Most people associate gout with the big toe, and for good reason, since that’s where it strikes most often. But gout doesn’t always follow the textbook. If you’ve been dealing with sudden, intense heel pain and haven’t found answers, you may be wondering: can gout cause heel pain? The short answer is yes. Uric acid crystals can deposit in the heel joint, triggering inflammation and pain that’s often mistaken for plantar fasciitis or other common conditions.
The distinction matters because treating the wrong diagnosis means prolonged pain and potential joint damage. Gout in the heel has its own set of characteristics, and it requires a different treatment approach than most mechanical causes of heel pain. At Achilles Foot and Ankle Center, our podiatrists across Central Virginia regularly evaluate patients whose heel pain turns out to be gout-related rather than structural.
This article breaks down how gout affects the heel, what symptoms to watch for, how it’s diagnosed, and what treatment options actually work, so you can take the right steps toward relief.
Why gout can show up as heel pain
Gout is a form of inflammatory arthritis caused by a buildup of uric acid in the blood. When uric acid levels get too high, the body can no longer dissolve the excess, and it crystallizes into sharp, needle-like deposits inside joints and surrounding soft tissue. Most people know this happens in the big toe, but gout can settle in any joint, including the ones in your heel.
How uric acid crystals affect the heel
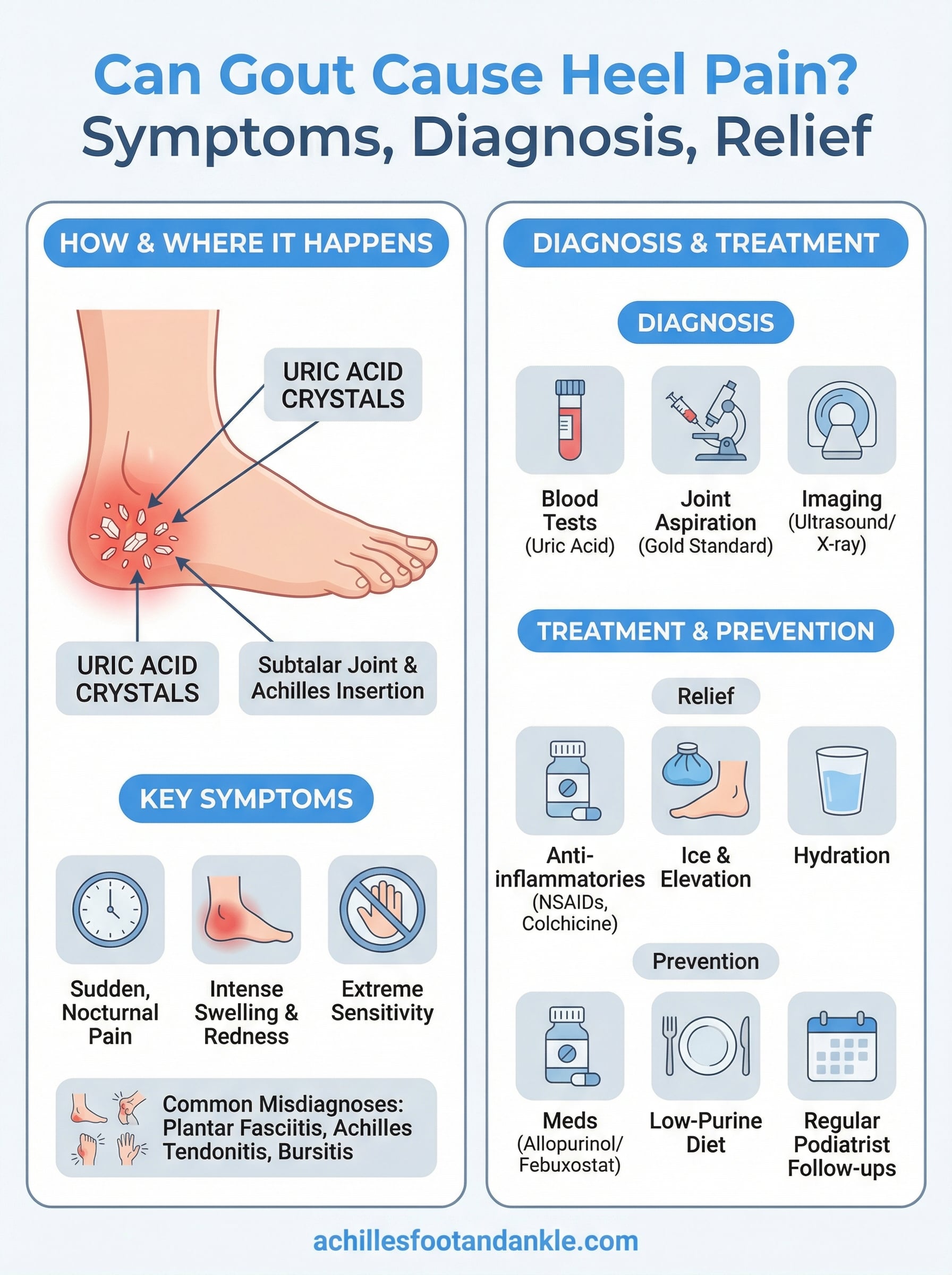
The heel contains two structures that gout commonly targets: the subtalar joint (where your heel bone meets the ankle bone) and the area around the Achilles tendon insertion. When uric acid crystals accumulate in either location, your immune system recognizes them as foreign and launches an inflammatory response. That response floods the area with white blood cells, causing intense swelling, heat, and pain that make gout flares hard to ignore.

Gout-related heel pain can appear suddenly, often overnight, and may feel like a severe sprain even when no injury occurred.
Your heel absorbs an enormous amount of force with every step, roughly 1.5 times your body weight during normal walking. That mechanical stress can make the heel more susceptible to crystal accumulation over time, particularly if your uric acid levels stay elevated for months or years without treatment.
Why gout in the heel gets misdiagnosed
Many patients asking can gout cause heel pain never get a clear answer because the symptoms closely resemble other conditions. Plantar fasciitis, Achilles tendinopathy, and heel bursitis all produce pain in similar areas, and without blood work or imaging, the presentations can look nearly identical.
