You feel a sharp ache in the bottom of your foot every time you stand up, but you’re not sure what’s causing it. When you search arch pain vs plantar fasciitis, you’ll find that the two conditions overlap quite a bit, and that overlap is exactly what makes them hard to tell apart without a closer look at your specific symptoms.
Here’s the thing: arch pain is a broad term that covers several possible causes, from fallen arches and tendon strain to stress fractures. Plantar fasciitis is one specific condition, inflammation of the plantar fascia ligament, that happens to produce pain in the arch area. So while all plantar fasciitis involves arch pain, not all arch pain is plantar fasciitis. That distinction matters because the right treatment depends on an accurate diagnosis.
At Achilles Foot and Ankle Center, our podiatrists evaluate and treat both conditions daily across our Central Virginia locations. This article breaks down the key differences in symptoms, pain patterns, and causes so you can start understanding what’s going on with your feet, and know when it’s time to get professional help.
Why Arch Pain and Plantar Fasciitis Get Confused
The bottom of your foot is a compact, interconnected system of bones, tendons, ligaments, and muscles. When something goes wrong in that space, pain signals don’t come with a label. You feel discomfort somewhere along the arch or heel, and your brain has to work out the rest. That’s the core reason these two conditions get mixed up so often: they share the same general territory, and the body isn’t precise about telling you which structure is actually the problem.
The Anatomy Sets Up the Confusion
Your plantar fascia is a thick band of connective tissue that runs directly along the bottom of your foot, connecting your heel bone to the base of your toes. It forms the primary support structure of your arch. When it becomes inflamed, pain shows up in the arch area. But your arch is also supported by several other structures, including the posterior tibial tendon, the intrinsic foot muscles, and the plantar ligaments. A problem with any of these can produce pain that feels almost identical from the outside.
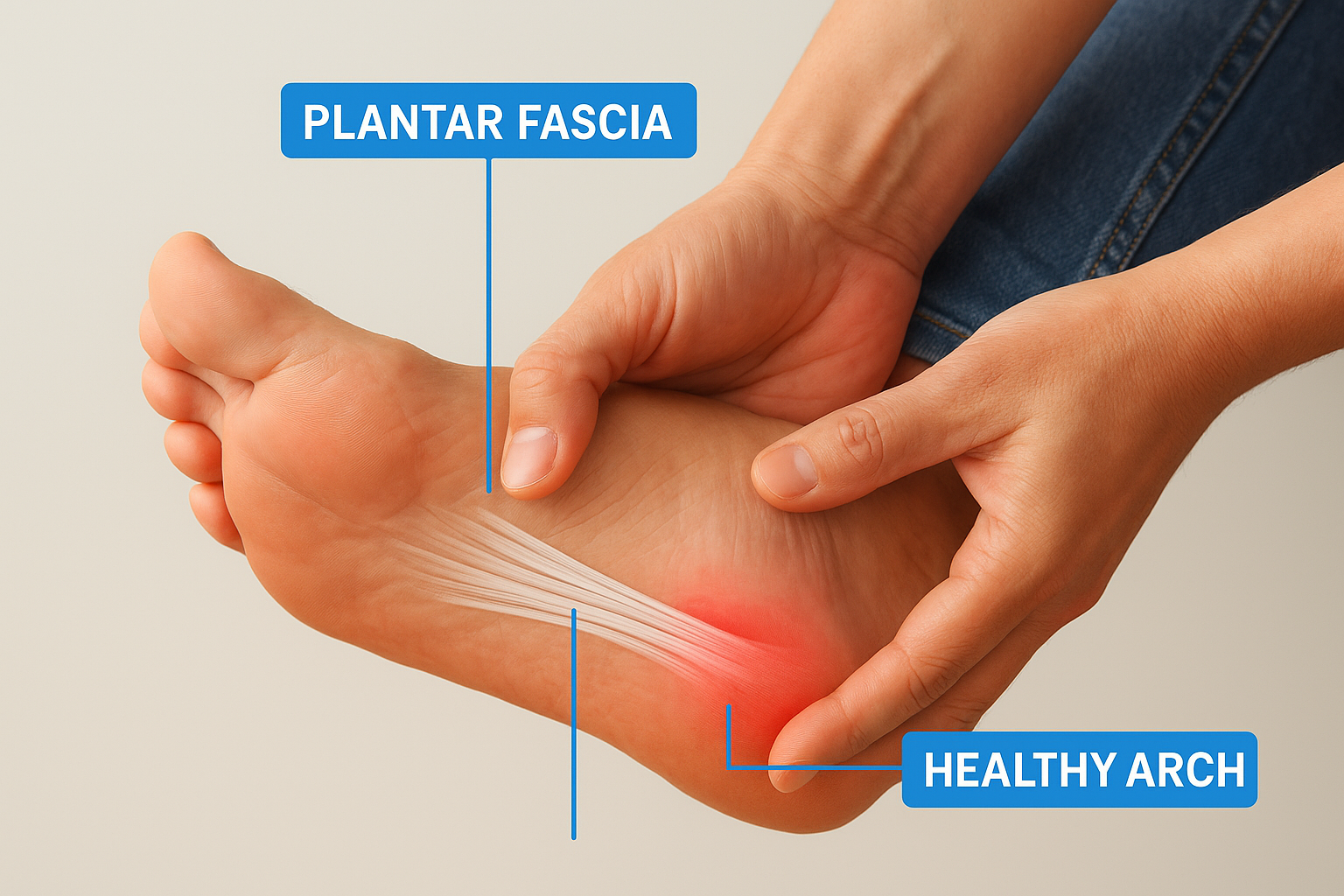
Because the plantar fascia sits at the center of your arch anatomy, plantar fasciitis pain and general arch pain can feel indistinguishable without a targeted clinical evaluation.
The Symptoms Overlap in Real Ways
When people research arch pain vs plantar fasciitis, they quickly notice the symptom descriptions sound nearly the same. Both conditions can cause a dull ache that sharpens with prolonged standing or activity. Both can make your first steps in the morning feel sharp and punishing. The timing and exact location of your pain are the details that actually separate them, but picking up on those details requires careful attention that most people haven’t been trained to apply.
