That sharp stab in your heel during your first few morning steps, if you’ve felt it before, you already know how quickly plantar fasciitis can sideline your training. And if you haven’t, understanding how to prevent plantar fasciitis before it starts is one of the smartest moves you can make as a runner. The condition accounts for roughly one million doctor visits per year in the U.S., and runners are among the most frequently affected groups.
At Achilles Foot and Ankle Center, our podiatrists treat plantar fasciitis across our Central Virginia locations every single day, from weekend joggers ramping up mileage to competitive athletes pushing through pain they shouldn’t ignore. What we see consistently is that most cases are preventable with the right habits. The problem is that many runners don’t take action until they’re already limping through a flare-up, and recovery always takes longer than prevention.
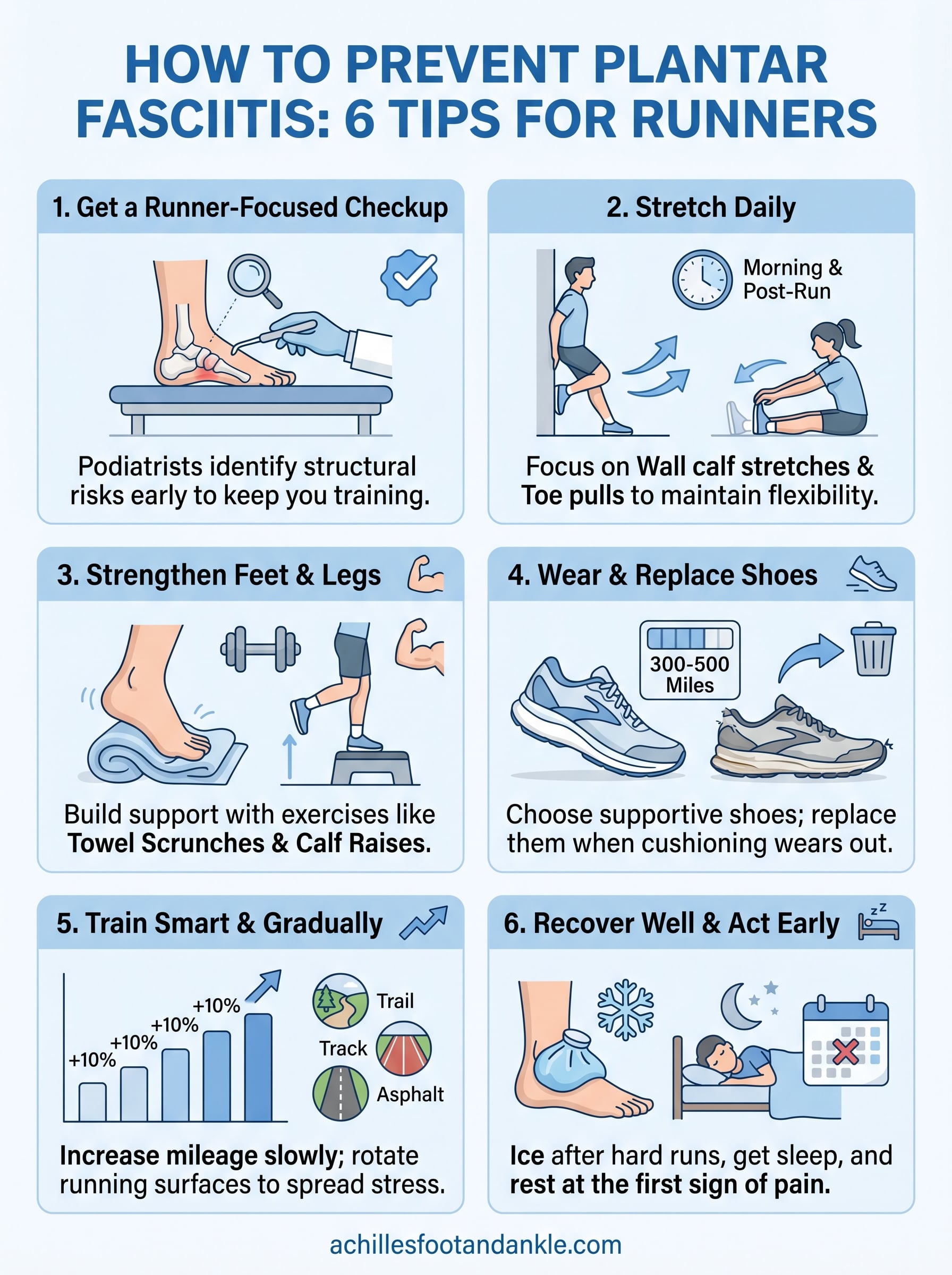
This guide breaks down six practical tips, covering footwear choices, stretching routines, strengthening exercises, and training adjustments, that can help you keep your plantar fascia healthy and your running schedule intact. Each recommendation comes from what we see work in clinical practice, not generic advice pulled from a textbook.
