Stress fractures don’t always come from a single bad step or a dramatic fall. Most of the time, they develop gradually, tiny cracks in bone caused by repetitive force that outpaces your body’s ability to repair itself. Understanding stress fracture risk factors is the first step toward figuring out whether you’re vulnerable and, more importantly, what you can do about it.
Some risk factors are within your control, like training habits and footwear choices. Others, such as bone density, foot structure, and hormonal health, are less obvious but equally significant. Whether you’re a runner ramping up mileage, someone managing a metabolic condition, or simply noticing persistent foot pain that won’t quit, knowing what puts you at risk can change the outcome.
At Achilles Foot and Ankle Center, our podiatrists diagnose and treat stress fractures across our Central Virginia locations every week. This article breaks down the causes, warning signs, and practical prevention strategies so you can protect your feet and ankles before a small problem becomes a serious one.
Why stress fracture risk factors matter
Most people think of fractures as something that happens all at once: a bad landing, a car accident, a hard fall. Stress fractures work differently. Repetitive mechanical loading gradually overwhelms your bone’s natural repair cycle, and the damage accumulates invisibly over days or weeks. By the time pain becomes noticeable, the injury is often well underway. That’s exactly why understanding stress fracture risk factors matters so much: it shifts you from reacting to an injury to preventing one.
Stress fractures versus acute fractures: a key difference
An acute fracture results from a single, high-force event. A stress fracture, by contrast, is the product of cumulative microtrauma, tiny cracks that form when bone remodeling can’t keep pace with the stress placed on it. Your body is constantly breaking down and rebuilding bone tissue in a process called remodeling. When breakdown happens faster than rebuilding, weak spots develop. Understanding this distinction matters because the treatment approach, recovery timeline, and preventive strategies are fundamentally different from what a standard broken bone requires.
A stress fracture caught early can often be managed conservatively; the same fracture ignored for weeks may require surgery or extended immobilization.
Why risk factors are not always obvious
Many people who develop stress fractures don’t consider themselves high-risk. They’re not necessarily elite athletes or elderly patients with osteoporosis. A recreational runner who suddenly increases weekly mileage, a worker who spends long hours on hard floors, or a young woman with irregular menstrual cycles can all develop stress fractures without any single dramatic cause. That’s the challenge: several overlapping factors often combine to create the conditions for an injury, and none of them alone would seem alarming on its own.
Recognizing your individual risk profile requires looking at the full picture, from your bone density and nutritional status to your footwear, training load, and foot mechanics. Most stress fractures are preventable when you identify those factors early and make targeted adjustments before the damage accumulates.
What happens when risk factors go unaddressed