Another layer of confusion comes from how pain spreads across your foot. Plantar fasciitis typically starts near the heel and radiates forward, but some people feel it primarily in the mid-arch, which mimics other arch conditions closely. General arch pain from a fallen arch or tendon strain often covers a wider area without the concentrated heel focus. Without knowing what to look for, even attentive patients struggle to tell the difference based on sensation alone.
What Arch Pain Can Mean and Common Causes
"Arch pain" is not a diagnosis. It’s a symptom, and multiple different conditions can produce it. When you compare arch pain vs plantar fasciitis, you first need to understand that arch pain is the umbrella term and plantar fasciitis fits under it as just one possible cause. Identifying the right cause requires looking at where the pain sits, when it appears, and what makes it better or worse.
Conditions That Commonly Cause Arch Pain
Several structural and tissue-related problems produce pain along the arch of your foot. Flat feet (fallen arches) occur when the arch collapses during weight-bearing, putting excess strain on surrounding tendons and ligaments. Posterior tibial tendon dysfunction is another common culprit, where the tendon responsible for holding your arch up begins to weaken or tear.
If your arch pain spreads across the entire midfoot rather than concentrating near the heel, a fallen arch or tendon problem is often the more likely cause than plantar fasciitis.
Other conditions that produce arch pain include:
- Stress fractures in the metatarsal or navicular bones
- Tarsal coalition, a structural problem where foot bones fuse together abnormally
- Overpronation, where your foot rolls inward excessively during each step
- Tight calf muscles, which pull on the plantar fascia and surrounding structures
Understanding which of these applies to you matters because each condition requires a different treatment approach, and using the wrong treatment for your actual problem often delays real recovery.
What Plantar Fasciitis Is and Its Classic Pattern
Plantar fasciitis happens when the plantar fascia ligament becomes irritated and inflamed, usually from repeated stress that the tissue can’t fully recover from. Unlike the broader category of arch pain vs plantar fasciitis, this condition has a specific mechanical cause: the plantar fascia absorbs load with every step, and when that load consistently exceeds what the tissue can handle, small tears and inflammation develop along the band.
