You went to bed feeling fine, then woke up at 2 a.m. with a toe so swollen and hot it hurts to let the bedsheet touch it. If that scenario sounds familiar, you’re not alone. Gout affects over 8 million adults in the United States, and the foot and big toe joint are among its favorite targets. Understanding what triggers gout flare-ups is the first step toward keeping them from derailing your life.
At Achilles Foot and Ankle Center, our podiatrists across Central Virginia diagnose and treat gout-related foot and ankle pain regularly, from acute flare-ups that need immediate relief to long-term plans that reduce how often attacks return. We see firsthand how specific habits, foods, and medical factors set the stage for a painful episode.
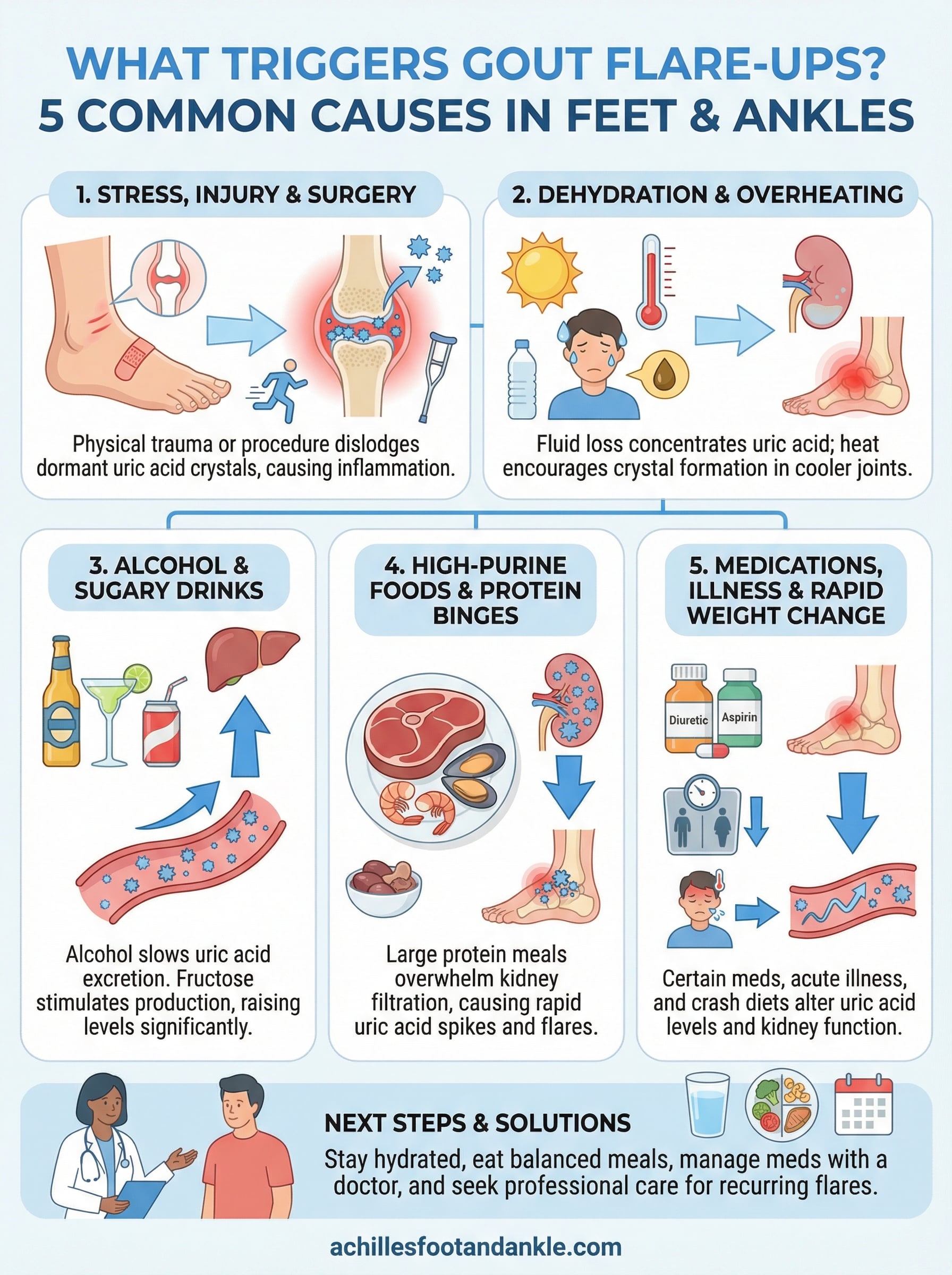
Below, we break down five common causes of gout flare-ups in the feet and ankles, explain why each one raises your uric acid levels, and share practical ways to avoid them. Whether you’re dealing with your first attack or your fifteenth, this guide will help you pinpoint your personal triggers and take control.
