A stress fracture foot from running doesn’t always announce itself with a dramatic moment. There’s no pop, no twist, no obvious injury. Instead, it starts as a dull ache that you brush off, until one morning you step out of bed and the pain stops you mid-stride. Stress fractures are among the most common overuse injuries runners face, and the metatarsal bones of the foot absorb more repetitive force than most people realize.
The tricky part is knowing when that nagging soreness crosses the line from normal training fatigue into actual bone damage. Ignoring a stress fracture, or misdiagnosing it as something less serious, can turn a few weeks of rest into months of recovery. The good news is that with early detection and the right treatment plan, most runners return to full activity without lasting problems.
At Achilles Foot and Ankle Center, our podiatrists across Central Virginia diagnose and treat running-related stress fractures regularly, using advanced imaging like digital X-ray and ultrasound to catch fractures early and build recovery plans that actually get runners back on their feet. This article covers everything you need to know, from recognizing the first symptoms to understanding your treatment options and realistic recovery timeline.
Why runners get foot stress fractures
Running is a high-impact activity, and every foot strike sends force equivalent to two to three times your body weight through the bones of your foot. Your bones handle this by continuously remodeling, breaking down old bone tissue and building new tissue in its place. When the rate of breakdown outpaces the rate of repair, small cracks form in the bone. That’s a stress fracture. Unlike a traumatic fracture caused by a single incident, a stress fracture builds gradually over days or weeks of repeated loading.
The mechanics of repetitive bone stress
Your foot contains 26 bones, and the metatarsals (the five long bones running from your midfoot to your toes) absorb the most punishment during running. The second and third metatarsals are the most commonly fractured because they bear the greatest proportion of force during push-off. Each running stride compresses and bends these bones slightly, and over hundreds or thousands of steps, that stress accumulates. When your muscles fatigue and can no longer absorb shock efficiently, more of that force transfers directly to the bone, accelerating the damage.
Most stress fractures in runners develop not from a single bad run but from a gradual buildup of load that the bone never fully recovers from between sessions.
Training errors that raise your risk
Sudden increases in mileage or intensity are the single biggest driver of stress fractures from running. Many runners push weekly mileage increases well beyond what bone tissue can adapt to in time. Running on hard surfaces like concrete or asphalt amplifies ground reaction forces compared to softer surfaces like grass or a rubberized track. Worn-out shoes that have lost their cushioning contribute to the same problem, and switching to minimalist footwear too quickly shifts loading patterns before your bones have adapted.
Recovery timing matters as much as training volume. Rest days give your bones time to complete the remodeling cycle that makes them stronger, and compressing multiple hard running days back to back removes that window entirely, allowing cumulative stress to build faster than the bone can repair itself.
Foot structure and bone density factors
Your individual anatomy plays a real role in stress fracture foot from running risk. High-arched feet distribute force unevenly across the metatarsals, concentrating stress in specific spots rather than spreading it across the whole structure. Flat feet, on the other hand, alter gait mechanics in ways that can overload the medial structures of the foot with each stride. Low bone density, whether from nutritional gaps, hormonal factors, or conditions like osteoporosis, makes bones less capable of tolerating repetitive load over time. Female runners face a higher risk partly because of the relationship between low estrogen levels and calcium absorption, a pattern sometimes associated with the female athlete triad and reduced bone mineral density.
Signs you may have a foot stress fracture
A stress fracture foot from running rarely announces itself with sudden, severe pain. The symptoms tend to be subtle early on, which is exactly why so many runners dismiss them as normal soreness and keep training. Knowing what to look for specifically can save you weeks of unnecessary recovery time.
Pain that follows a predictable pattern
The hallmark sign of a stress fracture is pain that gets worse with activity and improves with rest. You’ll typically notice a dull ache during a run that fades once you stop. As the fracture progresses, the pain may start earlier in your run, last longer afterward, and eventually appear just from walking or standing. If you notice that the discomfort has shifted from "sore after a hard workout" to "hurts the moment I start moving," that pattern is a strong indicator that something structural is happening in the bone.
If your foot pain is consistently worse at the start of activity and improves mid-run only to return sharply afterward, do not push through it, because bone stress injuries worsen with continued loading.
Localized tenderness and visible changes
Press firmly along the top of your foot, especially over the second or third metatarsal bones, which run from your midfoot toward your smaller toes. A stress fracture typically produces very specific, pinpoint tenderness at one spot rather than a broad, diffuse ache. This focal tenderness separates stress fractures from softer tissue injuries like tendinitis, which tends to produce more distributed soreness along a tendon or muscle.
