Foot blisters are one of those injuries that seem minor, until they sideline you from your morning run or cut a hike short three miles in. Knowing how to prevent blisters on feet starts with understanding what causes them: friction, moisture, and heat working together against your skin. The good news is that most blisters are entirely avoidable with the right preparation.
At Achilles Foot and Ankle Center, our podiatrists treat blister-related complications regularly, from infections to ulcerations in patients with diabetes. We’ve seen firsthand how a little prevention goes a long way, especially for runners, hikers, and anyone breaking in new footwear. That clinical experience is exactly what shaped the advice in this article.
Below, you’ll find five practical tips to keep your feet blister-free, whether you’re logging miles on the trail or pounding pavement. We also cover what to do if a blister does form, so you can recover quickly and safely without making things worse.
1. Get a podiatry plan for repeat blisters
If you keep getting blisters in the same spots, that’s your body signaling a structural or mechanical problem that no amount of tape will permanently fix. A podiatrist can identify whether your gait, foot shape, or biomechanics are driving the repeated friction, then build a plan that actually addresses the root cause rather than just the symptom.
Why this prevents blisters
Recurring blisters in the same location almost always point to a repeating force pattern. A podiatrist can assess pressure distribution across your foot using gait analysis or pressure mapping tools, pinpointing exactly where and why your skin takes the most abuse. Addressing those underlying mechanical issues through custom orthotics, footwear recommendations, or targeted exercises stops blisters before they start rather than just treating them after the fact.
If you get blisters in the same spot on every run or hike, a single podiatry visit can save you months of repeated pain.
How to do it before your next run or hike
Book an appointment at least two to four weeks before a major event or trail season, so you have time to implement any recommendations. During the visit, bring the shoes you actually train in, not your newest pair, so the podiatrist can see real wear patterns. You should also mention any past foot conditions, like plantar fasciitis or bunions, because these often change how pressure distributes across your foot.
- Bring worn training shoes to the appointment
- Note which spots blister most often and how quickly they form
- Ask specifically about custom orthotics if over-the-counter insoles have not helped
Common mistakes to avoid
Many people visit a podiatrist only after a blister becomes infected or painful enough to stop activity. Waiting that long limits your options and extends recovery time significantly. Another common error is skipping follow-up appointments after getting custom orthotics fitted, since orthotics often need minor adjustments to work correctly for your specific movement patterns.
When to seek urgent care
You should seek same-day or urgent care if a blister shows signs of infection: increasing redness spreading beyond the blister, warmth, swelling, or pus. Patients with diabetes or poor circulation face a higher risk of serious complications from even minor blisters and should contact a podiatrist at the first sign of any skin breakdown on the foot.
2. Dial in shoe fit and break-in time
Ill-fitting shoes are the number one cause of preventable blisters, and buying the right size isn’t enough. Shoe volume, toe box width, and heel depth all affect how much your foot moves inside the shoe during any activity.

Why this prevents blisters
When your foot slides against the shoe’s interior, friction builds heat, and heat triggers a blister within minutes on a long run or hike. A properly fitted shoe with an adequate break-in period lets the materials conform to your foot shape, significantly reducing that internal movement.
Shop for shoes at the end of the day when your feet are at their largest, so you get a more accurate fit.
How to do it before your next run or hike
Give yourself at least two to three weeks to break in new footwear before any significant event. Your heel should feel snug but not compressed, and your toes need roughly a thumb’s width of space at the front.
- Start with short 20-minute sessions and build up gradually
- Wear new shoes around the house before taking them outdoors
- Check for pressure spots after each session
Common mistakes to avoid
Buying shoes that feel tight from day one is a common error. Leather and synthetic uppers both need time to soften, and skipping that break-in period causes friction spikes. Wearing brand-new shoes on a long trail is one of the fastest ways to learn how to prevent blisters on feet through painful experience.
When to seek urgent care
If new shoes cause immediate pain or numbness within the first 10 minutes, stop and remove them. Persistent soreness in one spot after breaking in shoes can signal a structural foot issue worth discussing with a podiatrist.
3. Use the right socks and manage moisture
Socks are your first line of defense between your foot and your shoe, yet most people treat them as an afterthought. Choosing the wrong material or thickness dramatically increases the moisture and friction that trigger blisters.
