Diabetes affects roughly 37 million Americans, and up to 34% of them will develop a foot ulcer in their lifetime. That’s not a scare tactic, it’s a reality our podiatrists at Achilles Foot and Ankle Center see every day across our Central Virginia clinics. The good news? Most of these complications are preventable when you know how to care for diabetic feet properly.
High blood sugar damages nerves and reduces blood flow to your feet over time. Small cuts, dry skin, or a blister you barely notice can quickly escalate into an infection or non-healing wound. Daily foot care isn’t optional when you have diabetes, it’s one of the most important things you can do to protect your mobility and avoid serious outcomes like hospitalization or amputation.
This guide breaks down the practical, everyday steps you can take to keep your feet healthy. From inspecting your skin and choosing the right footwear to recognizing early warning signs that need professional attention, we’ll cover what actually works based on our team’s experience treating diabetic foot conditions at every stage. Whether you were recently diagnosed or have been managing diabetes for years, these tips will give you a clear routine to follow starting today.
Why diabetic foot care matters every single day
Most people with diabetes understand that blood sugar management affects their heart, kidneys, and eyes. Fewer realize how directly it threatens their feet, often before any obvious symptoms show up. Learning how to care for diabetic feet is not a one-time task you check off a list. It requires consistent daily attention because the underlying changes diabetes causes in your body are always at work, even when your feet feel fine.
The connection between blood sugar and foot health
Persistently elevated blood sugar damages small blood vessels and nerves throughout your body over time. In your feet, this creates two compounding problems: peripheral neuropathy and peripheral artery disease. Peripheral neuropathy reduces or completely eliminates your ability to feel pain, pressure, heat, or injury in your feet. Peripheral artery disease limits the blood supply that your tissue needs to heal. Together, these two conditions turn minor foot problems into serious medical events faster than most people expect.
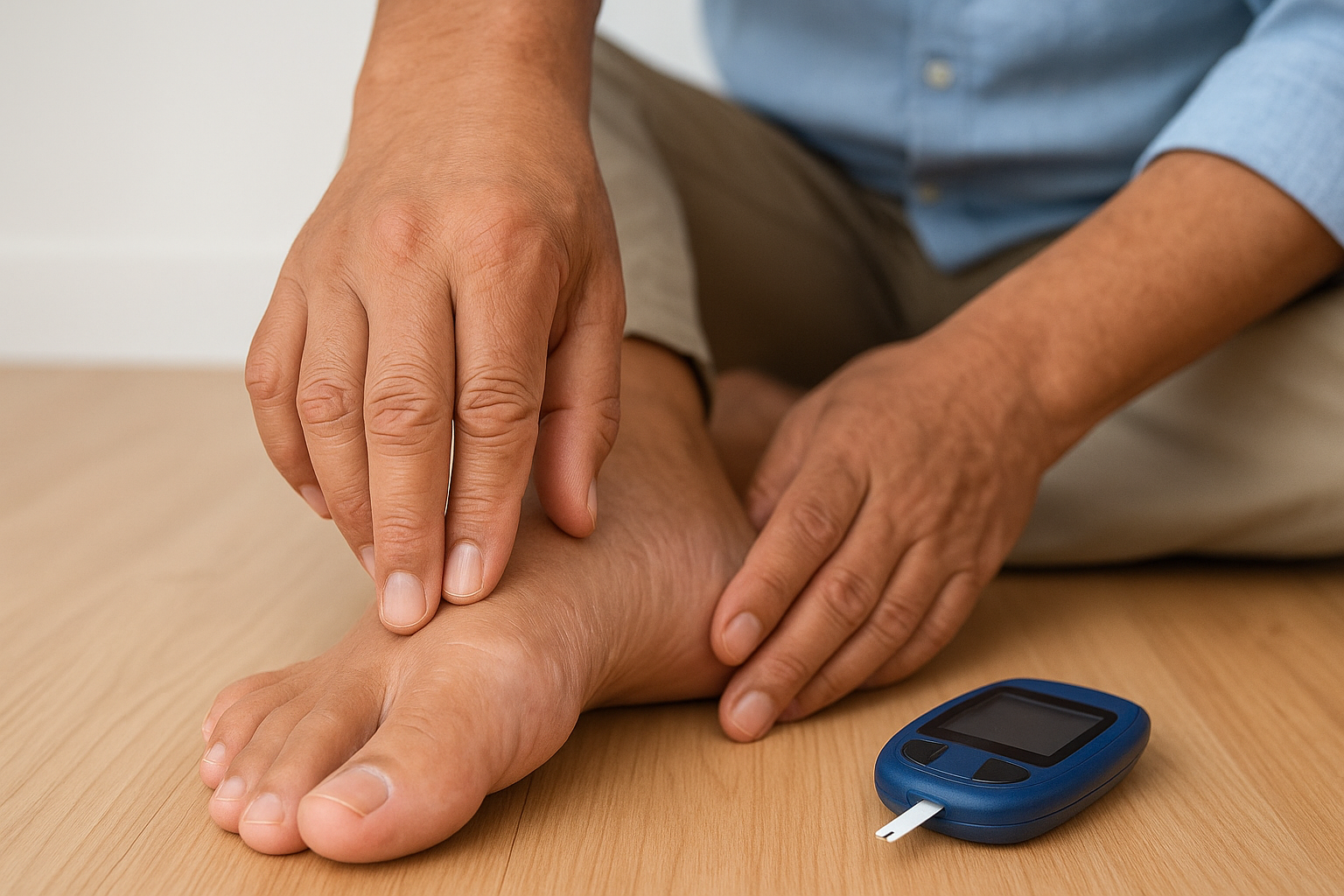
When your feet can’t feel pain and your circulation is reduced, your body loses its two main defenses against infection and tissue damage.
Your feet log more physical stress than any other part of your body. Every step you take puts pressure, friction, and force through the same small area of skin and bone. For someone without diabetes, that stress produces minor irritation that heals quickly. For you, the same stress can create a wound that your body struggles to recognize and repair.
What nerve damage actually does to your daily risk
