If you’ve ever felt a sharp ache under the front of your foot mid-run, you’re not alone. Ball of foot pain running is one of the most common complaints we hear from runners at our Central Virginia clinics, from weekend joggers to competitive athletes. That pain can show up as a dull burn, a stabbing sensation, or the feeling of stepping on a pebble that isn’t there.
The causes range from simple overuse and poorly fitting shoes to conditions like metatarsalgia, sesamoiditis, or Morton’s neuroma. Some of these respond well to rest and a shoe change. Others need professional evaluation before they turn into something that keeps you off the road for months. Knowing the difference matters.
At Achilles Foot and Ankle Center, our podiatrists diagnose and treat these injuries every day using advanced imaging and hands-on assessment across thirteen locations in Central Virginia. This article breaks down why the ball of your foot hurts when you run, what the most likely diagnoses are, how to treat each one, and when it’s time to stop pushing through the pain.
Why ball of foot pain shows up in runners
Running puts enormous force on the forefoot with every stride. Each time your foot pushes off the ground, the metatarsal heads (the five bones at the front of your foot) absorb pressure that can reach two to three times your body weight. Do that thousands of times per mile, and it becomes clear why the ball of your foot takes a beating long before other parts of your body give out.
The forefoot takes more repetitive impact per run than almost any other structure in the lower extremity, which makes ball of foot pain running one of the most predictable injuries in the sport.
The mechanics behind the problem
Your foot has a natural fat pad underneath the metatarsal heads that cushions ground contact. Over time, that pad thins out, especially in older runners or those who log high weekly mileage. When the cushion shrinks, bone and nerve tissue bear more direct impact, and inflammation follows quickly. The forefoot also flexes sharply at toe-off, which stresses the small joints and soft tissues in that area repeatedly throughout a run.

Runners who strike further forward on the foot, whether by habit or by switching to minimal shoes, shift even more load onto the metatarsal heads. Tight calf muscles and a limited ankle range of motion force the forefoot to compensate during push-off, adding stress to an already loaded area.
How training habits make it worse
Sudden spikes in weekly mileage are one of the most common triggers. Your soft tissue needs time to adapt to new loads, and adding too many miles too fast does not give it that chance. Hill running and speed work increase forefoot pressure compared to flat easy running, so stacking those sessions without recovery amplifies the risk. Worn-out shoes that have lost their midsole cushioning contribute just as much as any training error.
What might cause your pain
Several conditions can produce ball of foot pain running, and each one has a slightly different feel. Pinpointing the right cause determines how you treat it and how quickly you recover.
The most common diagnoses
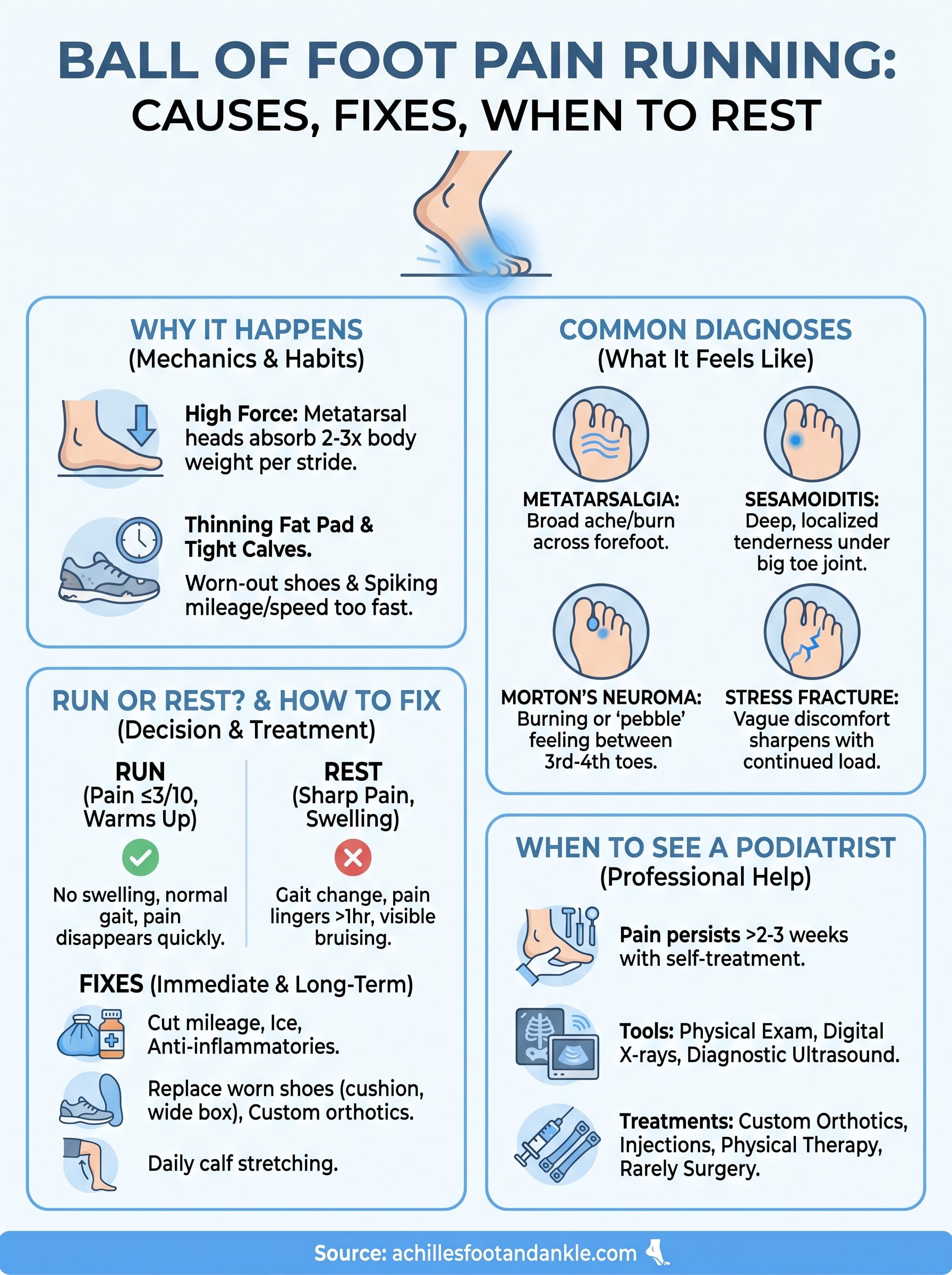
Metatarsalgia is an umbrella term for inflammation around the metatarsal heads. It typically feels like a broad ache or burning across the front of the foot rather than a sharp, pinpoint pain. Sesamoiditis targets the two small bones beneath your big toe joint and causes a deeper, more localized tenderness that gets worse when you push off the ground.