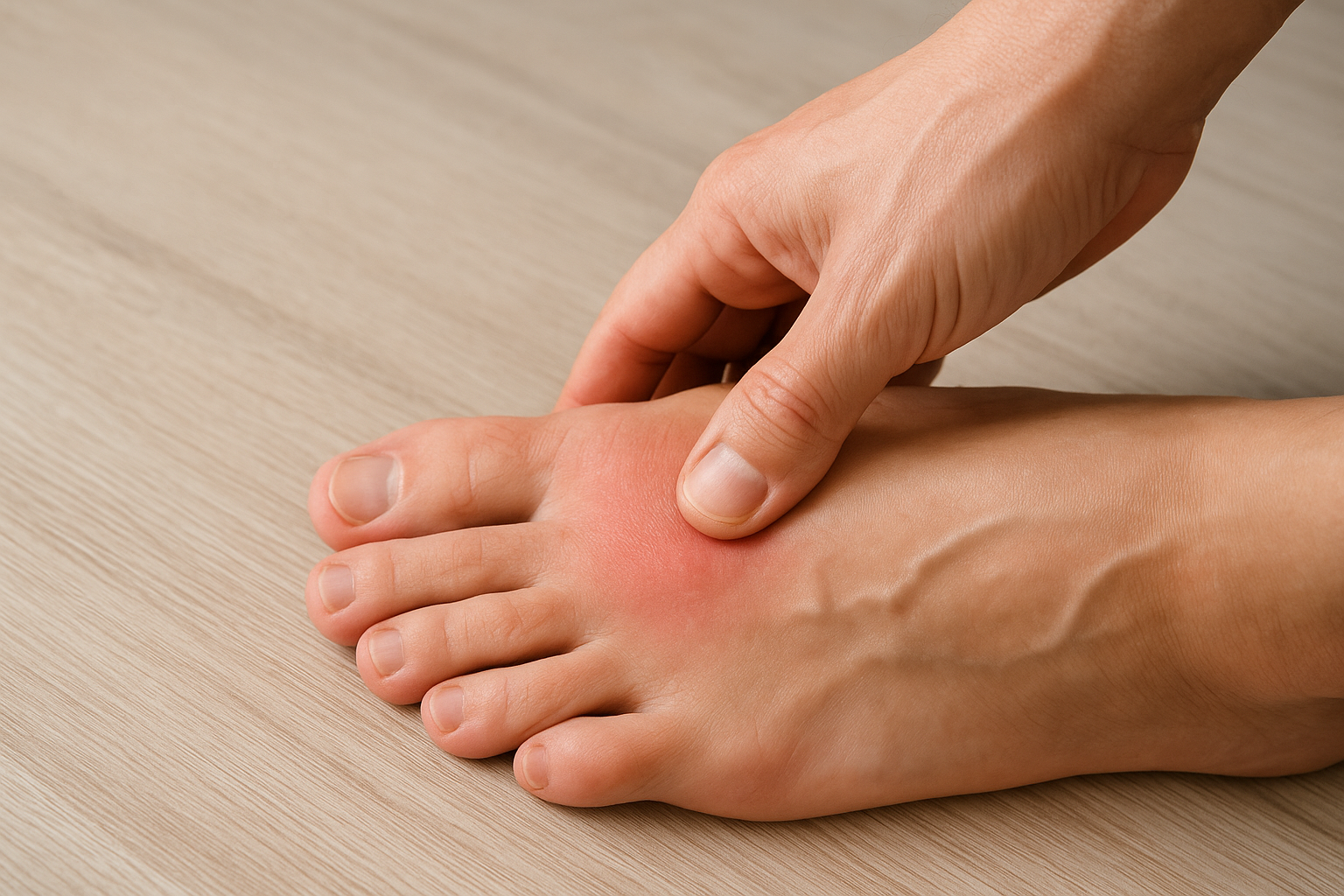
Some runners also notice mild swelling or faint bruising along the top of the foot, though these signs are not always present, particularly in early-stage fractures. The absence of visible swelling does not rule out a stress fracture. Pressing on a specific point of your foot that produces sharp, localized pain is a reason to stop running and get a proper evaluation before the damage progresses further.