Ignoring stress fracture risk factors doesn’t just increase your chance of developing one injury; it raises the odds of repeat fractures and longer recoveries. Individuals who sustain one stress fracture without addressing the underlying causes are significantly more likely to experience another. Left untreated, some stress fractures progress to complete fractures, which carry a far more serious recovery burden and, in certain bones like the hip or navicular, can result in long-term complications including avascular necrosis or chronic instability.
Catching a stress fracture in its early stages and addressing the root causes is the difference between a few weeks of modified activity and months of rehabilitation. That outcome depends almost entirely on how well you understand and manage your own risk.
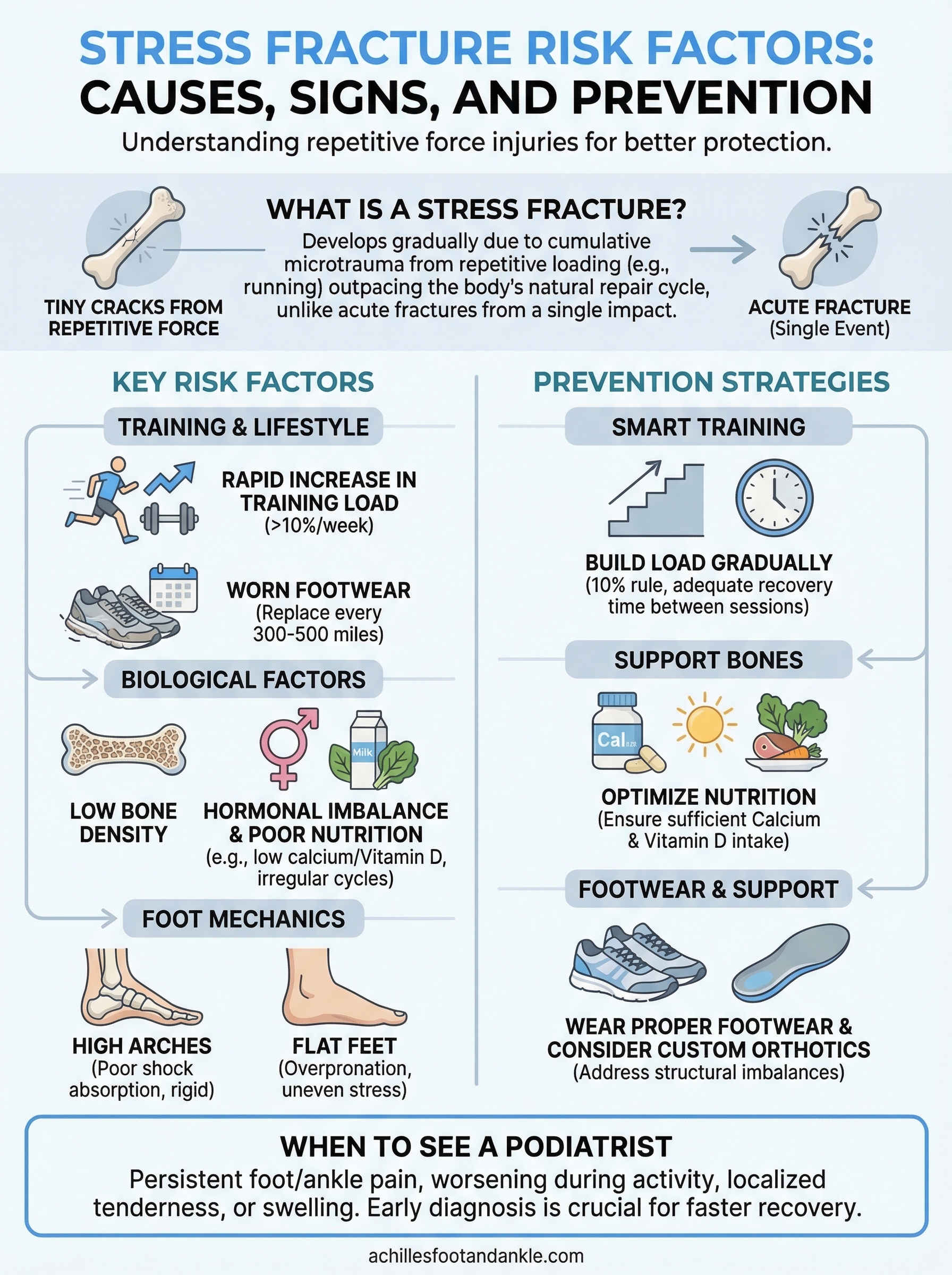
The biggest stress fracture risk factors
Certain factors consistently appear across clinical practice as the strongest predictors of stress fracture injury. While any single factor can raise your risk, the real danger comes when multiple factors combine in the same person over the same stretch of time. Knowing which ones apply to you gives you something concrete to act on.
Sudden increases in training load
Your bone needs time to adapt to new levels of stress. When you increase your training volume or intensity too quickly, the remodeling process falls behind, and microcracks accumulate faster than your body can repair them. This is one of the most widely recognized stress fracture risk factors in runners, military recruits, and anyone returning to activity after a break or illness.
Returning to full training too soon after time off puts you at a sharply elevated risk, even if the prior activity level felt manageable before the break.
A commonly cited guideline in sports medicine recommends increasing weekly mileage by no more than 10 percent at a time, giving bone remodeling a realistic chance to keep pace with demand. Skipping recovery days or stacking hard efforts on back-to-back days compounds the problem significantly.
Low bone density, hormonal health, and nutrition
Bone density directly determines how much repeated loading your skeleton can handle before damage accumulates. Lower density means a smaller structural reserve, and your bones reach a tipping point faster. Women who experience irregular or absent menstrual cycles are particularly vulnerable because estrogen plays a central role in bone formation, and disruptions to hormonal balance can quietly reduce bone strength over months.
Your diet matters just as much. Bones depend on adequate calcium and vitamin D to maintain density and support repair between training sessions. A diet consistently low in either nutrient, whether from restricted calorie intake, food avoidance, or limited sun exposure, reduces your body’s ability to keep pace with the daily demands of bone remodeling.
Foot and ankle factors that raise your risk
The structure of your foot shapes how force travels through your body with every step. When your foot mechanics are off, stress distributes unevenly across your bones, and certain areas absorb far more load than they should. These biomechanical patterns are among the most overlooked stress fracture risk factors in active patients.
