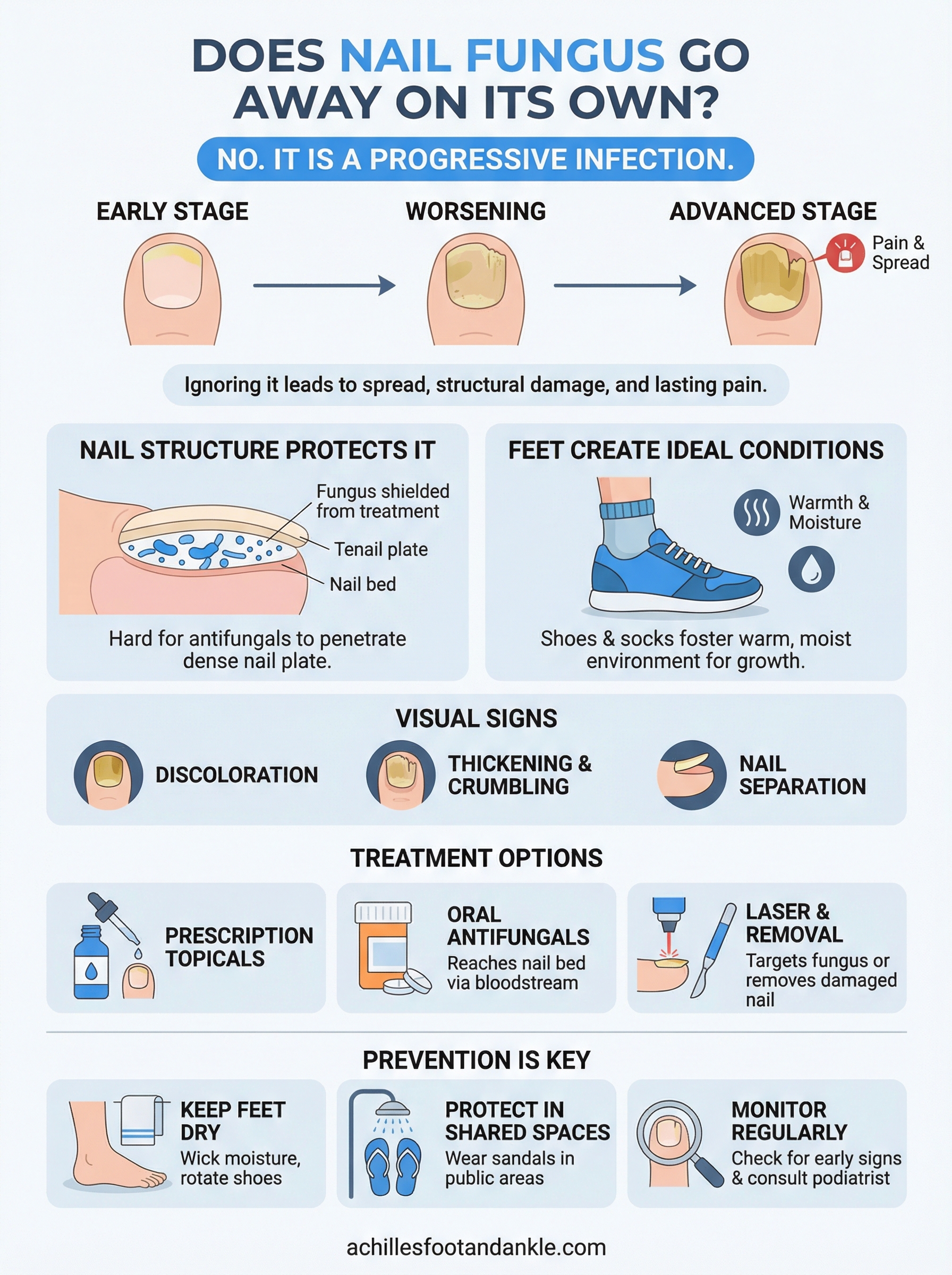
You noticed a yellowish discoloration under your toenail a few months ago. Maybe it’s thickened, started to crumble at the edges, or just looks off. You’re wondering: does nail fungus go away on its own? The short answer is no, and waiting it out typically makes things worse. Nail fungus is a progressive infection, meaning it spreads deeper into the nail and can jump to surrounding nails or skin the longer it goes untreated.