Why this prevents blisters
Wet skin blisters far faster than dry skin because moisture softens the outer layers, making them easier to shear. Technical running and hiking socks are engineered with moisture-wicking fibers that pull sweat away from the skin’s surface, keeping friction lower for much longer into your activity.
Switching from cotton to a moisture-wicking sock is one of the fastest, cheapest upgrades you can make to prevent blisters on feet.
How to do it before your next run or hike
Look for socks made from merino wool or synthetic blends like polyester or nylon, both of which manage moisture significantly better than cotton. Pair your socks with an antiperspirant foot spray applied the night before long efforts to further reduce sweat volume on the skin.
- Choose socks with reinforced heel and toe zones for high-friction areas
- Replace worn socks regularly since thinning fabric loses its cushioning and wicking ability
Common mistakes to avoid
Wearing double-layer socks incorrectly is a frequent problem. The inner layer needs to be thin and smooth against the skin. Thick, bunched seams near the toes cause localized friction spikes that create blisters faster than thin socks would.
When to seek urgent care
If excessive foot sweating persists despite moisture-wicking socks and antiperspirant products, a podiatrist can evaluate you for hyperhidrosis, a condition that significantly raises your blister risk and warrants targeted medical treatment.
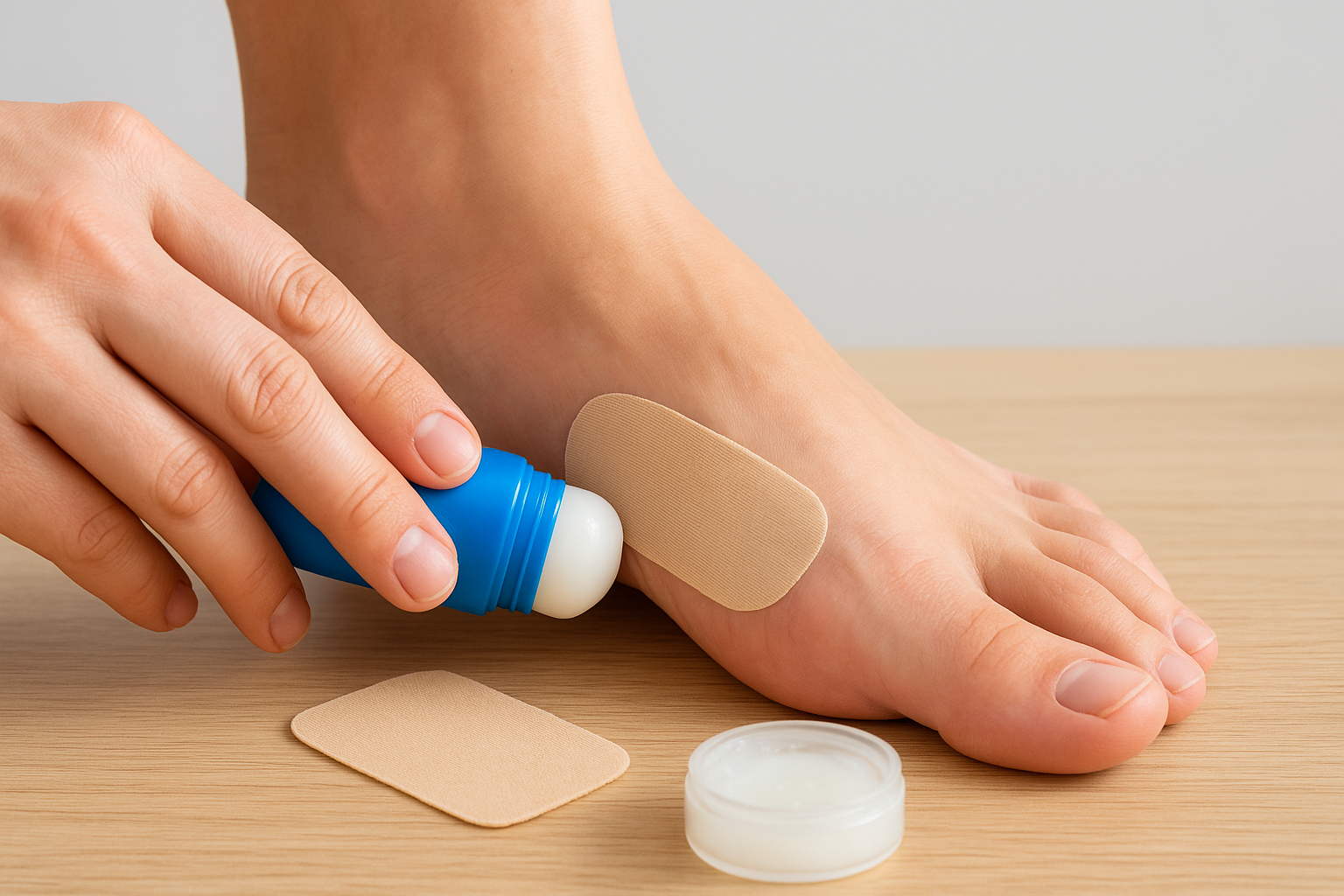
4. Reduce friction with tape, pads, and lube
Physical barriers and lubricants give your skin a direct layer of protection against the rubbing that causes blisters. When you know your high-risk spots, applying the right product before you start is one of the most reliable ways to understand how to prevent blisters on feet during long efforts.
Why this prevents blisters
Tape, gel pads, and lubricants all work by interrupting the friction cycle between your skin and your shoe. Lubricants reduce the shear force directly on the skin’s surface, while tape and pads create a physical buffer that absorbs the rubbing before it reaches your skin. Together, these tools give you meaningful protection even in shoes that still need more break-in time.
How to do it before your next run or hike