Foot structure and how it distributes load
High arches and flat feet both create mechanical imbalances that concentrate stress in predictable locations. A high-arched foot is rigid and absorbs shock poorly, so the metatarsals and heel take on disproportionate impact with each stride. A flat foot, by contrast, tends to overpronate, which shifts load toward the inner edge of the foot and increases strain along the second and third metatarsals over time.
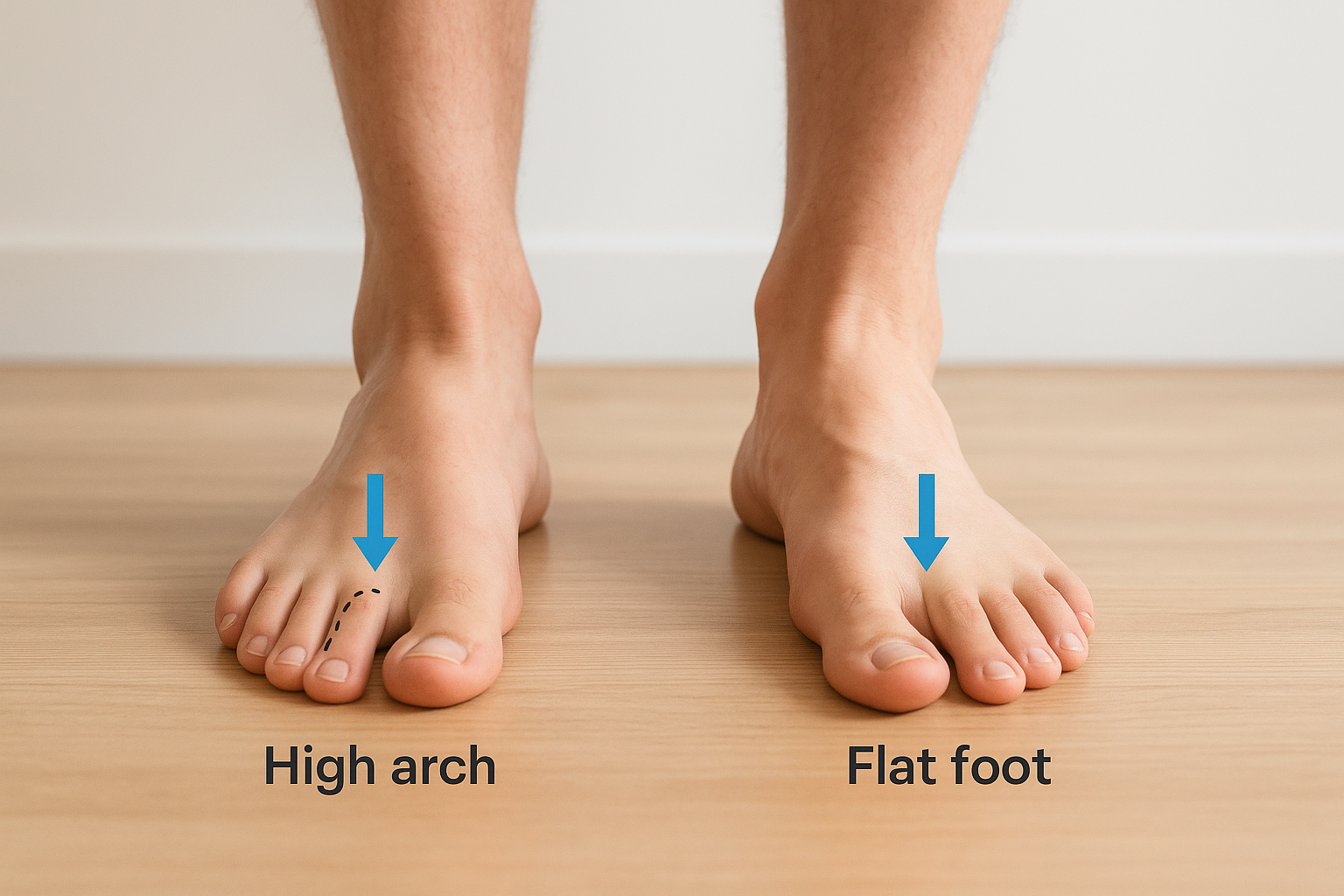
Your foot type doesn’t guarantee a stress fracture, but it does tell you exactly where you’re most vulnerable and which preventive steps matter most.
If you have a structural imbalance, custom orthotics can redistribute pressure more evenly and significantly reduce your risk of developing a stress fracture over a training cycle.
Previous injuries and worn footwear
A prior stress fracture raises your risk of developing another one, particularly if the underlying mechanics or training habits that caused the first injury haven’t changed. Your bone may have healed structurally, but the same forces will act on it again in the same way unless something shifts in how you move or how much load you apply.