At Achilles Foot and Ankle Center, our podiatrists across Central Virginia treat nail fungus regularly, from mild early-stage cases to stubborn infections that patients have lived with for years. We see firsthand what happens when people assume it will resolve without intervention, and the outcomes are consistently better when treatment starts early.
This article breaks down exactly why nail fungus won’t clear up on its own, what risks come with ignoring it, and what treatment options actually work. Whether you’re dealing with a single affected nail or a recurring problem, you’ll leave with a clear understanding of your next steps.
Why nail fungus rarely clears on its own
If you’re wondering whether nail fungus goes away on its own, understanding how the infection works will answer that question quickly. Nail fungus is caused by dermatophytes, a group of fungi that feed on keratin, the protein that forms your nails. Once these organisms get beneath the nail plate, they settle into a protected, dark, and moist environment where your immune system has almost no direct access. This combination of structural protection and favorable conditions is what makes spontaneous resolution so rare.
The nail structure protects the infection
Your nail plate is dense by design, and that density works in the fungus’s favor. Antifungal agents, whether topical or oral, have difficulty penetrating the nail plate at concentrations strong enough to eliminate the infection entirely. The fungi live between the nail plate and nail bed, shielded from both treatment and your immune response. Each millimeter of nail tissue between the surface and the infection site reduces the effectiveness of surface-applied products significantly.
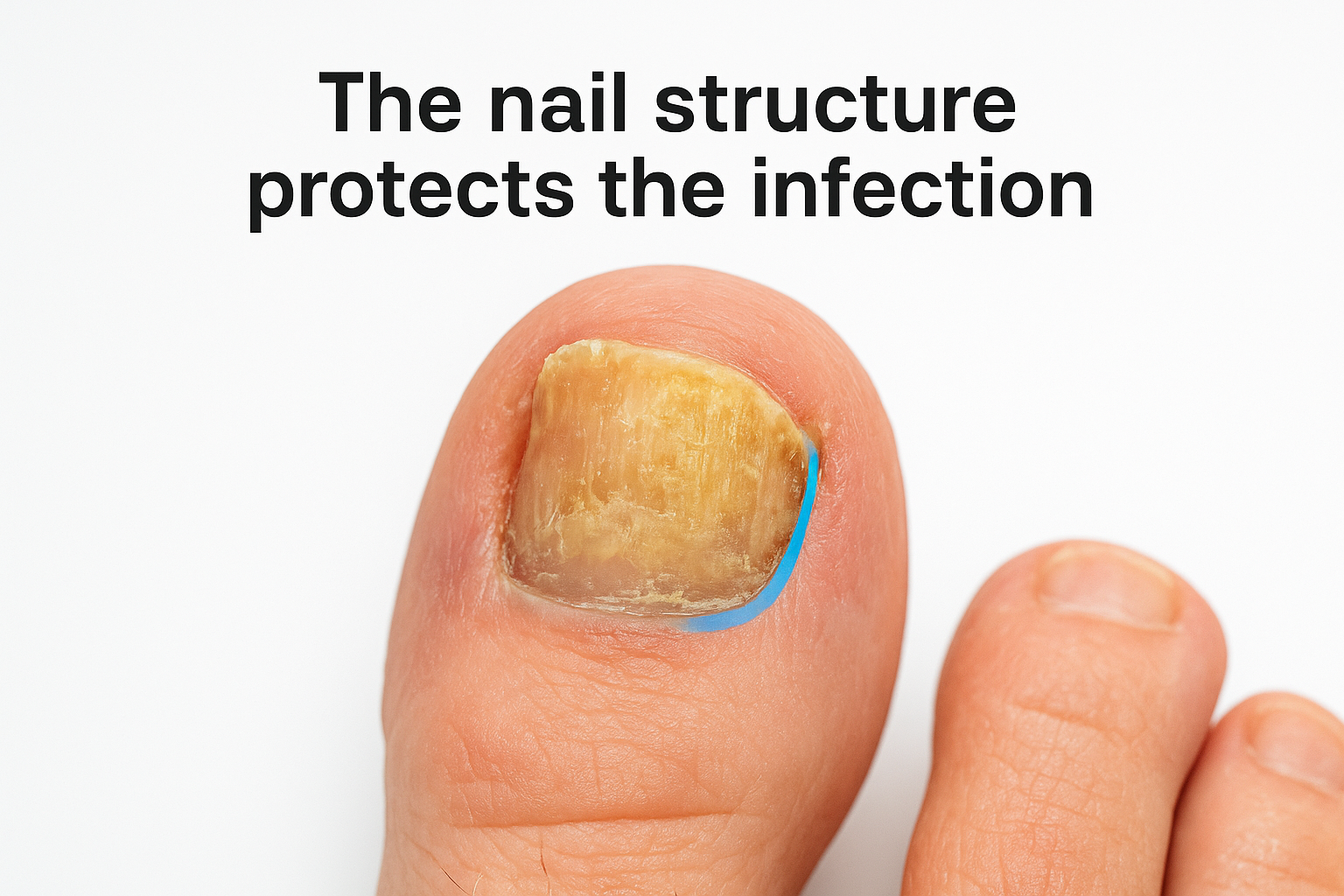
The fungus is not sitting on top of your nail; it is living inside and beneath it, which is why most over-the-counter topical treatments produce disappointing results.
Nails grow slowly, averaging about 3 millimeters per month for toenails. As the nail grows forward, infected tissue extends along with it. Without treatment, the infected portion keeps advancing further from the nail base, making it progressively harder to clear over time. This is one of the core reasons why anyone asking does nail fungus go away on its own tends to notice worsening rather than improvement after several months.
Your feet create conditions that support fungal growth
Shoes and socks create a warm, enclosed environment for most of the day, and sweat adds the moisture that dermatophytes need to survive and spread. This is not simply a hygiene issue; the physical conditions inside footwear are structurally favorable to fungal growth regardless of how clean your feet are. Factors that compound the problem include:
- Synthetic socks that trap moisture against the skin
- Tight-fitting shoes that limit airflow around the toes
- Shared shower floors, pool decks, and locker rooms
- Minor nail injuries that give fungi an entry point
- A weakened immune system or reduced circulation
What happens if you leave it untreated
Ignoring nail fungus does not freeze the infection in place. People who assume the question of does nail fungus go away on its own can wait for later typically find themselves dealing with more affected nails, thicker nail tissue, and increasing discomfort over time. The longer the infection persists, the harder it becomes to treat effectively and the more accumulated tissue damage you have to reverse.
The infection spreads to other nails and skin
Fungal spores shed continuously from an infected nail onto surrounding skin, adjacent nails, and surfaces you touch daily. Over time, you can develop tinea pedis (athlete’s foot) from the same dermatophytes spreading across the bottom and sides of your foot. What starts as one discolored toenail can become a multi-nail problem within a few months, and each additional nail adds time and complexity to treatment.
Common pathways through which the infection spreads include:
- Direct contact between infected and healthy toenails during grooming
- Walking barefoot on contaminated shower floors or pool decks
- Reusing socks and shoes that harbor fungal spores
- Transferring the infection to your fingernails when touching your feet
Treating a single nail early is significantly faster and less costly than managing a widespread infection across multiple nails and skin areas.
Structural damage and pain become lasting concerns
Nail tissue infected for years can become permanently thickened, distorted, and brittle, even after the fungus itself is cleared. In advanced cases, the nail separates from the nail bed in a process called onycholysis, which creates an opening for secondary bacterial infections to take hold.
Walking becomes painful as the thickened nail presses against the inside of your shoe with every step, and that altered gait can put additional stress on your ankles, knees, and hips over time.
How to tell if it is nail fungus
Before you can decide whether does nail fungus go away on its own is even the right question, you need to confirm you’re actually dealing with a fungal infection. Several other conditions affect nail appearance, so knowing the specific signs of fungal involvement helps you move toward the correct treatment rather than managing the wrong problem.