Neuropathy doesn’t always feel like numbness. Many people with diabetic nerve damage first notice tingling, burning, or sharp pain, especially at night. Others feel nothing at all in parts of their foot. Both situations are dangerous because they disrupt your normal feedback system. You might step on a sharp object, develop a pressure sore from a tight shoe, or crack your skin during cold weather and never feel it happen.
The skin on diabetic feet also changes. Reduced sweating from nerve damage dries out your skin faster, leading to cracks and fissures that open the door to bacteria. Your foot structure can shift as the small muscles in your foot weaken, creating new pressure points under the ball of your foot or over your toes. These mechanical changes happen gradually and silently, which is exactly why daily checks matter.
Why small problems escalate quickly
A healthy immune system responds to bacteria at a wound site with immediate inflammation, increased blood flow, and localized infection-fighting. With diabetes, impaired circulation slows that response significantly. Bacteria can spread into deeper tissue, bone, and the bloodstream before your body mounts an effective defense. This progression from a small cut to a limb-threatening infection can happen within days in severe cases.
Diabetic foot ulcers are the leading cause of non-traumatic lower limb amputations in the United States. According to data reviewed by the American Diabetes Association, people with diabetes are 10 to 20 times more likely to need an amputation than those without the condition. The overwhelming majority of these amputations follow an ulcer that either went unnoticed or was not treated early enough.
The encouraging reality is that most amputations are preventable with the right habits in place. Daily foot inspections, proper hygiene, appropriate footwear, and prompt professional care when something looks wrong form the foundation of prevention. None of these steps are complicated, but all of them require consistency. Your feet are working hard every single day, and they deserve the same level of attention you give to your blood sugar readings or your medication schedule.
Step 1. Check your feet daily for early warning signs
Daily foot inspection is the single most important habit in learning how to care for diabetic feet. Because nerve damage may prevent you from feeling cuts, blisters, or pressure sores, your eyes become your first line of defense. Schedule your inspection at the same time each day, such as right after your shower or before bed, so it becomes a fixed part of your routine rather than something you do when you remember.
What to look for during your daily inspection
Your inspection needs to be thorough and systematic, not a quick glance before you put on your socks. Examine every surface of your foot, including between the toes and along the heel, where problems often start unnoticed. Use a hand mirror or a long-handled mirror to see the bottom of your foot clearly, or ask a family member to help if bending is difficult. Bright, direct lighting makes it much easier to spot subtle color changes or small wounds before they worsen.