Worn-out footwear compounds the problem. Shoes lose cushioning and support well before they look visibly damaged, and once that support degrades, your foot absorbs far more ground-reaction force than it was designed to handle. Replacing athletic shoes based on mileage rather than appearance, typically every 300 to 500 miles, is a straightforward step that protects your foot structure under repeated load.
How to lower your risk and prevent stress fractures
Preventing a stress fracture isn’t about avoiding activity; it’s about managing load intelligently and supporting your body’s ability to keep pace with the demands you place on it. Most of the well-known stress fracture risk factors are addressable, and even small, consistent changes in how you train, eat, and equip yourself can meaningfully reduce your odds of developing one.
Build load gradually and protect your recovery
The most reliable prevention strategy is also the most straightforward: increase training volume slowly and build in adequate recovery time between sessions. Your bone needs roughly 48 to 72 hours between high-impact efforts to complete a remodeling cycle, and skipping that window repeatedly is what tips the balance toward injury. Cross-training with low-impact activity like swimming or cycling on off days keeps your fitness up while giving your bones the time they need to rebuild.

A few practical steps that support safe load progression:
- Increase weekly mileage or intensity by no more than 10 percent at a time
- Alternate hard training days with lighter recovery days
- Replace athletic footwear every 300 to 500 miles, not just when it looks worn
- Rotate between two pairs of shoes to extend cushioning life and support
Support your bones through nutrition and footwear
Calcium and vitamin D are the two nutrients most directly tied to bone density, and many active people fall short of both without realizing it. Adults generally need 1,000 to 1,200 mg of calcium daily and enough vitamin D to absorb it effectively. If your diet consistently falls short in dairy, leafy greens, or fortified foods, a targeted supplement can close that gap and reduce your fracture risk over time.
Wearing the right footwear for your foot type and activity is one of the lowest-cost, highest-impact changes you can make to protect your bones.
Footwear matters beyond cushioning alone. Shoes designed for your specific foot mechanics, whether you have a high arch, flat foot, or neutral alignment, distribute ground-reaction force more evenly and reduce the localized stress that leads to microcracks over time.
When to see a podiatrist and what to expect
Knowing your stress fracture risk factors is useful, but recognizing when to act on symptoms is what actually protects your long-term function. Persistent foot or ankle pain that doesn’t ease with rest after a few days, especially pain that gets worse during activity and fades when you stop, is a pattern worth taking seriously. Waiting too long to get an evaluation is one of the most common reasons a manageable injury becomes a prolonged one.
Signs that need professional evaluation
Pain that worsens progressively during a run or workout, localized tenderness when you press on a specific bone, and mild swelling without a clear injury event are all signals that something more than general soreness may be going on. You don’t need to wait until you can’t walk to seek care.
If your pain consistently appears at the same point in your activity and fades with rest, that pattern alone warrants an evaluation, not watchful waiting.
Common signs that indicate a podiatrist visit is appropriate include:
- Localized bone tenderness that you can pinpoint with one finger
- Pain that begins earlier and earlier into activity over successive sessions
- Swelling or bruising around a foot or ankle bone without a known trauma
- Pain that continues at rest or interrupts sleep
What a podiatrist will do
Your podiatrist will start with a thorough physical examination, including pressing along specific bones to identify point tenderness, which is a reliable early indicator of a stress fracture even before imaging shows a visible crack. Depending on your symptoms and history, they may order X-rays or an MRI to confirm the diagnosis and assess severity. X-rays often miss early-stage stress fractures, so an MRI gives a clearer picture when clinical suspicion is high.
From there, your treatment plan might include activity modification, protective footwear, a walking boot, or custom orthotics to offload the affected bone while it heals. If structural or biomechanical factors contributed to the injury, your podiatrist will address those directly to reduce the risk of a recurrence.
A simple plan to protect your bones
Reducing your risk of a stress fracture comes down to a few consistent habits applied over time. Increase your training load gradually, support your bone density through adequate calcium and vitamin D, and replace your footwear before it loses its structural support. If your foot mechanics put you at higher risk, custom orthotics can redistribute load before damage accumulates. None of these steps require dramatic changes to your routine; they require attention to the details most people overlook until something hurts.
Knowing your stress fracture risk factors gives you a real advantage, but acting on that knowledge is what actually makes a difference. If you’re already dealing with persistent foot or ankle pain, or you want a professional evaluation of your bone health and biomechanics, don’t wait for the injury to get worse. Schedule a same-day appointment with our podiatrists at Achilles Foot and Ankle Center and get a clear path forward.






