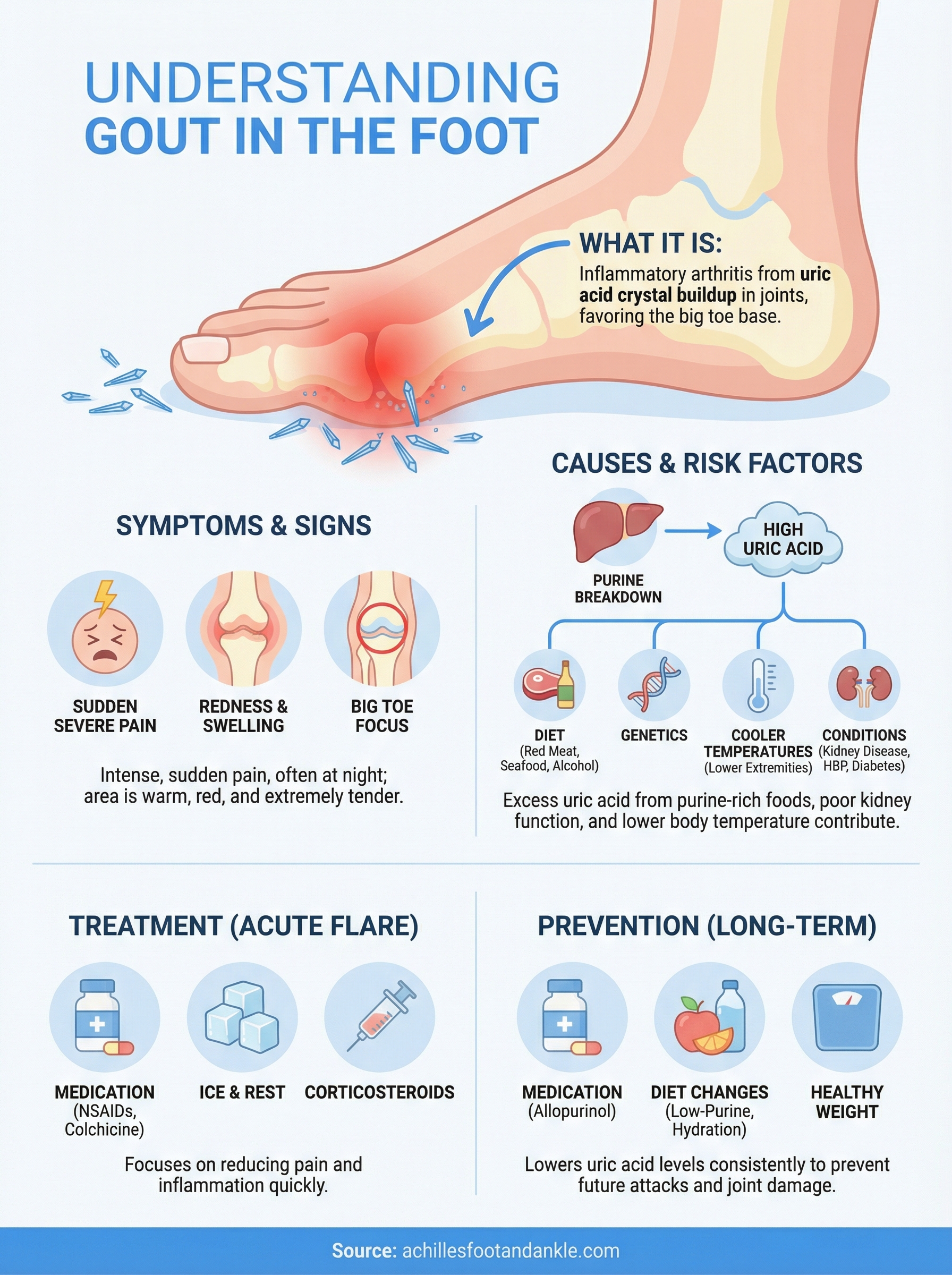
If you’ve ever been jolted awake by sudden, intense pain in your big toe or foot, you may already be wondering what is gout in the foot, and whether that’s what you’re dealing with. Gout is a form of inflammatory arthritis caused by a buildup of uric acid crystals in a joint, and it has a strong preference for the foot, especially the base of the big toe. The pain can be severe enough to make walking, wearing shoes, or even resting a bedsheet on your foot feel unbearable.
