You’re mid-run or halfway through a workout class, and a sharp ache spreads across the bottom of your foot. Arch pain during exercise is one of the most common complaints we hear from patients at Achilles Foot and Ankle Center, and it’s one that too many people try to push through. That decision often makes the underlying problem worse.
The causes range from overuse and flat feet to conditions like plantar fasciitis, and the right response depends entirely on what’s actually going on in your foot. Some cases respond well to simple changes in footwear or stretching, while others signal something that needs professional evaluation before it progresses.
This article breaks down why your arch hurts during physical activity, what you can do at home to find relief, and which warning signs mean it’s time to stop Googling and see a specialist. Our podiatry team treats these conditions daily across our Central Virginia locations, and we’ve built this guide around what we see in practice, not generic advice.
Why arch pain shows up during exercise
Your foot arch isn’t a static structure. It functions like a spring under load, absorbing ground impact with every step, jump, or lateral cut. When you exercise, that load increases dramatically compared to normal walking, which explains why arch pain during exercise often appears in people who had no symptoms at rest. Understanding what’s actually happening inside your foot makes the difference between choosing the right fix and making things worse.
What happens to your arch when you move
The arch is supported by a network of bones, tendons, and ligaments, with the plantar fascia serving as the main tension cable along the bottom of your foot. During physical activity, the plantar fascia stretches and recoils with each stride. When the demand on that structure exceeds its capacity, small tears and inflammation develop, and pain follows.
Repetitive impact activities like running, jumping, or court sports are particularly hard on the arch because they compress and stretch the plantar fascia at high frequency. Even low-impact workouts can cause problems if your foot mechanics are off, your footwear is worn out, or you’ve increased your training volume too quickly. Your foot structure, your training surface, and your shoes all influence how much stress lands on that tissue.
Why exercise intensity matters
Most patients who come into our clinic with arch pain describe a gradual onset, not a single injury. The tissue breaks down slowly through accumulated stress. Your body can handle a certain amount of load, but once you cross that threshold, inflammation sets in faster than your tissues can recover. Pain during a workout is your body telling you that the current demand exceeds what the tissue can tolerate.
The force your arch handles during a run can reach two to three times your body weight, which means even small mechanical problems get amplified quickly.
Training errors are one of the most preventable contributing factors. Jumping from light activity to high mileage, skipping rest days, or returning to sport too soon after a break all place sudden mechanical stress on tissues that haven’t had time to adapt. Understanding this load-response relationship is the first step toward addressing the root cause rather than just managing symptoms in the short term.
Common causes of arch pain
Several distinct conditions can produce arch pain during exercise, and identifying the right one matters because each has a different treatment path. A problem that looks like simple soreness on the surface often has a specific structural or mechanical cause driving it.
Plantar fasciitis
Plantar fasciitis is the most common cause of arch and heel pain in active people. The plantar fascia, a thick band of connective tissue running along your arch, becomes inflamed and microtorn when it’s repeatedly overloaded. You’ll typically feel the sharpest pain during the first few steps after rest and again when your workout intensity picks up. The condition tends to worsen progressively if you keep training through it without making any changes.