The Pain Pattern That Defines It
The hallmark of plantar fasciitis is sharp heel pain with your first steps in the morning. This happens because the plantar fascia tightens during rest, then gets suddenly stretched when you stand. Your pain often eases after a few minutes of walking, then returns after long periods of activity or standing. That cycle of morning pain, brief relief, and later flare-up is the clearest signal that plantar fasciitis is driving your symptoms.
If your worst pain hits during those first few morning steps and improves once you’ve been moving for several minutes, plantar fasciitis is a strong possibility.
Who Gets It and Why
Plantar fasciitis is most common in runners, people who stand for long hours, and those who carry extra body weight. Tight calf muscles and footwear that lacks adequate arch support are also significant contributing factors. Several groups face elevated risk:
- Middle-aged adults
- People who recently increased their activity level
- Those with flat feet or high arches
- Workers who spend most of their day on hard surfaces
How to Tell the Difference Based on Symptoms
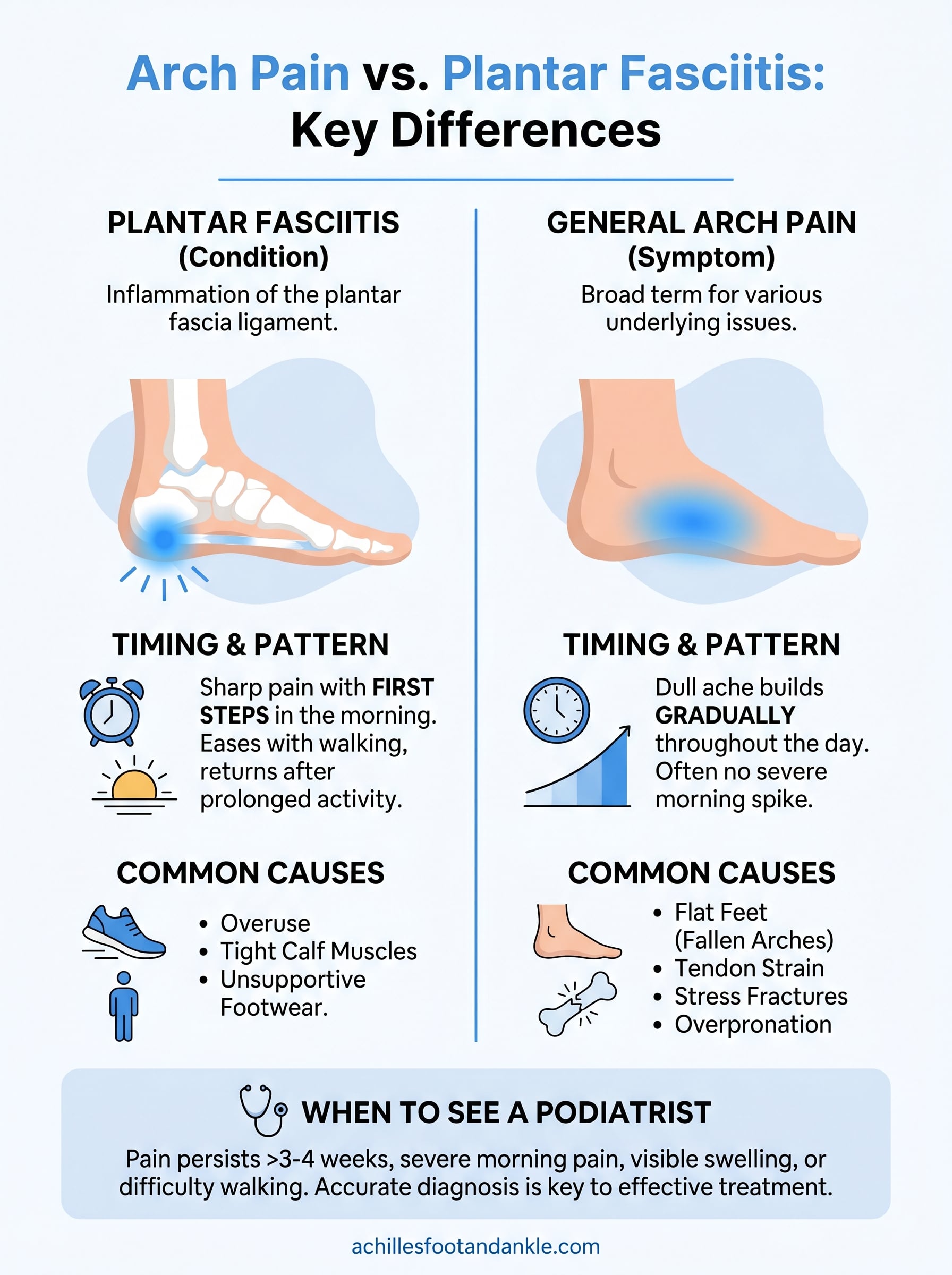
When comparing arch pain vs plantar fasciitis, two factors cut through most of the confusion: where your pain concentrates and when it hits hardest. Plantar fasciitis pain focuses near the heel and is worst at the start of the day. General arch pain from flat feet or tendon problems tends to spread across the midfoot and doesn’t follow that same morning-spike pattern.
Focus on Location and Timing