1. Get a runner-focused foot and ankle checkup
Most runners skip professional foot evaluations until something hurts, but a proactive checkup is one of the most effective steps you can take when thinking about how to prevent plantar fasciitis. A podiatrist who works with runners can identify structural vulnerabilities before they become injuries, which means you spend more time training and less time managing pain.
What a podiatrist looks for in runners
During a runner-focused exam, your podiatrist evaluates foot structure, arch height, and tissue flexibility to identify factors that increase plantar fascia strain. Flat feet, high arches, and tight Achilles tendons all place extra load on the plantar fascia during the push-off phase of your stride. Your podiatrist also checks ankle range of motion and heel alignment, since limited dorsiflexion is one of the most consistent predictors of heel pain in runners.
A thorough exam may also include standing X-rays to assess bone positioning and any signs of heel spurs, which frequently develop alongside chronic plantar fascia stress. Understanding your full foot profile gives your provider a clear baseline, so if symptoms do develop later, they have something concrete to compare against.
How a gait and footwear review lowers risk
Watching you walk or jog, even briefly, gives a clinician direct evidence of how your foot strikes the ground and how your arch responds to load. Overpronation, where your arch collapses inward with each step, places repeated stress on the plantar fascia across every mile you log. A gait review paired with a look at your current shoes can reveal wear patterns that confirm whether your footwear is protecting or undermining your heel.
Getting your gait assessed by a specialist costs far less time and money than treating a full plantar fasciitis flare-up that sidelines you for months.
When to book an appointment instead of DIY
Schedule a checkup if you are significantly increasing your weekly mileage, returning to running after a long break, or consistently training on hard surfaces like asphalt or concrete. You do not need to wait for pain to appear. Runners with a history of heel pain, flat feet, or previous plantar fasciitis benefit most from a professional evaluation before ramping up any training load.
2. Stretch your calves and plantar fascia daily
Daily stretching is one of the most consistently supported habits for how to prevent plantar fasciitis before it takes hold. Tight calves and a stiff Achilles tendon pull directly on the plantar fascia with every stride, so keeping these tissues flexible reduces the load your heel absorbs across every mile you run.
The key stretches that protect your heel
Two stretches deliver the most value for runners targeting heel health:

- Standing wall calf stretch: Press your heel flat to the floor, lean into the wall, and hold 30 seconds. Repeat with a slightly bent knee to hit the soleus separately.
- Toe pull plantar fascia stretch: Sitting down, pull your toes back toward your shin and hold for 30 seconds. Perform three repetitions per foot each session.
When to stretch for best results
Perform both stretches before you take your first steps in the morning, since the plantar fascia tightens overnight and morning loading is when micro-tears most commonly occur. Running a second session right after your workout, while tissue is still warm, compounds the flexibility gains over time.
Runners who build morning stretching into a daily habit reduce their exposure to the sharp first-step heel pain that signals early plantar fascia stress.
Form cues that prevent overstretching and flare-ups
Keep your heel fully grounded during every calf stretch and stop well short of sharp discomfort. A gentle pulling sensation is the target, and pain during the stretch means you have gone too far, which can aggravate already stressed tissue rather than protect it.
3. Strengthen your feet and lower legs
Stretching addresses flexibility, but strength is what protects your plantar fascia under load. Runners who build foot and lower leg strength give their tissue a far better chance of handling the repetitive forces of training, which is a key part of understanding how to prevent plantar fasciitis long term.
Foot intrinsic moves that support your arch
The small muscles inside your foot, called intrinsic muscles, control arch stability with each ground contact. Two simple exercises target them directly:
- Towel scrunches: Place a small towel on the floor and scrunch it toward you using only your toes. Do 3 sets of 15 reps per foot.
- Short foot exercise: While seated, draw your toes toward your heel without curling them, creating a short, domed arch. Hold for 5 seconds and repeat 10 times per foot.
Calf and ankle strengthening that reduces strain
Single-leg calf raises are the most practical move for reducing plantar fascia strain, since they build the strength needed to absorb landing impact through each stride. Perform 3 sets of 15 repetitions per leg, progressing to a slow 3-second lowering phase once bodyweight becomes manageable.
Runners who strengthen their calves reduce the compensatory load that transfers directly down to the plantar fascia during push-off.
A simple weekly progression you can stick with
Start with two strength sessions per week and add one repetition per set every two weeks. This slow build lets your tissue adapt without triggering irritation.
