A patient’s experience starts long before a doctor walks into the exam room. It begins with the first phone call, the ease of scheduling, the greeting at the front desk, and the feeling that someone actually listens. Improving patient care experience isn’t just a buzzword for hospital administrators, it’s the difference between a clinic patients return to and one they warn others about.
At Achilles Foot and Ankle Center, we’ve spent years refining how we deliver care across thirteen locations in Central Virginia. From same-day appointments to our dedicated surgery center, every operational decision ties back to one question: does this make things better for the patient? That hands-on perspective shapes the practical advice in this article. We’ve seen what works, and what quietly drives patients away.
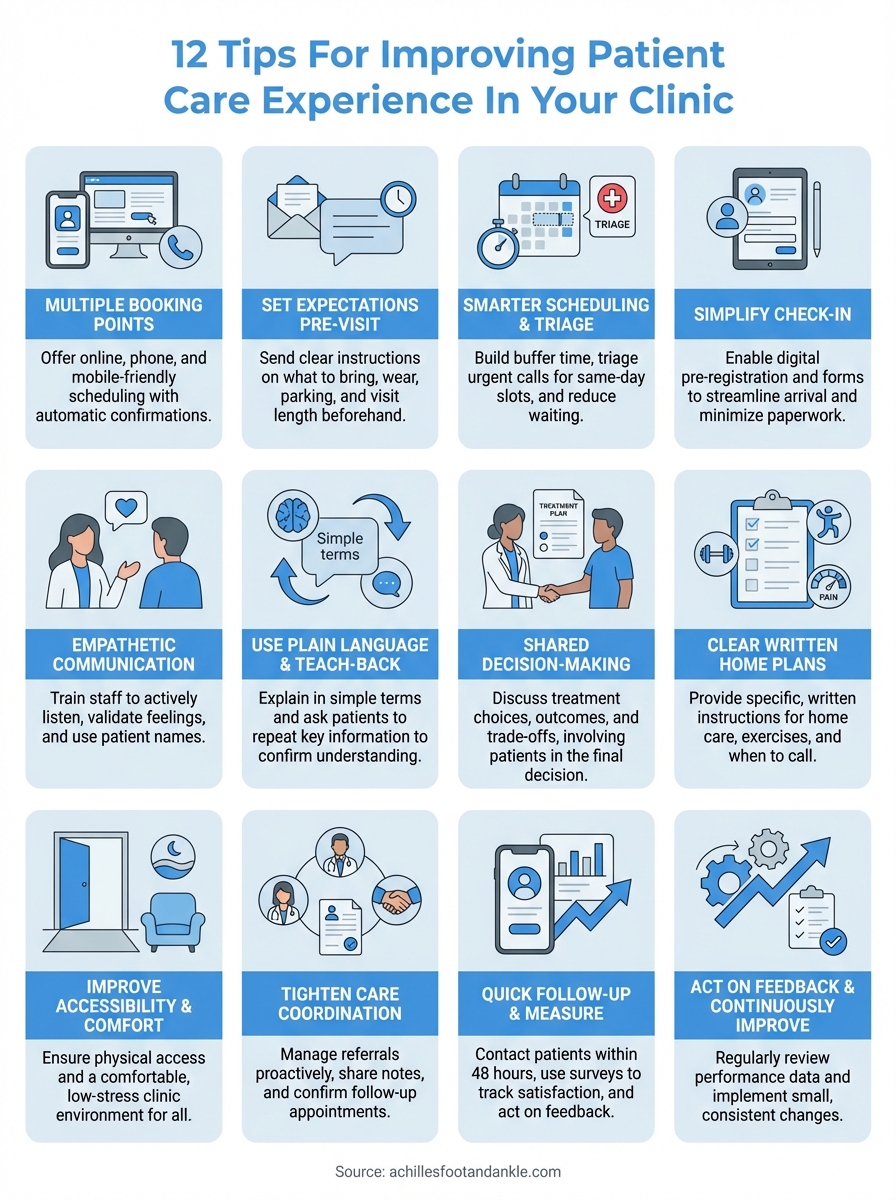
Below, you’ll find 12 actionable tips that any clinic can put into practice to strengthen patient satisfaction, build loyalty, and deliver care that people genuinely appreciate. Whether you run a solo practice or a multi-location operation, these strategies address real friction points, from communication gaps to follow-up failures, that shape how patients feel about the care they receive.