1. Foot and ankle stress, injury, or surgery
Physical trauma to the foot or ankle is one of the most underrecognized causes of gout attacks. When tissues around a joint take a hit, the body’s inflammatory response can dislodge uric acid crystals that were sitting dormant, sending your immune system into overdrive within hours.

Why it triggers a flare
Even minor trauma shifts the fluid balance and temperature inside a joint. Uric acid crystals are sensitive to those changes, and when disturbed, white blood cells rush in to attack them, producing the intense swelling and heat of a gout attack. Surgery amplifies this because anesthesia, blood loss, and post-op fluid changes all spike uric acid levels rapidly.
Physical trauma and surgery are two of the most reliable answers to what triggers gout flare-ups in people who already carry elevated uric acid levels.
Common foot and ankle scenarios that set it off
Several everyday situations can push your feet into flare territory:
- Long-distance running or hiking after a period of inactivity
- Spraining an ankle or stubbing your big toe
- Foot or ankle surgery, including bunion correction and tendon repair
- Wearing tight footwear for extended periods
How to reduce risk during activity and recovery
Ease back into exercise gradually to avoid rapid uric acid shifts. Stay hydrated before, during, and after activity, and choose well-fitting footwear to distribute pressure evenly across the foot. After any foot or ankle procedure, follow your recovery plan exactly and report unexpected swelling to your care team right away.
A few targeted habits help most:
- Drink water consistently throughout the day, not just during workouts
- Avoid jumping into intense training after a long break
- Keep every post-surgical follow-up appointment without skipping
When to see a foot and ankle specialist
A flare that starts within days of an injury or procedure warrants a podiatrist visit, not a wait-and-see approach. Getting proper diagnosis and treatment early limits pain duration and the longer-term joint damage that repeated attacks can cause.
Your podiatrist can also determine whether underlying uric acid levels need medical management, particularly if your activity level or surgical history makes you prone to repeat episodes.
2. Dehydration and overheating
Dehydration is one of the most overlooked answers to what triggers gout flare-ups, yet it happens in very common situations: hot weather, intense activity, illness, or simply not drinking enough throughout the day. When your body loses fluid faster than you replace it, uric acid concentrates in your bloodstream and the risk of crystal formation rises sharply.
Why it triggers a flare
Your kidneys need adequate fluid to flush uric acid efficiently. Without it, uric acid accumulates and settles into the cooler joints of your feet and ankles. Heat compounds this problem by driving fluid loss through sweat while lowering temperatures in peripheral joints, creating the exact conditions crystals need to form.
Consistent hydration is one of the simplest, lowest-cost tools for reducing gout attack frequency.
Signs your flare relates to fluid loss
A dehydration-linked attack often follows a recognizable pattern. You may notice dark urine or reduced urination in the hours before a flare begins. Attacks arriving after outdoor exertion in heat or during fever, vomiting, or diarrhea also point directly toward fluid loss as the trigger.
Practical hydration habits that help
Aim for at least eight cups of water daily, adjusting upward during exercise or hot weather. Spreading intake throughout the day works better than drinking large amounts at once. Water-rich foods like cucumber and watermelon can also contribute to your overall fluid balance.
When dehydration becomes urgent
Seek medical care if a gout flare arrives alongside extreme thirst, dizziness, or significantly reduced urination. These symptoms signal that your kidneys are under stress, and prolonged dehydration weakens your body’s ability to clear uric acid over time.
3. Alcohol and sugary drinks
What you drink affects uric acid levels more directly than many people expect. Both alcohol and fructose-heavy beverages drive those levels up through separate pathways, making them a dangerous combination for anyone prone to attacks.
Why it triggers a flare
Alcohol slows your kidneys’ ability to excrete uric acid, allowing it to accumulate in your bloodstream. Beer carries a double risk because it contains both alcohol and purines from brewer’s yeast.