Morton’s neuroma produces a burning or electric sensation between the third and fourth toes, often described as walking on a folded sock.
Stress fractures in the metatarsals start as vague discomfort that sharpens with continued loading and can become serious if you ignore them. A plantar plate tear, which involves the ligament that holds your toe joints stable, causes swelling and a sense of instability at the ball of the foot. Each of these conditions requires a different approach, which is why an accurate diagnosis saves you weeks of mistreated pain.
How to decide if you should run or rest
Not every ache means you need to stop training, but running through the wrong kind of pain can turn a minor issue into a serious injury. The key is knowing the difference between soreness and a warning sign before you lace up.
Signs you can keep running
Your pain might be manageable if it rates a 3 or below on a 10-point scale and disappears within a few minutes of warming up. If your form stays normal and the discomfort does not get progressively worse as the run continues, a shorter, easier effort may be reasonable.
If your pain level rises during the run or lingers for more than an hour after you finish, that is your body asking you to stop.
Signs you need to stop
Ball of foot pain running that is sharp, sudden, or localized to one spot deserves immediate rest. Stop running if you notice visible swelling, bruising, or any change in how your toes align, as these point to structural damage that worsens under load. Pain that forces you to alter your gait is also a clear stop signal.
How to fix ball of foot pain from running
Most cases of ball of foot pain running respond well to a structured approach that addresses both the immediate inflammation and the underlying cause. Starting with the right interventions early gives you the best chance of returning to full training without a prolonged setback.
Reduce load and inflammation first
Your first priority is to cut back your mileage and remove any sessions that spike your pain. Ice the affected area for 15 minutes after activity to calm inflammation. Anti-inflammatory medication like ibuprofen can help in the short term, but treating only the symptom without fixing the cause will bring the pain right back once you resume normal training.
Reducing load does not mean stopping completely; it means training at an intensity that keeps pain below a 3 out of 10.
Address the mechanical causes
Replacing worn-out shoes is often the single highest-impact fix you can make. Look for a shoe with adequate forefoot cushioning and a wide toe box that does not compress the metatarsal heads. Custom orthotics redistribute pressure away from the irritated area and correct biomechanical patterns that contributed to the problem. Stretching your calves daily also reduces the forefoot load during push-off, which directly lessens stress on the structures causing your pain.
When to see a podiatrist and what to expect
Self-treatment works for mild cases, but persistent ball of foot pain running that does not improve within two to three weeks of rest and shoe changes needs professional evaluation. A podiatrist can identify structural problems that conservative measures cannot fix and prevent a minor issue from becoming a chronic injury that sidelines you for months.
Do not wait until you cannot walk without pain to make an appointment.
What a podiatrist will check
Your appointment will start with a physical examination of your foot, including an assessment of how you walk and where pressure concentrates during movement. Digital X-rays and diagnostic ultrasound can confirm stress fractures, sesamoid damage, or a plantar plate tear quickly and without guesswork.
From there, your treatment plan might include custom orthotics tailored to your foot structure, corticosteroid injections for targeted inflammation, or a referral for physical therapy to correct the mechanics driving your pain. In rare cases where conservative care fails, minimally invasive surgical procedures are available. At Achilles Foot and Ankle Center, same-day appointments are offered across thirteen Central Virginia locations, so you do not have to wait long to get clear answers and start recovering.
A simple plan to move forward
Ball of foot pain running does not have to end your season or your progress. The path forward is straightforward: reduce your load now, address the mechanical causes with better shoes or orthotics, and give your tissue time to recover before ramping mileage back up. Most runners who act early return to full training within a few weeks.
Track your pain level on every run. If it stays below a 3 and drops within an hour of finishing, you are likely managing things correctly. Sharp pain, swelling, or worsening discomfort at any point means you need to pull back and reassess. Give your body honest feedback and it will tell you when you are ready to push again.
If your pain persists beyond two to three weeks or you are not sure what is causing it, do not guess. Book a same-day appointment at Achilles Foot and Ankle Center and get a clear diagnosis so you can move forward with confidence.