Apply your chosen barrier before you feel any discomfort, not after. Products like Body Glide, petroleum jelly, or anti-friction balms work well on heels, toes, and the ball of the foot.
- Use kinesiology tape or moleskin over known hot spots for multi-hour activities
- Apply lubricant to clean, dry skin so it bonds and stays in place throughout the activity
Applying tape and lube before you head out takes under two minutes and can save you from stopping mid-activity.
Common mistakes to avoid
Reapplying lubricant over already irritated or wet skin rarely works because the product won’t adhere properly. Many people also apply tape too loosely, which allows it to shift and create its own friction point.
When to seek urgent care
Seek care if tape or pad removal tears the skin beneath, especially if raw tissue is exposed. Patients with diabetes or neuropathy should not self-treat any skin damage and should contact a podiatrist promptly.
5. Treat hot spots fast and care for blisters safely
A hot spot is the burning sensation that warns you a blister is forming. Acting on that signal immediately is one of the most effective ways to understand how to prevent blisters on feet from becoming a real problem. Stopping to address it takes two minutes; ignoring it can cost you miles.
Why this prevents blisters
Hot spots become fluid-filled blisters within minutes if friction continues. Treating them at the first sign of irritation breaks that cycle before the skin layers actually separate. Early intervention keeps you moving and avoids the longer recovery that comes with a fully formed or popped blister.
Stop and address a hot spot the moment you feel it. The longer you wait, the worse the damage.
How to do it before your next run or hike
Carry a small blister kit in your pack or running vest with moleskin, a sterile needle, antiseptic wipes, and a bandage. If a blister forms, clean the area, drain it by puncturing the edge with a sterile needle, and cover it with a hydrocolloid bandage to protect the intact skin above it.
Common mistakes to avoid
Tearing off the blister roof is a common error that exposes raw tissue and significantly raises your infection risk. Do not use non-sterile tools to drain a blister.
When to seek urgent care
Contact a podiatrist if a blister shows red streaking, significant swelling, or discharge, as these indicate infection requiring prompt medical treatment.