Fructose, common in sodas and juice drinks, triggers a separate surge by stimulating uric acid production in the liver directly. This is one reason sugary beverages land on every list of what triggers gout flare-ups.
Even moderate, consistent drinking raises your baseline uric acid level over time.
Drinks most likely to cause problems
Certain beverages stand out as reliable flare triggers:
- Beer and spirits: strongest link to attack frequency
- Sugary sodas: high-fructose corn syrup elevates uric acid quickly
- Fruit juice: even natural varieties carry a significant fructose load
Smarter swaps that still feel realistic
Replacing high-risk drinks with water, black coffee, or low-fat milk can lower uric acid meaningfully over time. Black coffee in moderate amounts is associated with reduced gout frequency, making it a practical daily substitution.
When to talk to your clinician about patterns
If your flares reliably follow drinking episodes, bring that pattern to your clinician rather than guessing on your own. Tracking your intake before each attack gives your provider concrete data to inform both medication and dietary decisions.
4. High-purine foods and large protein binges
Your body breaks purines down into uric acid, so eating large amounts of high-purine foods floods your bloodstream faster than your kidneys can clear it. This spike is one of the most direct causes behind what triggers gout flare ups in the feet and ankles.
Why it triggers a flare
Purines occur naturally in many protein-rich foods. A large protein-heavy meal creates a rapid surge in uric acid production that overwhelms your kidney’s filtration capacity.
When that happens, uric acid crystals settle into the cooler, lower joints of your foot, where a painful flare follows quickly.
Food triggers people miss most often
Many people reduce red meat but overlook other major sources:

- Organ meats: liver, kidney, and sweetbreads carry the highest purine loads
- Shellfish: shrimp, scallops, and mussels are significant contributors
- Anchovies and sardines: small but densely packed with purines
How to eat for lower uric acid without extremes
Spreading moderate protein portions throughout the day keeps uric acid production steadier than one large meal. Low-fat dairy products are associated with lower uric acid, making them a practical substitute for higher-risk proteins.
Consistent, balanced eating controls uric acid more reliably than eliminating any single food group.
How to spot your personal food triggers
Keep a brief food log for two to three weeks, noting what you ate before each flare.
Bringing that record to your podiatrist gives them specific patterns to work with when adjusting your care plan.
5. Medications, illness, and fast weight changes
Some of the most surprising answers to what triggers gout flare ups involve factors your doctor controls, not your diet. Certain medications, acute illness, and rapid weight changes all shift uric acid levels in ways that can spark an attack with little warning.
Why it triggers a flare
Several medications raise uric acid directly or reduce your kidneys’ ability to clear it. Illness drives similar changes through dehydration, fever, and metabolic stress, concentrating uric acid quickly in peripheral joints like your feet and ankles.
Medications and health issues commonly involved
Your current medication regimen may be raising your uric acid without you realizing it. Common culprits include:
- Diuretics: frequently prescribed for blood pressure or heart failure
- Low-dose aspirin: can reduce uric acid excretion at certain doses
- Acute infections or fever: drive rapid fluid loss and uric acid spikes
Why crash diets and fasting backfire
Losing weight too fast is one of the most counterintuitive gout triggers people encounter.
Rapid weight loss floods your bloodstream with ketones and uric acid from breaking down tissue too quickly. Slow, steady progress through balanced, consistent eating protects your kidneys and keeps levels stable.
What to discuss with your prescribing doctor
Bring a complete list of current medications to your next appointment and ask whether any could be contributing to your flares. Your doctor can often adjust the dose or substitute an alternative that carries a lower gout risk.
Next steps if flares keep happening
Knowing what triggers gout flare-ups gives you a real advantage, but identifying triggers is only part of the equation. If attacks keep returning despite your best efforts to adjust diet, hydration, and activity, your uric acid levels may need medical management beyond lifestyle changes alone. Repeated flares cause progressive joint damage in the feet and ankles, and waiting too long to seek specialized care only makes that damage harder to reverse.
A podiatrist can run uric acid bloodwork, assess current joint damage, and build a treatment plan that fits your specific situation, whether that means prescription medication, custom orthotics, or a referral to a rheumatologist. At Achilles Foot and Ankle Center, our specialists across Central Virginia see gout patients regularly and can help you break the cycle for good. Book a same-day appointment and leave with a concrete plan before your next flare hits.