Your pain location is your first clue. Plantar fasciitis almost always produces pain at or just in front of the heel, along the inside edge of the foot. If you press your finger into the base of your heel and that spot feels distinctly tender, plantar fasciitis is a strong suspect. Arch pain from other causes typically covers a broader zone, often across the entire midfoot without one concentrated sore point.
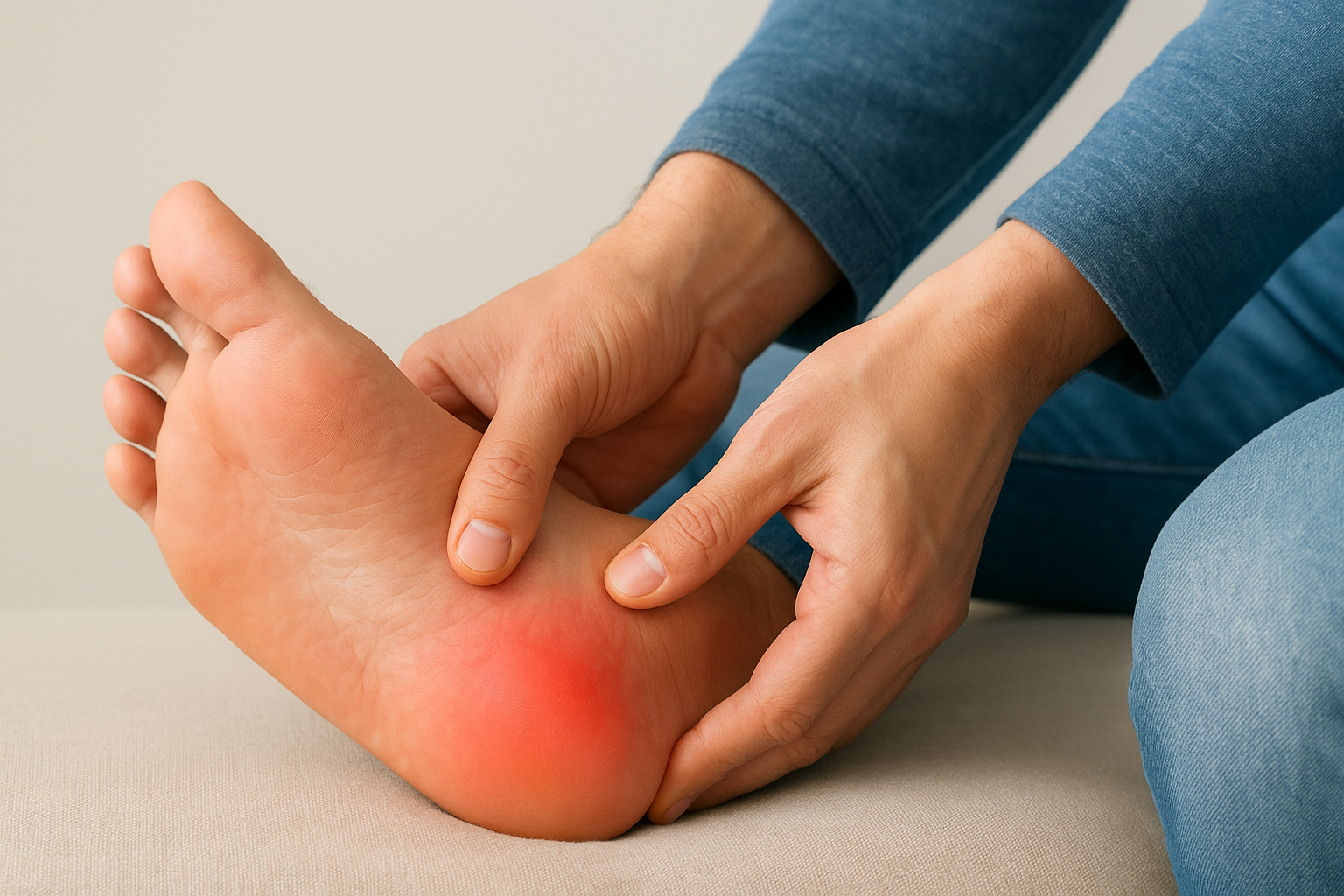
Pressing firmly on your heel and finding one distinct tender spot is one of the clearest physical signals that plantar fasciitis is the likely cause.
Timing adds the second layer of information. Plantar fasciitis follows a predictable cycle: severe morning pain that eases with movement, then returns after long periods of activity. With other arch conditions, pain often builds gradually throughout the day without that early-morning spike. Tracking when your pain peaks and when it eases gives you and your podiatrist useful data for narrowing down the cause, so paying attention to your daily pattern before your appointment is worth the effort.
When to See a Podiatrist and What to Expect
Self-assessment gets you only so far. When you can’t resolve arch pain vs plantar fasciitis on your own, or when home care isn’t reducing your pain after a few weeks, a podiatrist gives you the clinical evaluation that actually confirms what’s going on. Continuing to guess and treat the wrong condition wastes time and can allow the real problem to worsen.
If your pain has lasted more than three to four weeks despite rest and conservative care, scheduling an appointment is the right move.
Signs You Should Not Wait
Some situations call for prompt professional attention rather than a wait-and-see approach. See a podiatrist soon if your pain appeared after a specific injury, if you notice visible swelling or bruising along the arch, or if walking has become significantly difficult. These signs point toward conditions that need imaging and clinical assessment, not just stretching.