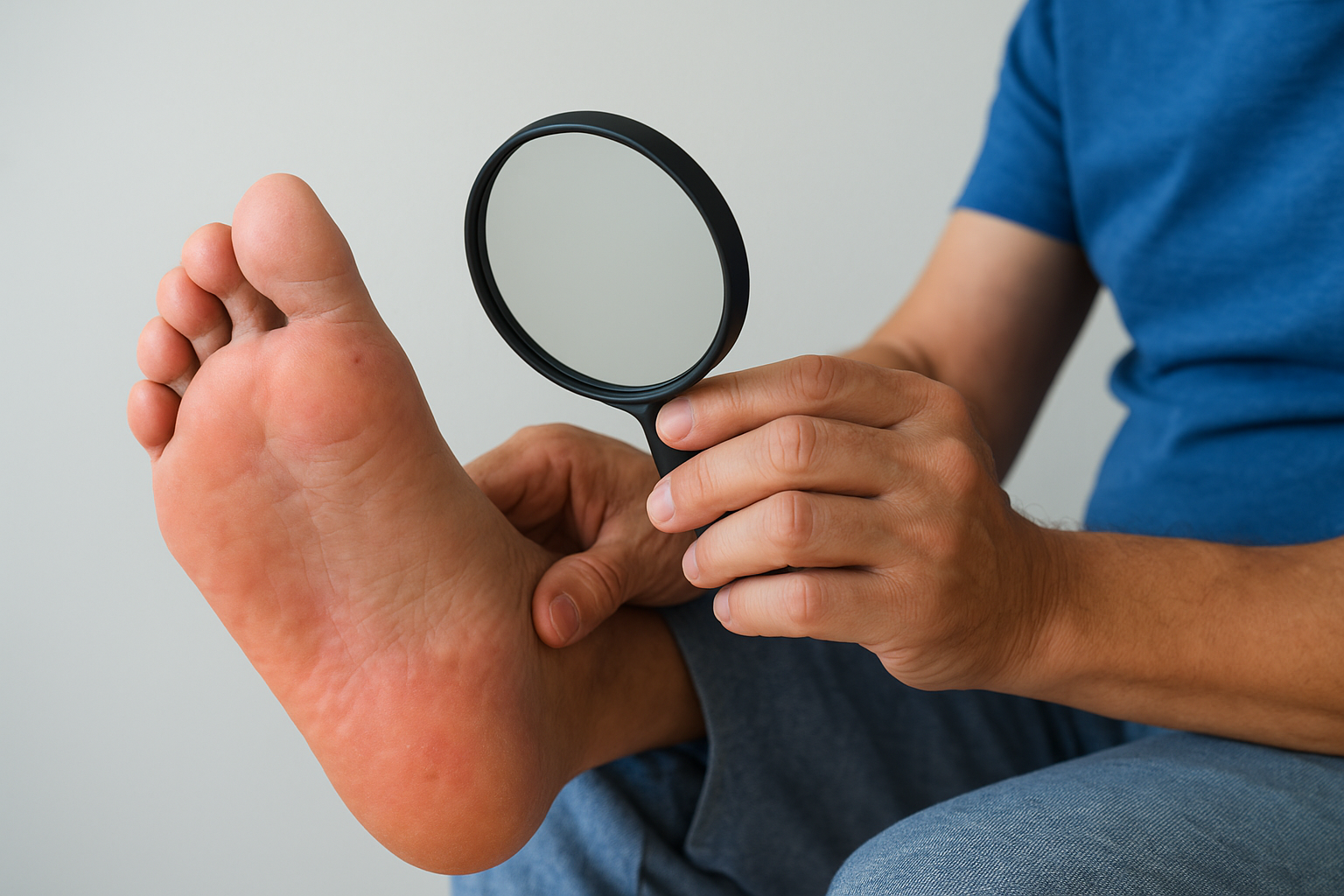
Look for these specific warning signs every time:
- Redness, swelling, or warmth in any area, which can signal early infection
- Cuts, cracks, or open sores, even tiny ones that seem minor
- Blisters or calluses that have changed in size, shape, or color
- Discoloration, including dark spots, pale patches, or unexplained bruising
- Ingrown toenails or nails that appear thickened or discolored
- Unusual odor, which can indicate infection or early tissue breakdown
If you spot anything that was not there the day before, do not wait to see if it resolves on its own. Contact your podiatrist that same day.
Building a daily inspection routine that sticks
The biggest barrier to daily inspection is forgetting to do it consistently. Linking the habit to something you already do each day makes it far more reliable. For example, keep a small mirror on your nightstand and do your check the moment you sit on the edge of the bed before sleep. This approach ties the new behavior to an existing one, which makes it much harder to skip.