Gout affects millions of Americans, yet it’s frequently misunderstood or mistaken for other conditions like a sprain, infection, or bunion flare-up. Knowing what triggers an attack, recognizing the symptoms early, and understanding your treatment options can make a real difference in how quickly you recover, and whether you can prevent future episodes from causing lasting joint damage.
At Achilles Foot and Ankle Center, our podiatrists diagnose and treat gout across our Central Virginia locations every week. This article breaks down the symptoms, causes, risk factors, and treatment approaches so you can take the right next step, whether that’s managing your first flare or getting a long-term plan in place.
Why gout often shows up in the foot
Gout can technically affect any joint in the body, but it targets the feet, and specifically the big toe joint, more than anywhere else. This isn’t random. Several biological and physical factors work together to make your foot the ideal environment for uric acid crystals to form and accumulate, which is a key part of understanding what is gout in the foot and why it behaves differently from other types of arthritis.
Uric acid, temperature, and the lower body
Uric acid is a waste product your body produces when it breaks down purines, substances found naturally in certain foods and in your own cells. Normally, uric acid dissolves in your blood and passes out through your kidneys. When your body produces too much, or your kidneys eliminate too little, uric acid levels rise. At a certain threshold, it starts forming needle-shaped crystals called monosodium urate crystals, and those crystals settle in joints.
Cooler temperatures cause uric acid to crystallize faster, and the joints in your feet, being farthest from your core, run cooler than the rest of your body.
This temperature difference is a major reason gout attacks frequently start in the foot rather than, say, the hip or shoulder. Lower extremity joints also experience more pressure from gravity and body weight throughout the day, which may further encourage crystal deposition over time.
Why the big toe takes the most hits
The first metatarsophalangeal joint, which connects your big toe to the rest of your foot, sits at the furthest point from your heart and experiences enormous mechanical stress with every step you take. That combination of poor circulation, lower temperature, and repetitive loading creates near-perfect conditions for uric acid crystals to accumulate.
Your ankle, midfoot, and heel can also be affected, particularly in people who have experienced repeated gout episodes without treatment. Over time, crystal deposits called tophi can develop around multiple joints, causing chronic inflammation and permanent joint damage if gout goes unmanaged.
Signs and symptoms of gout in the foot
Knowing what is gout in the foot starts with recognizing its distinctive pattern. Unlike a gradual injury that builds over days, gout tends to strike fast, often overnight, with little warning before you’re dealing with pain that feels completely out of proportion to anything you’ve done.
How a gout attack typically feels
The hallmark of a gout attack is sudden, severe pain in one joint, most often the big toe. The affected area becomes red, swollen, and warm to the touch, and even light contact like a bedsheet or sock can make the pain unbearable. Most attacks peak within 12 to 24 hours and can last anywhere from a few days to two weeks if you leave them untreated.