1. Make booking easy with multiple access points
Patients who struggle to book an appointment often don’t bother. They move on to a clinic that makes it simple. Friction at the booking stage is one of the most preventable reasons clinics lose new patients before care ever begins, and fixing it is one of the fastest wins available when you’re focused on improving patient care experience.

What great looks like
A clinic with excellent booking gives patients at least three ways to schedule: by phone, through an online portal, and via a mobile-friendly website request form. Great scheduling systems also confirm appointments automatically, send reminders, and allow patients to cancel or reschedule without calling during office hours. The goal is to remove every obstacle between a patient’s decision to seek care and their confirmed appointment slot.
When patients can book on their own terms, at any hour, show rates increase and no-shows decrease.
How to run it in a foot and ankle clinic
Foot and ankle patients often deal with pain or limited mobility, which makes navigating a complicated phone tree even more frustrating. Your clinic should offer online booking that captures the reason for the visit, insurance details, and any urgent symptoms upfront. This lets staff prepare before the patient walks in. Same-day appointment availability, like the option Achilles Foot and Ankle Center provides, should be clearly advertised so patients with acute injuries know they don’t have to wait or head to an emergency room.
Examples to copy in your next visit
Start by auditing your current booking flow as if you were a first-time patient. Call your own clinic line and time how long it takes to reach a human. Test your online portal on a phone to see whether the process takes under three minutes. If either experience frustrates you, it frustrates your patients. Add a direct booking link to your Google Business Profile so patients searching locally can schedule without visiting your website first.
How to measure and improve
Track two key numbers: the rate of incomplete online booking attempts (your portal analytics will show drop-off points) and your no-show rate by booking channel. If phone bookings produce more no-shows than online bookings, that tells you something about the patient commitment level at each touchpoint. Review these monthly, and adjust your reminder cadence or booking steps accordingly.
2. Set expectations before the patient arrives
When patients don’t know what to expect, anxiety fills the gap. Unclear instructions, surprise costs, and confusion about what to bring all create friction before the appointment even starts. Proactively communicating what will happen removes that friction and signals that your clinic respects the patient’s time, which is a direct part of improving patient care experience at every touchpoint.
What great looks like
A well-prepared patient arrives on time, knows exactly what to bring, and understands the rough shape of their visit. Great clinics send a pre-visit communication that covers parking details, check-in steps, what to wear, and any preparation the appointment requires, like removing nail polish before a foot exam. This one step alone reduces front-desk chaos and cuts late arrivals significantly.
Patients who feel informed before they arrive are less anxious and more engaged during the visit.
How to run it in a foot and ankle clinic
Foot and ankle appointments often involve specific physical requirements, such as removing shoes and socks or bringing prior imaging. Send an automated email or text 24 to 48 hours before the appointment that outlines exactly what to expect. Include your cancellation policy, estimated visit length, and a link to your patient portal for pre-registration so patients can complete forms from home.
Examples to copy in your next visit
Draft a short pre-visit message that covers four items: what to bring, what to wear, where to park, and how long the visit will take. Keep it under 150 words and test it with a staff member who hasn’t read it before to check for clarity.
How to measure and improve
Track late arrivals and missing document rates each month. If patients consistently show up unprepared, your pre-visit message isn’t working. Adjust the timing, channel, or wording and retest until the numbers shift.
3. Cut waiting with smarter scheduling and triage
Long waits erode trust faster than almost anything else in a clinical setting. Patients notice every extra minute they spend in a waiting room, and that frustration directly shapes how they feel about the care they received. Smarter scheduling and triage are two of the most direct levers for improving patient care experience without requiring major new technology or additional staff.
What great looks like
A well-run schedule builds buffer time between appointments to absorb overruns without pushing every subsequent patient back. Great clinics also triage incoming calls to separate urgent needs from routine visits, so acute cases get same-day slots and planned appointments stay on track.
When your schedule reflects realistic time blocks, both patients and staff stay calmer throughout the entire day.