Gout in the heel also tends to flare and then resolve on its own within days, which leads many people to assume the problem went away rather than seeking a proper diagnosis. These conditions are frequently confused with gout:
- Plantar fasciitis
- Achilles tendinopathy
- Heel bursitis
- Stress fractures
That cycle of flares and remissions is exactly why gout damage builds quietly over time before becoming a more serious joint problem.
Signs your heel pain may come from gout
Knowing whether gout can cause your specific heel pain comes down to recognizing a distinct pattern. Gout flares behave differently from most structural heel problems, and paying close attention to how and when your pain begins gives you critical information before you ever see a provider.
The hallmark symptoms of a gout flare
Gout-related heel pain typically arrives without warning, often waking you in the middle of the night with intense, throbbing pain. Within hours, the affected area becomes visibly swollen, red, and warm to the touch. Even light pressure from a bedsheet or sock can feel unbearable at the height of a flare.
Most gout flares resolve within 7 to 10 days on their own, but the underlying problem remains and will trigger another episode without proper treatment.
Your pain may also include limited range of motion in the heel or ankle and significant difficulty bearing weight. Flares frequently follow recognizable triggers such as alcohol consumption, dehydration, high-purine foods like red meat or shellfish, or a recent illness or surgery.
Less obvious signs to watch for
Some indicators are easier to miss entirely. Repeated episodes of unexplained heel pain that come and go over several months point strongly toward gout rather than a one-time injury. You may also develop small, firm lumps near the heel called tophi, which appear when uric acid crystals accumulate under the skin after prolonged elevated levels. Watch for these additional warning signs:
- Pain that shifts between different joints rather than staying fixed in one spot
- Heel discomfort that consistently follows rich meals or alcohol
- A personal or family history of gout diagnoses elsewhere in the body
Gout vs plantar fasciitis and other heel problems
Understanding whether gout can cause heel pain in your case becomes much clearer once you know how it compares to other common diagnoses. The location of pain can overlap significantly, but the pattern, timing, and associated symptoms differ in ways that point a trained provider toward the right answer.