How doctors diagnose a running stress fracture
When you walk into a podiatrist’s office with symptoms consistent with a stress fracture foot from running, the diagnostic process follows a clear path. Your doctor starts by gathering a detailed history of your training habits and recent mileage increases, along with when the pain first appeared. This conversation alone provides critical clues before any imaging takes place.
Physical examination
Your podiatrist will apply direct pressure to specific bones in your foot to locate the point of maximum tenderness. This point-specific tenderness test is highly informative because stress fractures produce sharp, localized pain at the fracture site, which is distinct from the broader discomfort of a soft tissue injury.
Foot structure and gait mechanics are also part of the assessment. Your doctor checks for biomechanical factors, such as a high arch or flat foot, that may have contributed to the injury. Understanding the root cause helps your provider build a treatment and prevention plan that addresses why the fracture happened, not just the fracture itself.
Imaging tests
X-rays are usually the first imaging step, but they carry a significant limitation. Early-stage stress fractures often don’t appear on X-ray until the bone starts healing and visible callus forms, which can take two to three weeks. Because of this, your podiatrist may order an MRI or bone scan when clinical suspicion is high but X-rays look normal.
MRI is particularly reliable for catching stress fractures early because it detects bone marrow edema, the internal swelling that signals stress injury before a visible crack appears on standard imaging.
Advanced practices like Achilles Foot and Ankle Center use digital X-ray and diagnostic ultrasound in-office, which shortens the time between your appointment and a confirmed diagnosis. Getting the imaging right the first time prevents the common mistake of treating a stress fracture as a sprain or tendon problem, a mistake that delays proper recovery significantly.
How to treat a foot stress fracture
Treatment for a stress fracture foot from running depends on which bone is fractured and how severe the damage is. Most cases respond well to conservative, non-surgical management, but starting treatment early is critical. The longer you continue loading a fractured bone, the higher the risk of a complete fracture that leads to a significantly longer and more complicated recovery.
Rest and offloading
Stopping all high-impact activity is the first and most important step. Your doctor will typically recommend a period of protected weight-bearing, which often means wearing a stiff-soled walking boot or using crutches to reduce the load on the injured bone while it heals. The boot limits the bending forces traveling through your foot and gives the bone a stable environment to repair itself without constant disruption.