How to run it in a foot and ankle clinic
Foot and ankle cases vary widely in complexity. Schedule appointment types in matched time blocks rather than applying one default duration to every visit. Use a brief intake question during booking to flag elevated pain levels or new injuries that need a longer or more urgent slot, keeping your day from running off-course before noon.
Examples to copy in your next visit
Review your last month of schedules and identify which appointment types consistently ran over time. Adjust those blocks by ten minutes and monitor whether delays shrink. Consider these additions:
- Post estimated wait times visibly in your waiting room
- Add a triage question to your booking form to catch urgent cases early
How to measure and improve
Track average wait time per appointment type and review it monthly. Set a clear target, such as under 15 minutes from check-in to provider entry, and address persistent outliers in your regular team huddles so delays don’t quietly become the norm.
4. Simplify check-in and paperwork
Check-in is the first in-person impression your clinic makes, and a slow or confusing process signals disorganization before the patient even sits down. Streamlining this step is a direct investment in improving patient care experience from the moment someone walks through your door.
What great looks like
A smooth check-in takes under three minutes and requires no duplicate data entry from the patient. Great clinics collect insurance details, health history, and consent forms digitally before the visit so staff can focus on greeting patients warmly rather than shuffling paperwork.
When check-in feels effortless, patients arrive in a calmer state and the clinical encounter starts on stronger footing.
How to run it in a foot and ankle clinic
Foot and ankle patients frequently arrive in pain or with limited mobility, making a lengthy paper process particularly frustrating. Connect your online patient portal directly to your intake workflow so that forms completed at home populate your system automatically. Reserve paper forms only as a backup for patients who genuinely can’t complete intake online.
Examples to copy in your next visit
Audit your current check-in flow by timing it during a busy morning. Look for these common sources of delay:
- Patients re-entering information they already submitted online
- Staff hunting for printed forms during peak hours
- Insurance verification happening at the desk instead of in advance
How to measure and improve
Track average check-in time weekly by logging timestamps from arrival to exam room entry. Set a target of under five minutes and review any visit that exceeds it to find the specific bottleneck causing the delay.
5. Train your team to communicate with empathy
Every staff member who interacts with a patient, from the front desk to the clinical assistant, shapes the overall experience. Empathetic communication is not a soft skill you either have or don’t; it’s a trainable behavior that directly affects patient satisfaction and whether people return. Building this skill into your team is one of the most cost-effective steps toward improving patient care experience across your entire operation.

What great looks like
A clinic with a strong communication culture makes patients feel heard and respected at every single touchpoint. Staff acknowledge wait times, explain delays without being asked, and use a patient’s name throughout the visit. Active listening means facing the patient, not the computer screen, and asking follow-up questions before moving to solutions.
Patients who feel genuinely heard are far more likely to follow their treatment plans and return for follow-up care.
How to run it in a foot and ankle clinic
Foot and ankle patients often arrive with chronic pain or post-injury anxiety, which raises the emotional stakes considerably. Train your team to acknowledge the discomfort before moving into clinical questions. A simple phrase like "I know this has been affecting your daily routine" costs nothing and resets the tone of the entire encounter.
Examples to copy in your next visit
Run a 15-minute role-play exercise in your next team huddle using these common scenarios:
- A patient frustrated by an unexpected wait
- A patient nervous about a surgical recommendation
- A first-time patient unsure about their diagnosis or next steps
How to measure and improve
Review patient satisfaction comments monthly and flag any feedback that mentions feeling rushed, dismissed, or confused. Tie those patterns back to specific interaction points and use them directly in your next team training session.
6. Use plain language and teach-back every time
Medical jargon creates real distance between you and your patients. When someone leaves confused about their diagnosis or treatment plan, adherence drops and outcomes suffer. Making plain language and teach-back a standard part of every visit is a practical, proven step toward improving patient care experience that costs nothing and takes only seconds to implement.
What great looks like
A clinician using plain language replaces terms like "plantar fasciitis" with "inflammation along the bottom of your foot" and follows every explanation with a teach-back prompt. That prompt asks the patient to repeat the key information in their own words so you can confirm they understood it, not test them. Teach-back is a two-way check, not a quiz.