Document anything unusual by taking a photo with your phone and noting the date. A visual record helps your podiatrist see exactly how a wound or skin change has progressed and whether it needs urgent care or monitoring. A brief note in your phone’s calendar takes under 30 seconds and gives your care team far more useful information than your memory alone can provide at an appointment.
Step 2. Wash and dry your feet the safe way
Washing your feet seems straightforward, but the standard approach most people use can cause real harm when you have diabetes. Water temperature and drying technique matter far more than most patients realize, and getting either wrong can create the very skin damage you are working to prevent. Understanding how to care for diabetic feet through proper hygiene is one of the simplest adjustments you can make with an immediate impact on your daily risk level.
Getting the temperature and technique right
Peripheral neuropathy makes it difficult or impossible to accurately judge water temperature by feel, which means water you think is comfortable may actually be hot enough to scald your skin. Before putting your feet in any water, test the temperature with your elbow or a bath thermometer. The water should be lukewarm, between 90 and 95 degrees Fahrenheit, which is noticeably cooler than what most people prefer for a bath or shower.

Never soak your feet for extended periods. Prolonged soaking softens and breaks down your skin barrier, making it more vulnerable to cracks and infection.
Use a mild, fragrance-free soap applied gently with your hands or a soft washcloth. Avoid scrubbing between your toes harshly, since the skin there is thin and prone to small tears. Keep your wash time to a few minutes rather than a long soak. If you shower rather than bathe, let warm water run over your feet and wash them directly with your hand, keeping the process gentle throughout.
Why drying matters as much as washing
After washing, thorough but careful drying is just as critical as the wash itself. Moisture left between your toes creates the warm, damp environment that fungi and bacteria need to thrive, which can lead quickly to athlete’s foot or skin breakdown. Pat your feet dry with a soft towel rather than rubbing, since rubbing can irritate fragile skin or tear areas you may not be able to feel.
Pay particular attention to the spaces between each toe, using a corner of your towel or a separate dry cloth to gently absorb any remaining moisture. Once your feet are fully dry, apply moisturizer to the tops and bottoms of your feet, but keep it away from the areas between your toes where extra moisture causes harm rather than helps. This two-minute drying routine is a small effort that directly reduces your risk of daily skin complications.
Step 3. Protect your skin barrier and prevent cracking
Your skin is your body’s first physical defense against bacteria and infection. When you have diabetes, dry skin and cracking are not just cosmetic problems, they are actual entry points for bacteria that can start a serious infection. Protecting your skin barrier is a core part of learning how to care for diabetic feet, and it takes less than two minutes built into your daily routine.
Choose the right moisturizer and apply it consistently
Not every lotion works well for diabetic feet. You need a thick, fragrance-free moisturizing cream or urea-based lotion rather than a thin, watery product that evaporates quickly. Formulas with urea or lactic acid work particularly well because they pull moisture into dry skin and help soften thickened areas without causing irritation. Apply your moisturizer immediately after drying your feet, when your skin is still slightly warm from washing, so it absorbs more effectively.
Apply moisturizer to the tops and bottoms of your feet, but always skip the spaces between your toes to avoid creating the damp conditions that lead to fungal infections.
Consistency matters more than the specific brand you choose. Pick one product, keep it next to wherever you do your daily foot check, and apply it every single day. If your skin still feels rough or cracked despite regular moisturizing, mention it to your podiatrist, since a prescription-strength cream may be more effective for your skin type.
Prevent heel cracks before they become open wounds
Heel fissures are among the most common and most overlooked foot problems for people with diabetes. The thick, dry skin on your heel splits under pressure and forms cracks that can reach deep into the dermis, where bacteria can enter directly. Wearing open-back shoes or sandals accelerates this process by allowing your heel skin to spread outward without support and dry out faster.
Switching to enclosed, supportive footwear reduces heel pressure and slows the drying process significantly. If you already have minor heel cracks, apply a thick barrier cream such as petroleum jelly over the area at night and cover it with a clean cotton sock to lock in moisture while you sleep. Check the crack each morning during your inspection. Any crack that shows redness, extends beyond the outer skin layer, or bleeds needs same-day attention from your podiatrist rather than continued home treatment.