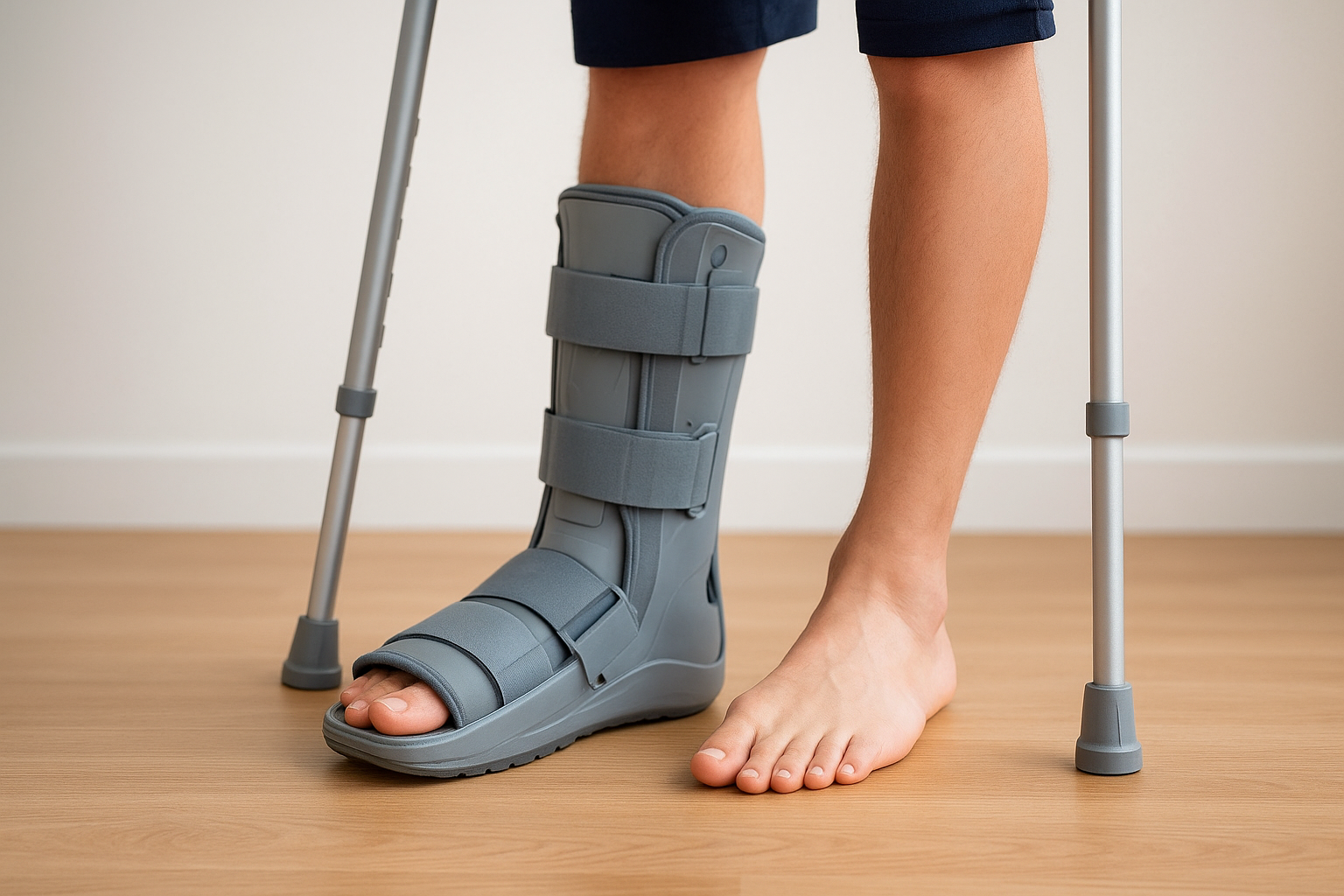
Some fractures require stricter protocols depending on their location. Stress fractures in high-risk sites such as the proximal fifth metatarsal or the navicular bone have limited blood supply, which slows healing and demands more conservative load management from the start.
Continuing to run on a diagnosed stress fracture can convert a partial crack into a complete fracture, extending your recovery significantly and potentially making surgical repair necessary.
Supportive devices and surgical options
Once you begin transitioning out of the boot, your podiatrist may recommend custom orthotics to correct the biomechanical factors that contributed to the original injury, such as abnormal arch mechanics or uneven load distribution across the metatarsals. Replacing worn-out running shoes is part of this same process, since adequate cushioning directly reduces ground reaction forces during your return to activity.
Most runners do not need surgery, but certain fractures require it. Locations with poor blood supply and a high nonunion rate often need internal fixation with screws to hold the bone in place while it heals. Your podiatrist will use imaging findings and fracture severity to determine whether surgical intervention is the right path before any procedure is scheduled.
Recovery timeline and return to running safely
Recovery from a stress fracture foot from running typically takes six to eight weeks for most metatarsal fractures, though the exact timeline depends on which bone is involved, how severe the damage is, and how consistently you follow your treatment plan. High-risk fractures in bones with limited blood supply can take three to four months or longer before you’re cleared to return to activity.
What to expect during the healing window
The first two to three weeks focus on offloading the bone completely and reducing any residual inflammation. You’ll likely spend most of this period in a walking boot, and your podiatrist will monitor how your symptoms respond. By weeks four through six, most low-risk fractures show enough bone healing on imaging to begin a gradual transition back to weight-bearing activity without the boot. Pain levels during daily walking serve as a reliable guide during this phase, because a bone that still hurts during normal movement is not ready for running.
Returning to running too early is the most common reason stress fractures recur, and a second fracture in the same location heals more slowly than the first.