Patients who can explain their diagnosis in their own words are far more likely to follow their treatment plan and return for follow-up care.
How to run it in a foot and ankle clinic
Foot and ankle conditions carry dense clinical vocabulary that patients rarely encounter outside your office. Build a short reference list of your ten most common diagnoses with plain-language equivalents and share it with every staff member who explains conditions or treatment steps to patients.
Examples to copy in your next visit
End every clinical explanation with one of these teach-back prompts:
- "What will you do when you get home today?"
- "How would you explain this condition to someone in your household?"
- "What questions do you still have about your next steps?"
How to measure and improve
Track patient-reported clarity scores through your post-visit surveys. If patients rate explanations low, audit your most common scripts and rewrite them using plain language before your next team review.
7. Practice shared decision-making for treatment plans
Patients who feel like passive recipients of a treatment plan are less likely to follow through on it. Shared decision-making means you actively involve the patient in choosing their care path, presenting options with honest trade-offs rather than handing down a single recommendation. This approach is central to improving patient care experience because it builds trust and strengthens the commitment patients bring to their recovery.
What great looks like
A clinician practicing shared decision-making explains two or more treatment options, outlines the realistic outcomes of each, and then asks the patient what matters most to them before moving forward. Great clinics document the patient’s stated preferences in the chart so the entire care team stays aligned with what the patient actually chose and why.
Patients who participate in their own treatment decisions report higher satisfaction and show better long-term adherence to their care plans.
How to run it in a foot and ankle clinic
Foot and ankle care often involves a genuine choice between conservative management and surgical intervention, and patients deserve to understand both paths clearly. Present each option with three pieces of information: what it involves, how long recovery typically takes, and what happens if the patient does nothing. This structure makes complex decisions manageable without overwhelming the patient.
Examples to copy in your next visit
Use this prompt to open the conversation: "There are two solid directions we can take here, and I want to walk you through both before we decide together." Then pause and let the patient ask questions before you offer a recommendation.
How to measure and improve
Add a single survey question asking whether the patient felt involved in their treatment decision. Review low scores monthly and bring specific visit patterns back to the team to adjust how options are presented.
8. Build a pain and mobility plan patients can follow
A treatment plan that lives only in a clinician’s notes does nothing for the patient once they leave. Clear, written pain and mobility guidance gives patients something concrete to act on at home, which is a fundamental part of improving patient care experience and improving actual outcomes at the same time.
What great looks like
A strong home plan is specific, not generic. It names the exact exercises, the frequency, the pain thresholds that should prompt the patient to stop, and a clear timeline for when they should expect to see progress. Great clinics present this plan in writing and walk through it verbally before the patient leaves the room.
Patients who leave with a written plan they understand are significantly more likely to complete their prescribed home care.
How to run it in a foot and ankle clinic
Foot and ankle recovery often requires daily mobility work and load management, and patients can’t do either correctly without specific instruction. Build a small library of condition-specific handouts for your most common cases, including plantar fasciitis, post-surgical rehab, and ankle sprain recovery, so staff can hand them out consistently without recreating instructions each visit.
Examples to copy in your next visit
Before the patient stands to leave, review the plan together and confirm they can answer two questions: what they will do today and what symptom would tell them to call your office. If they can’t answer both, the plan needs more clarification before they walk out.
How to measure and improve
Track return visit complaints about pain not improving as expected. If patients consistently report confusion about their home instructions, revise your handouts and retest comprehension using a teach-back prompt at the next round of appointments.
9. Improve accessibility and comfort in your clinic
Your physical environment sends a message before anyone on your team says a word. A clinic that is difficult to navigate or physically uncomfortable communicates carelessness, and that perception sticks with patients long after their appointment ends. Making your space genuinely accessible and welcoming is a practical, visible investment in improving patient care experience.

What great looks like
A well-designed clinic removes physical barriers and reduces sensory discomfort at every turn. Great clinics offer wide doorways and clear pathways for patients using mobility aids, provide seating at multiple heights, and keep noise levels low. Lighting, temperature, and cleanliness all contribute to whether a patient feels safe and respected inside your space.
Small environmental details, like the firmness of a waiting room chair, shape patient comfort more than most clinics realize.