How gout differs from plantar fasciitis
Plantar fasciitis causes pain along the bottom of the heel, typically worst with your first steps in the morning and improving as you walk. Gout flares, by contrast, often peak without any activity at all and get worse rather than better with movement. Plantar fasciitis develops gradually through repetitive strain, while gout arrives suddenly, often within hours.
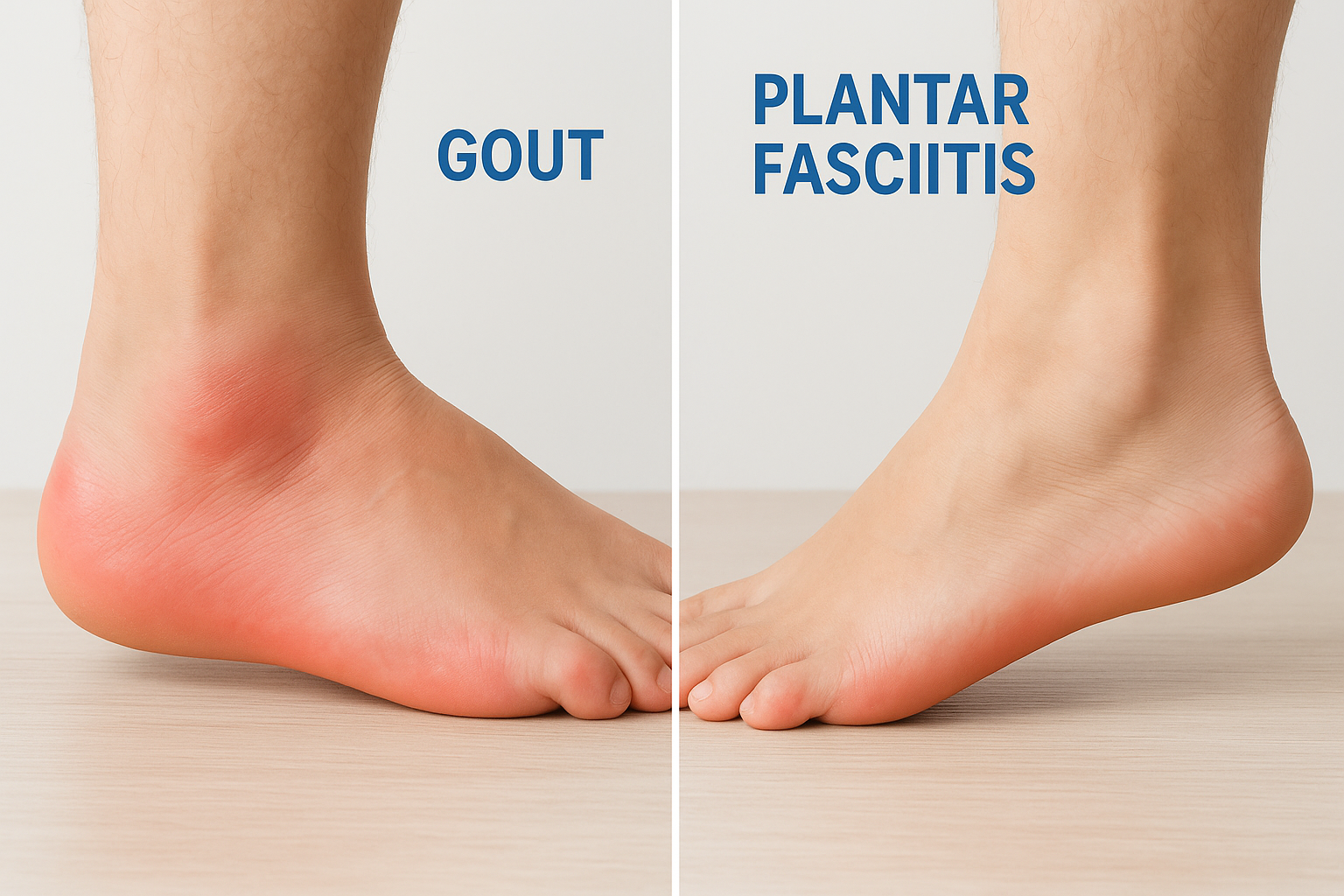
If your heel pain is also hot, visibly red, and swollen, plantar fasciitis is rarely the cause since inflammation that severe points toward a systemic condition like gout.