How to return to running without re-injury
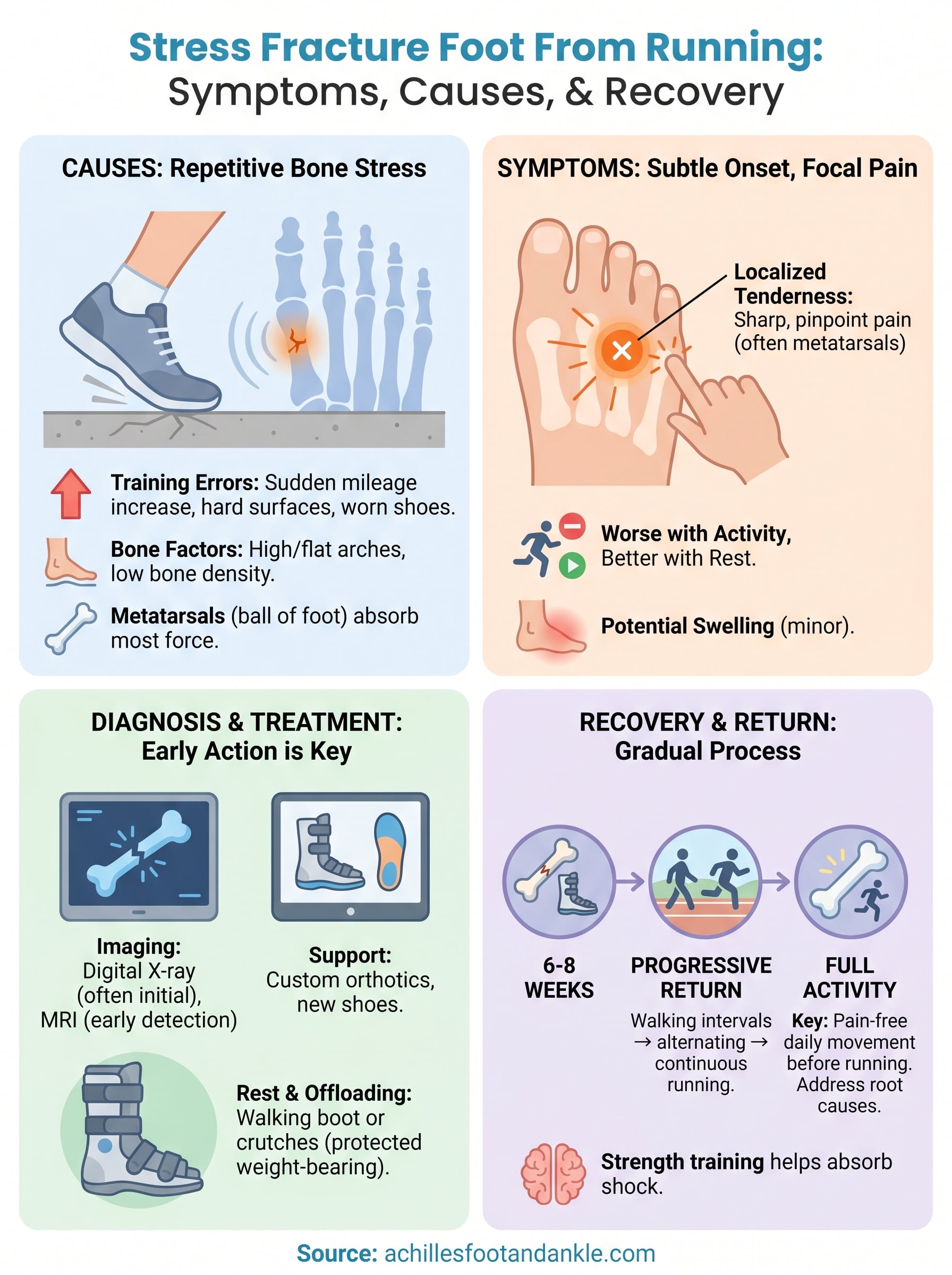
Your return should follow a structured, progressive plan that increases load in small increments rather than jumping back to your previous mileage. Most podiatrists recommend starting with walking intervals, then alternating short running segments with walking before building toward full continuous runs over several weeks. Running on softer surfaces like grass or a track during the initial weeks reduces the impact load on recovering bone.
Address the factors that caused the injury in the first place before you increase intensity. Switching to properly cushioned footwear, correcting biomechanical issues with custom orthotics, and building mileage no faster than ten percent per week all reduce the chance that you’ll end up back in a boot. Strength training for the lower leg also helps your muscles absorb more of the shock that would otherwise transfer to your bones during each stride.
Next steps if your foot still hurts
Foot pain that lingers beyond a few days of rest deserves a professional evaluation, not more waiting. A stress fracture foot from running can look identical to a sprain or tendon problem without proper imaging, and treating the wrong injury wastes time while the real problem gets worse. If your foot still hurts after reducing your activity, or if the pain is sharp and localized over a specific bone, the right move is to see a podiatrist who can confirm the diagnosis and start the correct treatment immediately.
Your recovery depends on acting before the damage progresses further. Achilles Foot and Ankle Center has thirteen locations across Central Virginia and offers same-day appointments so you do not have to wait weeks to get answers. The team uses in-office digital imaging to catch stress fractures early and build a return-to-running plan built around your specific injury. Schedule a same-day appointment and get back on the road faster.