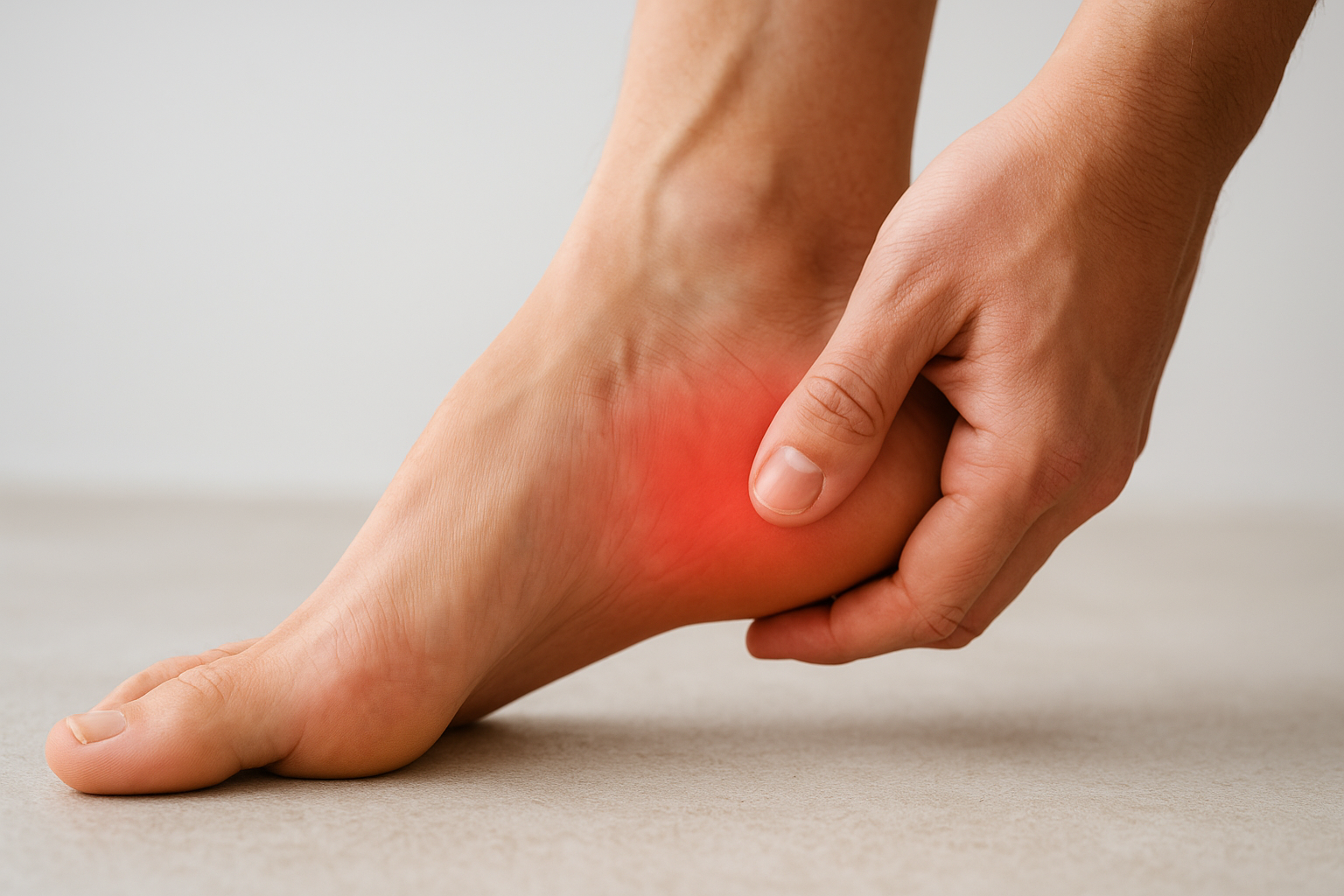
Plantar fasciitis accounts for roughly one million patient visits per year in the United States, making it one of the most frequently treated foot conditions in clinical practice.
Other conditions that contribute
Not every case of arch pain traces back to the plantar fascia. Flat feet (overpronation) force your arch to collapse inward under load, which strains muscles, tendons, and ligaments that aren’t built to absorb force at that angle. Posterior tibial tendon dysfunction is another common culprit, particularly in patients whose arch has progressively flattened over time. Stress fractures in the metatarsals or navicular bone can also mimic arch pain and often go undiagnosed because the pain feels diffuse rather than localized to one spot. If your symptoms don’t improve with basic rest and footwear changes, a podiatrist can use imaging and a physical exam to pinpoint which structure is actually involved.
Relief tips you can try today
Several practical steps can reduce arch pain during exercise without requiring a clinic visit right away. These aren’t permanent fixes for every condition, but they give your tissue a chance to calm down while you figure out the next step. Start with the simplest interventions first before adding layers of treatment.
Stretch and release the plantar fascia
The plantar fascia tightens during periods of rest and gets pulled hard when you start moving again. Loosening it before activity reduces the stress on that tissue from the first step. Each morning before you stand up, pull your toes back toward your shin and hold for 30 seconds, repeating three times. This pre-loads the fascia in a controlled way rather than letting your full body weight do it abruptly.