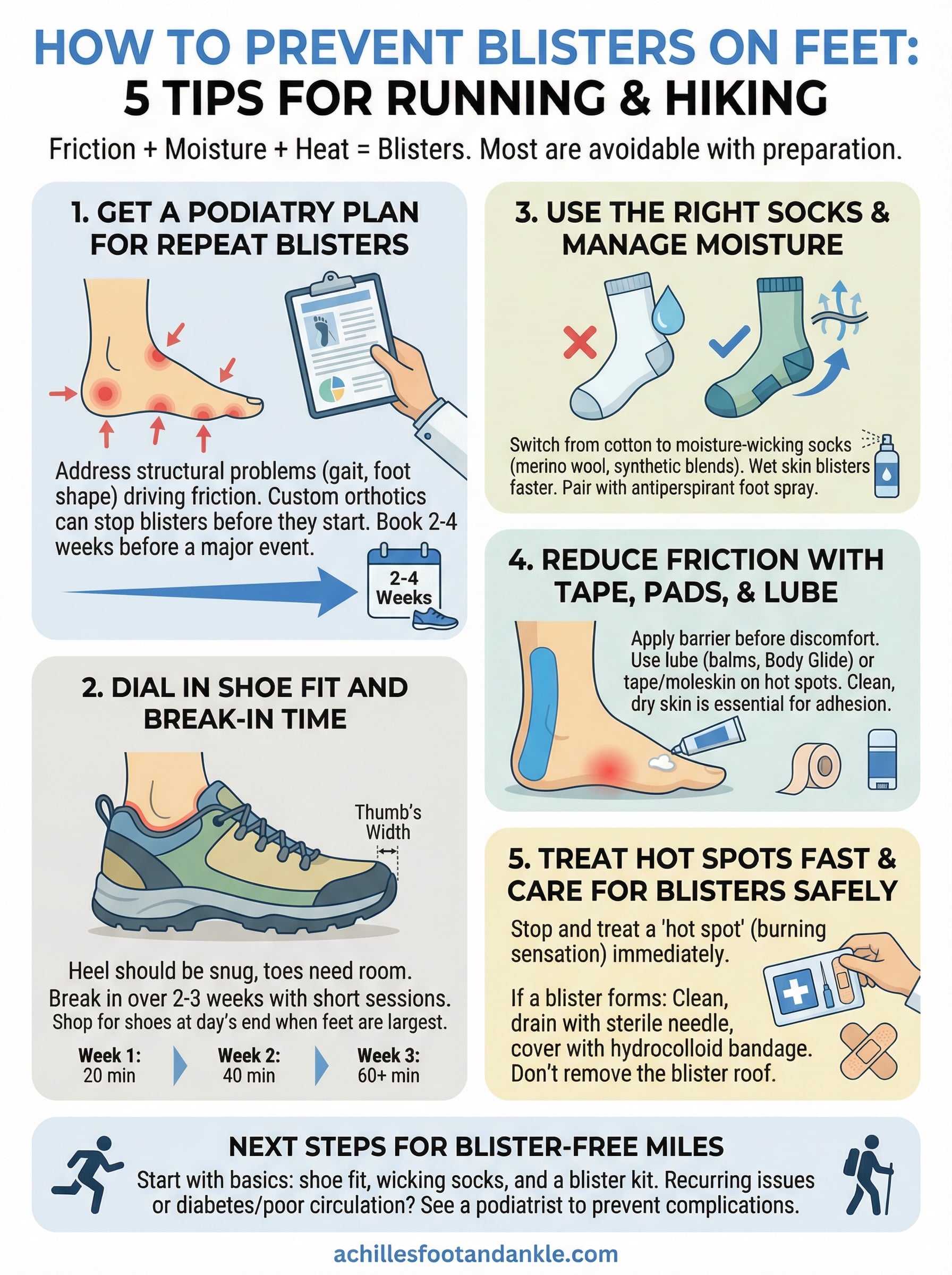
Next steps for blister-free miles
Knowing how to prevent blisters on feet is only useful if you put it into practice before your next run or hike. Start with the basics: check your shoe fit, swap to moisture-wicking socks, and carry a small blister kit on every outing. These three changes alone will reduce your blister risk significantly without adding much time or cost to your routine.
Persistent or recurring blisters deserve more than a bandage. If you keep getting them in the same spot, or if you have diabetes, poor circulation, or any condition that slows wound healing, a podiatrist can identify what’s driving the problem and build a prevention plan around your specific foot mechanics. Don’t wait for a blister to become infected before you seek help. Book a same-day appointment at Achilles Foot and Ankle Center and get your feet evaluated by a specialist who can keep you moving.