Step 4. Trim toenails safely and avoid DIY callus care
Toenail trimming is one of the most underestimated risks in learning how to care for diabetic feet. What seems like a routine grooming task becomes genuinely dangerous when reduced sensation means you cannot feel a nick, and impaired circulation means that small wound heals slowly or not at all. Getting your technique right, and knowing which tasks to leave to a professional, prevents a significant number of preventable infections.
How to trim your toenails correctly
The right time to trim your nails is right after your daily wash, when the nails are slightly softer and easier to cut cleanly. Use a pair of straight-edged nail clippers rather than curved ones, and cut straight across each nail rather than rounding the corners. Cutting into the corners is one of the primary causes of ingrown toenails, which in diabetic feet can escalate into a serious infection within days.
Never cut your nails so short that you expose the skin underneath, since that raw edge creates an immediate entry point for bacteria.
Follow these specific steps each time you trim:
- Sit in good lighting with your foot at a comfortable height so you can see clearly
- Cut in small, straight increments rather than one large clip to avoid splitting the nail
- File any sharp edges gently with an emery board after cutting
- Check the surrounding skin for redness or swelling before and after the trim
- Stop immediately and contact your podiatrist if you nick the skin or draw blood
If your nails are thickened, discolored, or curved, do not attempt to trim them yourself. Thick nails require professional tools and technique to cut safely, and a podiatrist can handle them at a routine visit without any risk to your skin.
Why callus removal at home puts you at risk
Calluses form as your body’s response to repeated pressure or friction, and they are extremely common in people with diabetes due to altered foot mechanics and pressure distribution. Many people reach for a pumice stone, callus file, or over-the-counter callus remover pads to handle them at home. All three options carry real risk when you have reduced sensation, since you can remove too much tissue without realizing it, leaving a raw, vulnerable surface.
Chemical callus removers are especially problematic because they contain salicylic acid, which does not stop working at the callus layer. These products can break down healthy surrounding skin and create open wounds. Bring any calluses to the attention of your podiatrist instead, who can safely reduce them with professional tools and assess the underlying pressure patterns causing them.
Step 5. Choose socks and shoes that prevent pressure spots
Footwear is one of the most direct factors in how to care for diabetic feet effectively, yet many people with diabetes continue wearing shoes and socks that create friction, pressure, and moisture without realizing the damage accumulating over time. Your feet spend most of the day enclosed and under load, which means every fit problem, seam, or material choice compounds with each step you take.
What to look for in diabetic socks
Standard cotton socks trap moisture and often contain thick seams across the toe box that press against your skin with every step. That constant, low-level pressure can cause blisters or skin breakdown you will not feel until significant damage has already occurred. Diabetic-specific socks are designed to eliminate those risks through their construction.
Look for socks labeled "seamless" or "non-binding" and made from moisture-wicking materials like bamboo, wool blend, or synthetic fibers designed to pull sweat away from your skin.
When selecting socks, check for these specific features:
- No elastic band at the top that could restrict circulation around your ankle or calf
- Seamless toe closures or hand-linked seams that sit flat against your skin
- Cushioned sole panels that add padding under the ball of the foot and heel without adding bulk
- Light or white color so any discharge, bleeding, or drainage from a wound shows up clearly when you remove them
- Correct fit with no bunching, since excess fabric folds into pressure points just like seams do
How to select shoes that fit and protect
Shoes need a wide, deep toe box that allows your toes to sit flat without any digit being pushed against the material above or beside it. Lace-up or adjustable closures give you the ability to accommodate any swelling that develops throughout the day, which is common for people with diabetes. Avoid slip-on styles without adjustment options because your foot will shift forward inside the shoe with each step, increasing friction at the toes and heel.

Always shop for shoes in the afternoon or evening, when your feet are at their largest after daily activity and any normal swelling has developed. Bring your orthotic insoles or diabetic inserts with you so the shoe fits correctly with them inside, not without them. Replace worn shoes before the cushioning compresses completely, since a flat sole transfers significantly more pressure into your foot with every step you take.
Step 6. Improve circulation and reduce nerve damage risks
Poor circulation is one of the core reasons diabetic foot injuries heal so slowly, and improving blood flow to your feet is something you can actively influence through daily choices. This step in learning how to care for diabetic feet focuses on what you can do with your body and your habits to keep blood moving and slow the progression of nerve damage over time.