Rolling a frozen water bottle or a firm massage ball under your foot for two to three minutes after a workout helps reduce local inflammation and keeps the tissue pliable between sessions.
A calf stretch against a wall is equally important because a tight Achilles tendon pulls on the heel bone and increases tension throughout the plantar fascia. Hold each stretch for at least 30 seconds on both sides.
Adjust your footwear and support
Worn-out shoes are one of the most common and overlooked contributors to arch pain. Running shoes lose significant cushioning well before the upper shows visible wear, so replace them based on mileage rather than appearance. Adding over-the-counter arch support insoles to your current shoes can provide immediate relief by distributing load more evenly across your foot during activity.
Prevent arch pain and return to training
Preventing arch pain during exercise comes down to managing how much stress you put on your foot relative to what it can currently handle. Most arch injuries are not random, they follow a predictable pattern of load exceeding tissue capacity, often because training volume increased too quickly or recovery time got cut short. Addressing both factors keeps you moving without interruption.
Build load gradually
Your connective tissue adapts more slowly than your cardiovascular system, which means your lungs and legs may feel ready for more before your plantar fascia is. A 10 percent weekly increase in mileage or intensity is a widely used guideline in sports medicine because it gives tendons and ligaments time to remodel and strengthen. Skipping rest days or jumping back into full training after a break is where most patients create the conditions for their next injury.
Scheduling at least one full rest day per week and rotating between high-impact and low-impact sessions reduces cumulative stress on your arch significantly.
Strengthen the muscles that support your arch
Your arch does not work in isolation. The intrinsic foot muscles and calf complex share the load with the plantar fascia, and when those muscles are weak, the fascia absorbs a disproportionate share of the stress. Single-leg calf raises, short-foot exercises (where you scrunch your toes to shorten the arch without curling them), and towel-scrunching drills all build the muscular foundation that protects your arch over time. Doing these three to four times per week takes less than ten minutes and pays off in reduced injury risk.
Red flags and when to see a podiatrist
Not every case of arch pain during exercise needs a clinical evaluation, but some cases clearly do. The challenge is knowing which category your situation falls into. Mild soreness that fades with rest and responds to the relief tips above is usually manageable on your own, at least initially. Symptoms that persist, intensify, or change character are telling you something different.
Signs that go beyond normal soreness
Pain that does not improve after two to three weeks of rest, stretching, and footwear adjustments is a clear signal to stop self-treating and get a proper assessment. Other red flags include swelling or bruising across the arch, sharp localized pain that gets worse with each workout rather than better, numbness or tingling in the foot, or pain that wakes you up at night. These symptoms point to conditions like stress fractures, nerve compression, or tendon damage that home care cannot resolve.
If you cannot complete a normal walk without significant pain, do not wait weeks to see someone.
What a podiatrist can do that rest alone cannot
A podiatrist brings diagnostic tools and clinical experience that no amount of self-treatment can replace. Through physical examination, gait analysis, and imaging when needed, they identify the exact structure involved and rule out more serious causes. Getting the right diagnosis early shortens your recovery and prevents a minor problem from becoming a chronic one. Depending on your diagnosis, treatment options can include:
- Custom orthotics built to your specific foot mechanics
- Corticosteroid injections to reduce persistent inflammation
- Physical therapy targeting the weak structures contributing to your pain
- Minimally invasive or surgical intervention for structural problems that conservative care cannot fix
A simple path forward
Arch pain during exercise rarely resolves on its own when you keep ignoring it. The good news is that most causes respond well once you address the right contributing factor, whether that’s your footwear, your training load, or a specific structural issue that needs professional attention. Starting with the basics, stretching, better shoes, and smarter training progression, handles a large percentage of cases before they ever need clinical care.
When those basics aren’t enough, acting quickly matters. A podiatrist can identify exactly what’s happening inside your foot, rule out conditions like stress fractures or tendon damage, and give you a treatment plan built around your specific mechanics rather than generic advice. The longer you wait on a problem that isn’t improving, the harder and longer the recovery typically becomes.
If your arch pain has lasted more than a few weeks or is keeping you out of training, schedule a same-day appointment at Achilles Foot and Ankle Center and get a clear answer today.