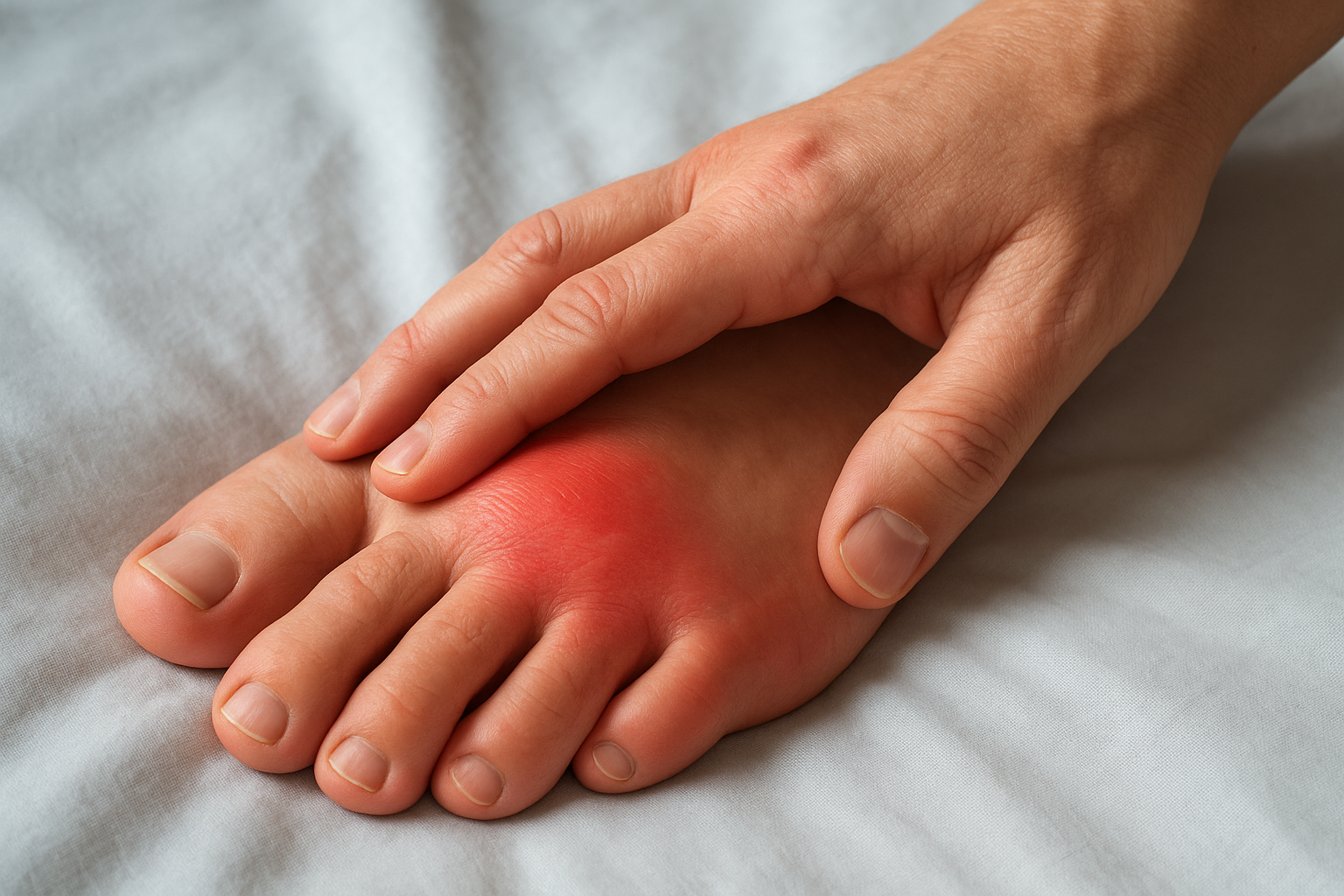
Many people describe gout pain as the worst joint pain they’ve ever experienced, which is why it rarely gets ignored after the first episode.
Other symptoms to watch for
Beyond the initial flare, you may notice lingering stiffness or soreness in the joint for several days after the worst pain fades. Some people also develop visible lumps under the skin called tophi when uric acid crystals accumulate over time without treatment. These deposits commonly form around the big toe joint, ankle, or top of the foot, and their presence signals that gout has become chronic and needs more aggressive medical management before permanent joint damage sets in.
What causes foot gout and who is at risk
Understanding what is gout in the foot requires looking at why uric acid builds up. Your body produces uric acid when it breaks down purines, compounds found in red meat, organ meats, shellfish, and alcohol. When your kidneys can’t clear it fast enough, uric acid levels rise until crystals form and settle in your joints.