Move your body to keep blood flowing
Regular physical movement is one of the most effective tools you have for improving peripheral circulation. Low-impact activities like walking, swimming, and cycling all stimulate blood flow to your lower limbs without putting excessive force through vulnerable areas of your foot. Even short sessions make a difference, and you do not need intense exercise to see results.
Aim for at least 30 minutes of low-impact movement most days of the week, broken into smaller sessions if needed, to consistently support circulation to your feet.
A simple daily routine you can follow looks like this:
- Morning: 10-minute walk after breakfast to stimulate circulation early in the day
- Midday: 5 minutes of seated ankle rotations and toe flexes at your desk or in a chair, rotating each ankle clockwise and counterclockwise 10 times per direction
- Evening: 10-minute walk after dinner, which also supports blood sugar control after meals
- Before bed: Elevate your feet on a pillow for 15 minutes to reduce swelling if it developed during the day
These movements keep blood circulating through the small vessels in your feet and reduce the pressure that builds from extended sitting or standing.
Avoid habits that cut off circulation
Certain everyday habits restrict blood flow to your feet in ways that compound the vascular damage diabetes already causes. Sitting with your legs crossed for extended periods compresses the blood vessels behind your knee and reduces circulation to everything below it. Make a conscious effort to keep both feet flat on the floor when you sit, and stand up to walk around for a minute or two at least once every hour.
Smoking is one of the most damaging circulatory habits for anyone with diabetes because it constricts small blood vessels directly and accelerates peripheral artery disease. Extreme cold also causes blood vessels to narrow, so keep your feet warm during cold weather with proper socks and enclosed shoes rather than warming them near a heat source, which your neuropathy may prevent you from accurately sensing.
Step 7. Know when to call a podiatrist right away
Even with a solid daily routine covering how to care for diabetic feet, problems can still develop. The difference between a minor complication and a serious one often comes down to how quickly you act when something changes. Knowing which signs require same-day contact with your podiatrist removes the guesswork and gives you a clear threshold to act on rather than a vague sense that something might be wrong.
Warning signs that need same-day attention
Some changes on your feet cannot wait for a scheduled appointment or a few days of home monitoring. Delaying care by even 24 to 48 hours when an active infection is present can allow bacteria to spread into deeper tissue or bone, a complication that requires far more aggressive treatment than a wound caught early. Trust your inspection routine and respond quickly when you see these specific signs:
- Any open wound that does not begin closing within 24 hours, regardless of how small it looks
- Redness spreading outward from a cut, blister, or sore, which indicates spreading infection
- Warmth or swelling in one area without an obvious cause like a recent injury
- Discharge, pus, or foul odor coming from any wound or from between your toes
- Skin that appears black, blue-gray, or dark brown, which can signal tissue death
- A fever over 100.4 degrees Fahrenheit combined with any foot symptom
- New or sudden increase in pain in a foot where you normally have reduced sensation
If you see black or blue-gray discoloration on any part of your foot, call your podiatrist immediately and do not wait to see if the color resolves on its own.
What to tell your podiatrist when you call
When you contact your care team, giving them specific, detailed information helps them determine how quickly you need to be seen and what to prepare for your visit. Vague descriptions slow the process and may result in a delayed appointment when you actually need urgent care.
Use this template when you call:
- When you first noticed it: date and time
- What it looks like: size, color, any discharge
- Whether it has changed: larger, redder, or more swollen since you first spotted it
- Your current symptoms: fever, pain level, whether you can bear weight
- Photo: mention that you have a photo on your phone to share at the visit
Your podiatrist uses this information to triage your situation accurately, so be as specific as you can rather than minimizing what you see.

Keep your feet healthy for the long run
Knowing how to care for diabetic feet comes down to daily consistency more than any single technique. The seven steps in this guide work together as a system: daily inspections catch problems early, proper hygiene and moisturizing protect your skin barrier, correct footwear reduces pressure, movement supports circulation, and prompt action when something looks wrong keeps small issues from becoming serious ones. None of these steps require expensive equipment or a lot of time, but all of them require you to show up for your feet every single day.
Your feet carry you through every part of your day, and protecting them is protecting your independence and quality of life. Build these habits into your routine the same way you manage your blood sugar or medication schedule. If you spot a warning sign or want a professional assessment of your foot health, the team at Achilles Foot and Ankle Center is ready to help. Book a same-day appointment and get the personalized care your feet deserve.