- Pain that wakes you at night
- Numbness or tingling in the arch or heel
- Sudden worsening after a period of improvement
- Inability to bear weight on the foot
What Your Appointment Involves
Your podiatrist will review your pain history, activity level, and footwear, then perform a physical exam to pinpoint the tender areas. Digital X-rays and ultrasound imaging help confirm whether the plantar fascia is inflamed or whether a structural issue like a tendon problem or stress fracture is involved. From there, your care team builds a targeted treatment plan specific to your actual diagnosis.
Next Steps for Lasting Relief
Now that you understand the key differences in arch pain vs plantar fasciitis, the next step is putting that knowledge to work. Waiting out foot pain rarely produces results, and both conditions respond better to early, targeted treatment than to weeks or months of guessing at the cause. Whether your symptoms point to a structural arch problem or a classic plantar fasciitis pattern, getting an accurate diagnosis is what unlocks the right care plan for your situation.
Your podiatrist can confirm the cause, rule out more serious conditions like stress fractures or tendon tears, and build a treatment plan specific to your diagnosis. That plan might include custom orthotics, physical therapy, stretching protocols, or other interventions matched to what your foot actually needs. You don’t have to keep managing daily pain on your own. Book a same-day appointment at Achilles Foot and Ankle Center and take the first real step toward lasting relief.






