive shoes and stop going barefoot
Your footwear is one of the biggest factors in how to prevent heel pain, and it is also one of the easiest things to fix. Walking barefoot on hard floors, or wearing shoes with no arch support, forces your plantar fascia and heel to absorb impact they are not designed to handle repeatedly.
What to look for in everyday shoes
Choose shoes with a firm heel counter, a slight heel lift, and adequate arch support built into the midsole. Flexible, flat shoes like flip-flops or ballet flats offer almost no protection for the structures under your heel. A good everyday shoe should not bend easily in half when you twist it.

The right shoe does not just feel comfortable at first wear; it actively protects your heel through every hour you are on your feet.
Adjust your footwear for work, workouts, and home
Activity-specific footwear matters more than most people realize. Running shoes should match your gait pattern, work boots should have cushioned insoles, and at home, keep supportive slippers within reach instead of walking barefoot from room to room. Rotating between two pairs of athletic shoes also helps each pair fully decompress between uses.
Replace worn shoes before they trigger a flare-up
Most athletic shoes lose meaningful cushioning and support after 300 to 500 miles of use, even when they still look fine on the outside. Check the midsole for compression and the outsole for uneven wear patterns, which signal that the shoe is no longer protecting your heel properly.
When inserts or orthotics make sense
Over-the-counter insoles can help mild cases, but custom orthotics prescribed by a podiatrist correct the specific biomechanical issues driving your heel pain. If store-bought inserts have not solved the problem after a few weeks, custom orthotics are worth discussing at your next appointment.
3. Stretch your calves and plantar fascia every day
Tight calves and a stiff plantar fascia consistently drive heel pain, and daily stretching is one of the most direct ways to keep both in check. If you want to understand how to prevent heel pain from recurring, building flexibility in these tissues should be a fixed part of your routine.
Do the key stretches the right way
Two stretches anchor any solid heel pain prevention plan:

- Standing calf stretch: Press your back heel flat against the floor with your knee straight and hold for 30 seconds per side.
- Plantar fascia stretch: Pull your toes back toward your shin before your first step each morning until you feel a firm pull along the arch.
Consistent, correct stretching reduces tissue load more effectively than aggressive stretching done only when pain flares.
Build a simple morning and evening routine
Stretch before your first steps of the day and again before bed. These are the two windows when tissue tension peaks: right after waking and right before prolonged rest.
Morning stretching takes under two minutes and protects the fascia before weight-bearing stress hits. Evening stretching keeps the calf pliable overnight so you wake to less stiffness.
Use a night splint when morning pain keeps returning
A night splint holds your foot in mild dorsiflexion while you sleep, stopping the plantar fascia from tightening during rest. Add one when first-step morning pain keeps repeating despite consistent daytime stretching.
Avoid stretch mistakes that can backfire
Bouncing or forcing a stretch through sharp pain can worsen small tears in already irritated tissue. Keep every stretch controlled and pain-free, and back off immediately if discomfort increases during the movement.
4. Strengthen the foot and ankle to support your heel
Stretching keeps tissue flexible, but strength is what keeps your heel protected under real load. Weak intrinsic foot muscles and underpowered calves force your plantar fascia and Achilles tendon to pick up the slack, and that extra stress is a direct path back to pain. Building targeted strength is a core part of how to prevent heel pain from returning after it clears up.
Train your arch and foot intrinsics
Short-foot exercises activate the small muscles that support your arch, reducing the load transferred to your plantar fascia. Practice pulling your toes toward your heel without curling them to contract the arch, and hold for five seconds at a time. Marble pickups and single-leg balance drills also build the fine motor control your foot uses to stabilize with every step.
Strengthen calves and control Achilles load
Eccentric heel drops off a step are one of the most researched and effective exercises for protecting the Achilles tendon. Lower your heel slowly over three counts, then use both feet to return to the starting position. Start with two sets of fifteen reps on each side and build from there.
Eccentric calf training reduces Achilles tendon stress more effectively than concentric-only exercises.
Improve hip and core control to fix mechanics
Weak glutes and unstable hips cause your foot to pronate excessively, shifting load directly onto your heel. Add single-leg glute bridges and lateral band walks to your weekly routine to correct this pattern before it reaches your foot.
Use smart progressions to avoid tendon flare-ups
Increase resistance or repetitions by no more than ten percent per week to give tendons time to adapt. Tendons respond more slowly than muscles, so outpacing their recovery creates the exact overload you are trying to avoid.
5. Manage training load, surfaces, and recovery
How much you do matters just as much as how you do it when it comes to how to prevent heel pain. Your heel structures need time to adapt to increasing demands, and ignoring recovery is one of the fastest ways to undo every other step on this list.
Increase activity gradually and plan rest
Jumping from low activity to long runs or extended walks strains your plantar fascia and Achilles tendon before they have time to adapt. Increase your weekly mileage or training time by no more than ten percent each week, and schedule at least one full rest day between high-impact sessions.
Gradual progression protects your heels far better than alternating between overtraining and complete rest.
Plan your recovery just as deliberately as your training days to give heel tissues the time they need to handle increasing load.
Swap in low-impact cardio during flare-prone weeks
When your training schedule peaks or your heels feel tender, replace running and jumping with swimming, cycling, or elliptical training. These activities protect your heel tissue while keeping your cardiovascular fitness on track.
Adding a low-impact week every four to six weeks also gives your tendons a built-in reset that reduces the risk of overuse injury accumulating quietly in the background.
Reduce all-day standing strain with small changes
If your job keeps you on your feet for hours, anti-fatigue mats and regular seated breaks reduce the cumulative load on your heels. Moving around or shifting your weight every 30 to 45 minutes also prevents pressure and fatigue from building in one spot.
Act fast when pain starts instead of pushing through
At the first sign of new heel discomfort, cut your activity volume by about 30 percent and apply ice for 10 to 15 minutes after activity. Early intervention consistently stops minor irritation from turning into a weeks-long setback that sidelines you completely.
If heel pain keeps coming back
Persistent heel pain that returns after rest, or never fully clears between flare-ups, signals that something deeper is driving the problem. Following these five steps covers the most reliable methods for how to prevent heel pain from becoming a recurring issue, but some cases involve structural, biomechanical, or nerve-related factors that self-management alone cannot resolve.
A podiatrist can run advanced imaging, gait analysis, and pressure testing to identify what your heel is actually dealing with and build a treatment plan around that specific diagnosis. Waiting and hoping the pain settles on its own often adds months to your recovery and increases the risk of long-term tissue damage.
If your heel pain keeps returning despite your best efforts, the right next step is a professional evaluation. Book a same-day appointment at Achilles Foot and Ankle Center and get a clear plan from a specialist who treats heel conditions every day.