What raises your uric acid levels
Several factors push uric acid beyond what your kidneys can handle. Genetics plays a meaningful role; if a close relative has gout, your own risk is higher. Certain conditions and medications also contribute:
- Chronic kidney disease reduces your filtering capacity directly
- High blood pressure and type 2 diabetes both correlate with elevated uric acid
- Diuretics commonly prescribed for blood pressure raise uric acid as a side effect
Men develop gout far more often than women, especially between ages 30 and 50, though women’s risk increases after menopause.
Diet and lifestyle factors that trigger attacks
What you eat and drink directly affects your uric acid levels. High-purine foods like organ meats, shellfish, and red meat spike uric acid quickly, and beer and liquor both increase production while reducing how well your kidneys excrete it.

Being overweight adds extra risk because excess tissue generates more uric acid and puts greater mechanical stress on your foot joints. Sugary drinks with high fructose content raise uric acid similarly to alcohol, which catches many patients off guard.
How doctors diagnose gout in the foot
Diagnosing what is gout in the foot involves more than a quick glance at a swollen toe. Your doctor will look at your full clinical picture, including your symptoms, medical history, and test results, before settling on a diagnosis, because several other conditions can look similar to gout at first.
What happens during your appointment
Your podiatrist will start by asking about the onset and pattern of your pain, including how fast it came on, which joint is affected, and whether you’ve had similar episodes before. They’ll also review your diet, alcohol use, medications, and family history since all of these feed directly into your uric acid levels. A physical exam follows, where your doctor checks for redness, swelling, warmth, and tenderness around the affected joint.
A thorough history often points strongly toward gout before any lab work comes back.
Tests that confirm the diagnosis
Your doctor will likely order a blood test to measure your uric acid levels, though it’s worth knowing that levels can be normal during an active flare, which is why your symptoms and history matter just as much. Other diagnostic tools include:
- Joint fluid analysis: Drawing fluid from the affected joint to look for uric acid crystals directly, which is the most definitive test available
- Imaging: X-rays or ultrasound can reveal crystal deposits or joint damage, especially in people with repeated episodes
Treatment and self-care for foot gout
Once you understand what is gout in the foot, treatment becomes much more straightforward. Your doctor will typically address two separate goals: stopping the current flare and preventing future attacks from happening.
Managing an acute attack
During an active flare, your doctor may prescribe nonsteroidal anti-inflammatory drugs (NSAIDs) like indomethacin or naproxen to reduce pain and swelling quickly. Colchicine is another effective option that works best when started within the first 24 hours of an attack. For patients who can’t tolerate either medication, corticosteroids, taken orally or injected directly into the joint, can bring relief fast.
Resting the affected foot and applying ice wrapped in a cloth for 20 minutes at a time can also help reduce swelling during a flare.
Long-term management and lifestyle changes
Preventing future attacks means keeping uric acid levels low on a consistent basis. Your doctor may prescribe uric acid-lowering medications like allopurinol or febuxostat, which work by reducing how much uric acid your body produces over time. Alongside medication, your daily habits carry real weight. Cutting back on alcohol and high-purine foods such as shellfish and organ meats, drinking plenty of water, and maintaining a healthy body weight all contribute to keeping your uric acid in a manageable range. Even moderate dietary changes, combined with the right medication plan, can significantly reduce both the frequency and severity of future gout attacks. Your podiatrist can help you build a personalized prevention plan that fits your health profile and lifestyle.
Next steps
Now that you understand what is gout in the foot, including how it develops, what triggers it, and how doctors treat it, you’re in a much better position to act quickly if a flare hits. The most important takeaway is that gout responds well to treatment, but only when you address it promptly. Waiting out repeated attacks without medical care raises the risk of permanent joint damage and more frequent episodes over time.
If your foot pain came on suddenly, feels severe, and involves redness and swelling around your big toe or ankle, don’t guess about the cause. A podiatrist can confirm your diagnosis and build a treatment and prevention plan tailored to your uric acid levels, health history, and daily habits. The team at Achilles Foot and Ankle Center serves patients across Central Virginia and offers same-day appointments for urgent concerns. Schedule your foot gout evaluation today and get answers fast.