Another key difference is response to rest. Plantar fasciitis generally feels better after a night of sleep, but gout can make the pressure of your bedsheet against your heel nearly unbearable. That level of sensitivity is a strong distinguishing sign.
When other conditions overlap with gout
Heel bursitis and Achilles tendinopathy also mimic gout because they cause localized swelling and tenderness near the heel. However, both of those are mechanical conditions tied to overuse or poor biomechanics rather than elevated uric acid levels in the blood. A stress fracture can produce sudden heel pain too, but it typically follows a period of increased activity rather than appearing after a rich meal or a night of drinking.
How providers diagnose gout in the heel
When can gout cause heel pain is the question your provider is working to answer, diagnosis involves more than a physical exam. Because gout symptoms overlap so closely with mechanical conditions, providers combine clinical evaluation, laboratory testing, and imaging to reach a confident conclusion rather than guessing based on appearance alone.
Blood and fluid tests
A serum uric acid test measures the concentration of uric acid in your blood, but it comes with an important caveat: uric acid levels can actually drop during an active flare, which means a normal result does not automatically rule gout out. Your provider may order the test between episodes for a more reliable reading.
The most definitive way to confirm gout is by analyzing fluid drawn directly from the affected joint under a microscope, where uric acid crystals appear as sharp, needle-like structures.
This procedure, called joint aspiration or arthrocentesis, involves withdrawing a small amount of synovial fluid from the heel joint and examining it for crystal deposits. It remains the gold standard for diagnosis and removes any ambiguity about the underlying cause.
Imaging to assess joint damage
Your provider may also use X-rays or musculoskeletal ultrasound to evaluate the heel. X-rays can reveal bone erosion or tophi deposits in patients with long-standing gout, while diagnostic ultrasound detects crystal deposits and joint inflammation in real time, even during early-stage disease. MRI is occasionally ordered when the clinical picture remains unclear or when ruling out a stress fracture is necessary.
How to get relief and prevent future flares
Once you confirm that gout can cause heel pain in your case, treatment targets two goals at once: stopping the current flare and lowering uric acid levels to prevent the next one. Addressing only the acute pain without managing the underlying cause keeps you in a cycle of recurring episodes that gradually damage the joint.
Managing an active flare
Anti-inflammatory medications are the first line of treatment during a flare. Your provider may prescribe NSAIDs, colchicine, or corticosteroids depending on your health history and how severe the episode is. Each option works to interrupt the immune response driving the inflammation in your heel.
Starting treatment within the first 24 hours of a flare significantly reduces how long it lasts and how severe it becomes.
Elevating your foot and applying ice wrapped in a cloth for 20-minute intervals reduces swelling quickly. Staying well-hydrated also helps your kidneys clear excess uric acid and can shorten flare duration.
Preventing future episodes
Long-term uric acid management is what separates patients who keep having flares from those who don’t. Your provider may prescribe allopurinol or febuxostat to reduce uric acid production over time. Consistent lifestyle changes reinforce the medication’s effect. Focus on:
- Limiting high-purine foods like organ meats, shellfish, and alcohol
- Drinking enough water daily to support kidney function
- Maintaining a stable weight and avoiding crash diets
- Scheduling regular follow-ups to monitor uric acid levels
This combination of medication and habit changes keeps your uric acid in a range where crystals stop forming and flares become far less frequent.
What to do next
If you’ve been wondering whether gout can cause heel pain and you recognize the symptoms described here, your next step is getting a proper diagnosis from a qualified podiatrist. Self-treating without confirming the underlying cause almost always leads to longer recovery times and ongoing joint damage.
A podiatrist can run blood work, perform joint aspiration, and use diagnostic imaging to pinpoint exactly what’s driving your symptoms and build a treatment plan that addresses both the active flare and long-term uric acid control. Achilles Foot and Ankle Center providers across Central Virginia have the experience to identify gout-related heel pain quickly and get you back on your feet without prolonged guesswork.
Don’t wait for another flare to stop you in your tracks. Same-day appointments are available, so you can get answers and start the right treatment without delay. Book a same-day appointment and take the first step toward lasting relief.