Visual signs to look for
Nail fungus produces a recognizable set of changes that develop gradually over weeks to months. A single sign in isolation can occasionally point to something else, but a cluster of the following changes is a strong indicator that fungi are involved:
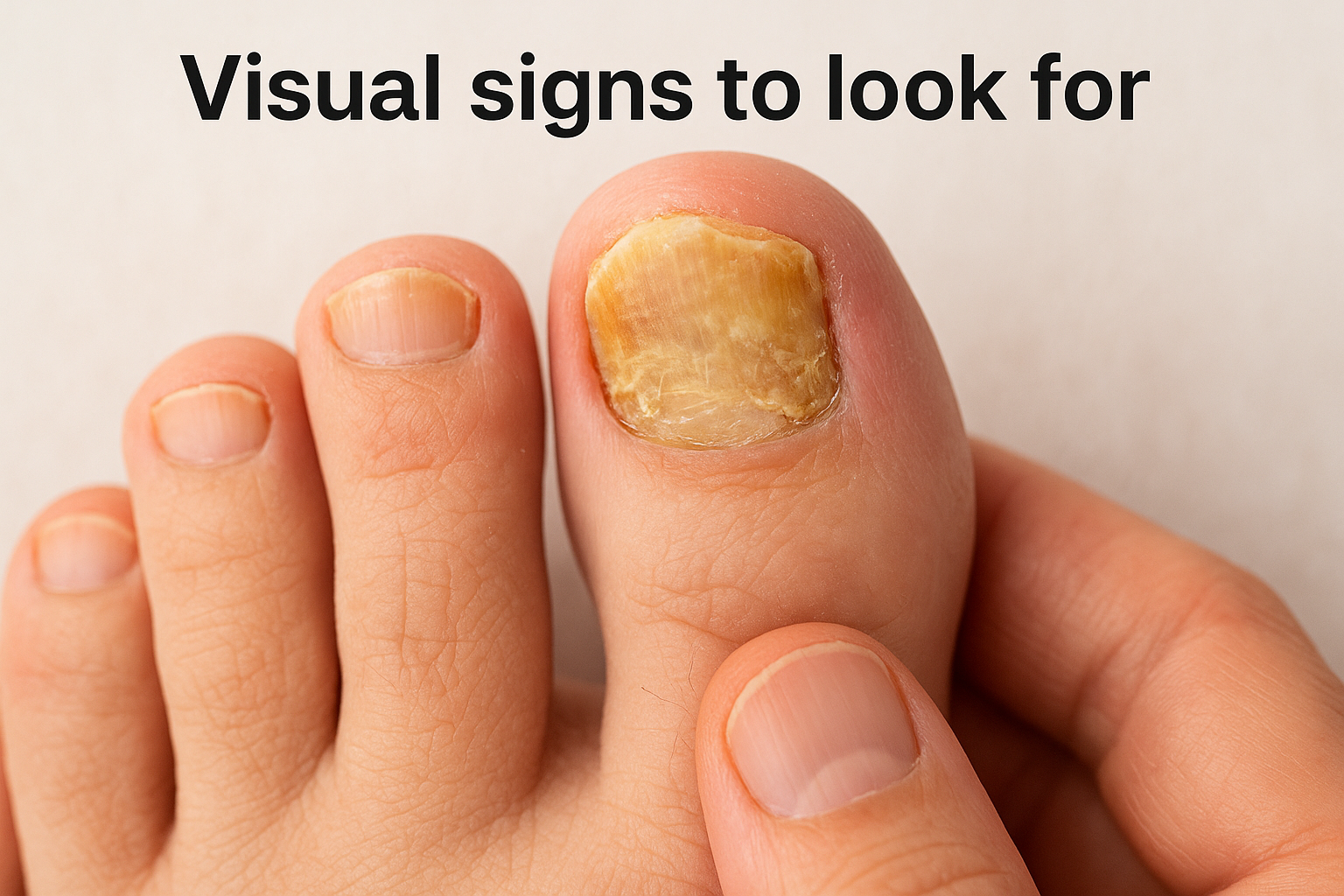
- Yellowish, brownish, or white discoloration starting at the nail tip or edges
- Thickened nail plate that becomes difficult to trim
- Brittle or crumbling texture, especially at the edges
- A nail that is pulling away from the nail bed underneath
- A mild odor coming from the affected nail
- Debris accumulating beneath the nail surface
The changes tend to worsen progressively rather than stay stable, and they almost never reverse without some form of treatment.