4. Wear supportive running shoes and replace them on time
Your footwear choices directly influence how much stress your plantar fascia absorbs with every stride. Choosing the right shoe, and knowing when to retire it, is a practical and underrated part of understanding how to prevent plantar fasciitis before it derails your training.
What to look for in a shoe if you get heel pain
Look for a running shoe with firm arch support and adequate heel cushioning to reduce the load transferred to your plantar fascia at each foot strike. Runners with flat feet benefit from motion control or stability shoes, while those with high arches often need extra cushioning to compensate for reduced natural shock absorption.

A shoe fitting at a specialty running store where staff can assess your foot type gives you a far more accurate match than ordering based on brand alone.
How to tell when shoes stop supporting you
Most running shoes lose meaningful cushioning and structural support between 300 and 500 miles, even when the outsole still looks intact. Check for compression in the midsole and uneven heel wear, both of which signal that the shoe is no longer absorbing impact effectively.
When inserts and orthotics make sense
Off-the-shelf inserts can add short-term arch support if your current shoes lack structure. Custom orthotics prescribed by a podiatrist go further by correcting biomechanical issues specific to your foot, making them the better option for runners with recurring heel pain or pronounced structural imbalances.
5. Build mileage gradually and train smart
How you structure your training load matters just as much as your footwear and stretching habits. Rapid mileage increases are one of the most common triggers for plantar fasciitis in runners, and smart training progression is a core part of how to prevent plantar fasciitis from disrupting your season.
How to increase weekly volume without overloading tissue
The standard guideline is no more than a 10 percent increase in weekly mileage, and your plantar fascia adapts slowly to load. Pushing beyond that threshold leaves no recovery window between sessions, which is when cumulative stress builds into an actual injury.
Consistent small increases compound into significant mileage gains over a full training cycle without the tissue damage that forces you to take weeks off.
Why hills, speed work, and long runs trigger issues
Steep inclines and descents both increase the stretch demand on your plantar fascia, while speed work amplifies the impact force of each foot strike. Combining multiple high-stress sessions in the same week raises your injury risk significantly.
Long runs accumulate fatigue across your entire lower leg, leaving the plantar fascia less supported in the final miles when your form deteriorates and compensatory strain increases across the heel.
How to rotate surfaces and workouts to spread stress
Hard surfaces like concrete and asphalt concentrate impact directly into your heel with each step. Mixing in softer surfaces such as packed trails or rubberized track gives your plantar fascia periodic relief between harder training days.
Alternating easy days with harder sessions and distributing different workout types across the week prevents any single stress pattern from overloading the same tissue repeatedly.
6. Recover well and respond early to warning signs
Recovery is often where runners lose ground when it comes to how to prevent plantar fasciitis from becoming a recurring problem. Training stress without sufficient downtime gives the plantar fascia no window to rebuild between sessions, which is precisely how minor irritation turns into a stubborn injury that costs you months of training.
Recovery habits that keep the plantar fascia calm
Icing your heel for 15 minutes after long runs or hard sessions controls cumulative inflammation before it has a chance to build into persistent pain. Prioritize 7 to 9 hours of sleep each night, since connective tissue repair happens during rest, and runners who consistently under-sleep face a higher soft tissue injury risk overall.
Early symptoms runners should not ignore
Morning heel pain during your first steps out of bed and arch tenderness that lingers after runs are the two clearest early signals that your plantar fascia is under stress. Pushing through either symptom at full training volume turns a manageable situation into a prolonged recovery.
Catching these signs early and pulling back for a few days costs far less time than weeks of forced rest from a full flare-up.
What to do in the first 72 hours if pain starts
Act quickly when heel pain first appears. Reduce training volume immediately and replace high-impact sessions with swimming or cycling to maintain fitness without aggravating the tissue.
- Apply ice twice daily for 15 to 20 minutes
- Resume daily calf and plantar fascia stretches
- Check your shoes for midsole compression
- Book a podiatrist appointment if pain continues past 72 hours
Next steps if you want to stay ahead of heel pain
These six tips give you a clear, actionable framework for how to prevent plantar fasciitis before it ever interrupts your training. Consistency across all six areas, from daily stretching to smart mileage progression, matters far more than perfecting any single habit. Small, steady actions compound into real protection for your plantar fascia over a full running season, and that protection adds up quickly when you stay disciplined about each one.
That said, no amount of self-management replaces an expert eye on your specific foot structure and training habits. If you have a history of heel pain, notice early warning signs, or are ramping up your mileage this season, a podiatrist who works with runners can catch problems before they develop into injuries. Our team at Achilles Foot and Ankle Center is ready to help you train longer with less risk. Book a same-day appointment and get a runner-focused foot and ankle evaluation today.