How to run it in a foot and ankle clinic
Foot and ankle patients frequently arrive with significant mobility limitations, whether from a recent injury, post-surgical recovery, or chronic conditions like peripheral neuropathy. Your clinic layout should allow them to move from the entrance to the exam room without unnecessary steps, uneven surfaces, or narrow corridors that add pain to an already difficult visit.
Examples to copy in your next visit
Walk through your clinic as if you were a patient using crutches. Note every point where navigation becomes difficult or where seating is inadequate. Address the highest-friction items first.
How to measure and improve
Review patient feedback comments for any mention of physical discomfort or difficulty navigating your space. Assign one staff member to do a quarterly accessibility walkthrough and log findings for your next facilities review.
10. Tighten care coordination and referrals
Gaps between providers are where patients fall through. When referrals get lost, test results sit unreported, or patients are left to navigate specialist handoffs on their own, trust erodes and outcomes suffer. Strengthening care coordination is a direct path to improving patient care experience across every stage of a patient’s care journey.
What great looks like
A well-coordinated clinic treats referrals as a shared responsibility rather than a transaction. Great practices send the receiving provider complete clinical notes, confirm the patient has scheduled their follow-up appointment, and close the loop internally once the referral is complete.
When patients feel guided through transitions rather than abandoned at them, they trust your clinic far more.
How to run it in a foot and ankle clinic
Foot and ankle care regularly intersects with vascular specialists, physical therapists, and primary care physicians, so your coordination workflows need to be airtight. Assign one staff member to own referral follow-through, from sending the initial documentation to confirming the patient’s appointment within a defined window, such as five business days.
Examples to copy in your next visit
Review your last 20 referrals and check how many were confirmed as completed. If more than a quarter show no documented follow-through, that gap needs a defined workflow immediately. A simple shared tracking sheet with referral date, receiving provider, and confirmation status is enough to start closing that hole.
How to measure and improve
Track your referral completion rate monthly by logging the percentage of referrals with a confirmed patient appointment. Set a target above 90 percent and review any gaps in your weekly staff huddle to identify exactly where handoffs are breaking down.
11. Follow up quickly and measure experience
Most clinics collect feedback passively, if at all, and then wonder why patient satisfaction scores stay flat. Following up promptly after a visit and systematically measuring what patients actually experienced are two of the fastest ways to identify gaps in care before they become patterns. This step closes the loop on everything else discussed in this guide and gives you real data to drive improving patient care experience forward.
What great looks like
A clinic with a strong follow-up system contacts the patient within 24 to 48 hours after their appointment, either through an automated survey or a personal call for complex cases. Great clinics track responses over time, spot trends by appointment type or provider, and act on feedback within a defined review cycle rather than letting it sit in a dashboard.
Patients who receive a follow-up message after their visit report feeling more valued, even when their experience was only average.
How to run it in a foot and ankle clinic
Foot and ankle patients recovering from procedures or managing chronic conditions like peripheral neuropathy benefit from a direct check-in call within two days. Send a short satisfaction survey to every other patient through your patient portal or SMS system to capture experience data at scale without overwhelming your staff.
Examples to copy in your next visit
Use a three-question post-visit survey: Was your pain addressed clearly? Did you leave knowing your next step? Would you return to this clinic? Keep it short so completion rates stay high.
How to measure and improve
Review survey results monthly, broken down by provider and visit type. Flag any score below your target threshold and bring those specific cases into your next team huddle to identify the exact point where the experience broke down.
Simple next steps for your clinic
Improving patient care experience doesn’t require a complete overhaul of how your clinic operates. Start with the two or three tips in this guide that address your biggest current friction points, whether that’s a clunky booking flow, inconsistent follow-up, or communication gaps between your team and your patients. Small, consistent changes compound over time into a noticeably better experience for everyone who walks through your door.
Pick one tip this week and run it as a test. Measure the result, adjust based on what you find, and then move to the next item on the list. Your patients notice every improvement you make, even the ones that seem minor from the inside. If your clinic is in Central Virginia and you need foot and ankle care that already puts these principles into practice, book a same-day appointment and see the difference firsthand.