Conditions that can look similar
Nail psoriasis, nail trauma, and bacterial infections can all produce discoloration and thickness that resembles fungal infection at first glance. Nail psoriasis, for example, often causes pitting and oil-drop discoloration that looks remarkably similar to early fungal involvement.
Getting a confirmed diagnosis from a podiatrist before starting treatment matters, because applying antifungal products to a nail that is not actually infected delays the correct care.
A podiatrist can perform a nail culture or laboratory analysis on nail clippings to confirm the presence of dermatophytes, giving you a clear diagnosis to work from.
How nail fungus gets treated
Once you have a confirmed diagnosis, the treatment your podiatrist recommends will depend on how far the infection has progressed and how many nails are involved. Mild cases caught early respond better to a narrower treatment approach, while moderate to severe infections typically require a combination of methods to fully clear the fungus.
Prescription topical and oral antifungals
Prescription-strength topical antifungals differ from over-the-counter products in their ability to penetrate the nail plate more effectively. Options like efinaconazole and tavaborole are applied directly to the nail and have stronger evidence behind them than most store-bought alternatives. For more advanced infections, oral antifungals such as terbinafine or itraconazole are usually the first-line recommendation because they reach the nail bed through your bloodstream rather than relying on surface penetration.
Oral antifungal treatment typically runs for 12 weeks, but you may not see full results until a completely new, healthy nail grows in, which can take 9 to 12 months for toenails.
Laser treatment and nail removal
Laser therapy targets fungal cells beneath the nail plate using focused light energy, with minimal discomfort and no systemic side effects. Your podiatrist may recommend this option if you cannot tolerate oral medications or if previous treatments have not worked. In cases where the nail is severely damaged or a secondary bacterial infection has developed, partial or complete nail removal may be necessary to allow the nail bed to clear and a healthy nail to regrow.
Your podiatrist will evaluate all relevant factors before recommending a treatment plan, including your overall health, circulation, and the extent of the infection across affected nails.
How to prevent nail fungus from coming back
Clearing a fungal infection takes months, and the last thing you want after finishing treatment is to ask does nail fungus go away on its own all over again because it returned. Recurrence is common, especially if the conditions that allowed the original infection to develop remain unchanged. Prevention comes down to consistent habits rather than a single product or fix.
Keep your feet dry and protected
Moisture and warmth are the two conditions fungi need most to survive, so controlling them directly reduces your risk of reinfection. Swap synthetic socks for moisture-wicking materials like merino wool or treated cotton, and change them daily. Rotate your shoes to allow them to dry fully between uses, and consider using an antifungal powder or spray inside footwear that tends to hold moisture.
Protecting your feet in shared spaces matters just as much at home. Wear sandals or flip-flops on pool decks, gym showers, and locker room floors where dermatophytes live on surfaces and spread easily through direct contact.
Treating your shoes with an antifungal spray while you are treating your nails helps prevent reinfection from the same spores that may persist inside the footwear.
Monitor your nails regularly
Catching a new infection early is the single most effective way to avoid a repeat of a prolonged treatment cycle. Check your nails every few weeks for early signs like slight discoloration or any change in texture at the tip. If you notice anything developing, schedule an appointment with your podiatrist promptly rather than waiting to see if it progresses.
Next steps for healthy nails
Nail fungus does not go away on its own, and the longer you wait, the more work it takes to clear. Early treatment protects your nails from permanent structural damage and keeps the infection from spreading to surrounding nails and skin. If you have noticed discoloration, thickening, or crumbling at the nail edges, those signs are unlikely to reverse without professional care.
Your best next step is a confirmed diagnosis from a podiatrist who can assess how far the infection has progressed and recommend a treatment plan that fits your situation. Guessing at home wastes time and allows the fungus to establish itself more deeply. Whether you need a prescription topical, oral antifungal, or a more advanced approach, getting started promptly gives you the fastest path to healthy nails. Schedule a same-day appointment at Achilles Foot and Ankle Center and get an accurate diagnosis today.






