You’re finally settling into bed after a long day, and then it hits, a sharp, seizing pain shooting through your foot. Foot cramps during pregnancy are one of those symptoms nobody warns you about until you’re wide awake at 2 a.m., gripping your toes and wondering what just happened. The good news: you’re not alone, and there’s usually a clear reason behind it.
Hormonal shifts, extra weight on your feet, changes in circulation, and nutritional demands all play a role. Some cramps are mild annoyances. Others stop you mid-step. Either way, understanding the cause is the first step toward getting relief. At Achilles Foot and Ankle Center, our podiatrists work with pregnant patients across Central Virginia who deal with exactly this, foot and ankle pain that disrupts daily life during a time when comfort matters most.
This article breaks down why pregnancy triggers foot cramps, what you can do to stop them quickly, and when it’s worth seeing a specialist.
What foot cramps during pregnancy feel like
Foot cramps during pregnancy can range from a mild tightening you push through to a full muscle spasm that forces you to stop moving entirely. Most pregnant women describe the sensation as a sudden, involuntary contraction where the muscle seizes and refuses to release for several seconds or even a few minutes. There is usually no buildup or warning.
The sensation itself
The cramp often starts without any signal. Your foot or calf muscle locks up, and the harder you try to resist it, the tighter it seems to get. Some women feel a sharp, stabbing pain concentrated in the arch of the foot. Others experience a pulling sensation that spreads from the ball of the foot up through the heel, making it nearly impossible to flex or point the toes normally until the spasm passes.
After the cramp releases, the area often stays tender and sore for several hours. That lingering ache is your muscle recovering from the sudden contraction it just went through. If cramps are happening regularly, that soreness can accumulate over days and make walking feel uncomfortable even between episodes.
Where and when cramps tend to hit
Cramps most commonly strike in the arch, the toes, and the calf, and sometimes all three at once. The foot is especially vulnerable during pregnancy because weight distribution shifts forward, placing more load on the arch and forefoot throughout the day. As your body changes, the muscles in your feet work harder just to keep you upright and balanced.

Nighttime is the most common trigger, largely because circulation slows when you are lying still and electrolyte levels drop after a full day of physical demands.
Many women also notice cramps when they stretch their legs in bed, point their toes, or sit in one position too long. Footwear plays a role here as well. Wearing unsupportive shoes during the day compresses the foot muscles, leaving them primed to cramp the moment the shoes come off and the muscle finally tries to relax.
Why foot cramps happen during pregnancy
Foot cramps during pregnancy rarely have a single cause. Instead, several physical changes stack on top of each other, and your feet end up bearing the consequence. Understanding which factor is driving your cramps helps you target the right fix rather than guessing.
Circulation and added weight
As your uterus grows, it puts pressure on the veins running through your pelvis, which slows blood flow returning from your legs and feet. Poor circulation means your foot muscles receive less oxygen during the night, making them far more likely to seize. At the same time, your body weight increases steadily throughout pregnancy, loading your arches and forefoot with every step you take.
That combination of reduced circulation and increased mechanical load is why foot cramps tend to get worse as pregnancy progresses into the second and third trimesters.
Nutrient and fluid shifts
Your body redirects magnesium, potassium, and calcium toward your growing baby, which can leave your muscles with less of the minerals they need to contract and release normally. Magnesium in particular plays a direct role in muscle relaxation, so even a mild shortfall can trigger spasms. Dehydration makes this worse because low fluid intake thickens the blood slightly, reducing how efficiently nutrients reach the small muscles in your feet. Hormonal changes during pregnancy also affect how your kidneys process electrolytes, which adds another layer of unpredictability.
How to stop a foot cramp fast
When a cramp hits, your instinct might be to curl up and wait it out. That approach actually prolongs it. Foot cramps during pregnancy respond best to immediate, active intervention rather than staying still.
Stretch and move the muscle
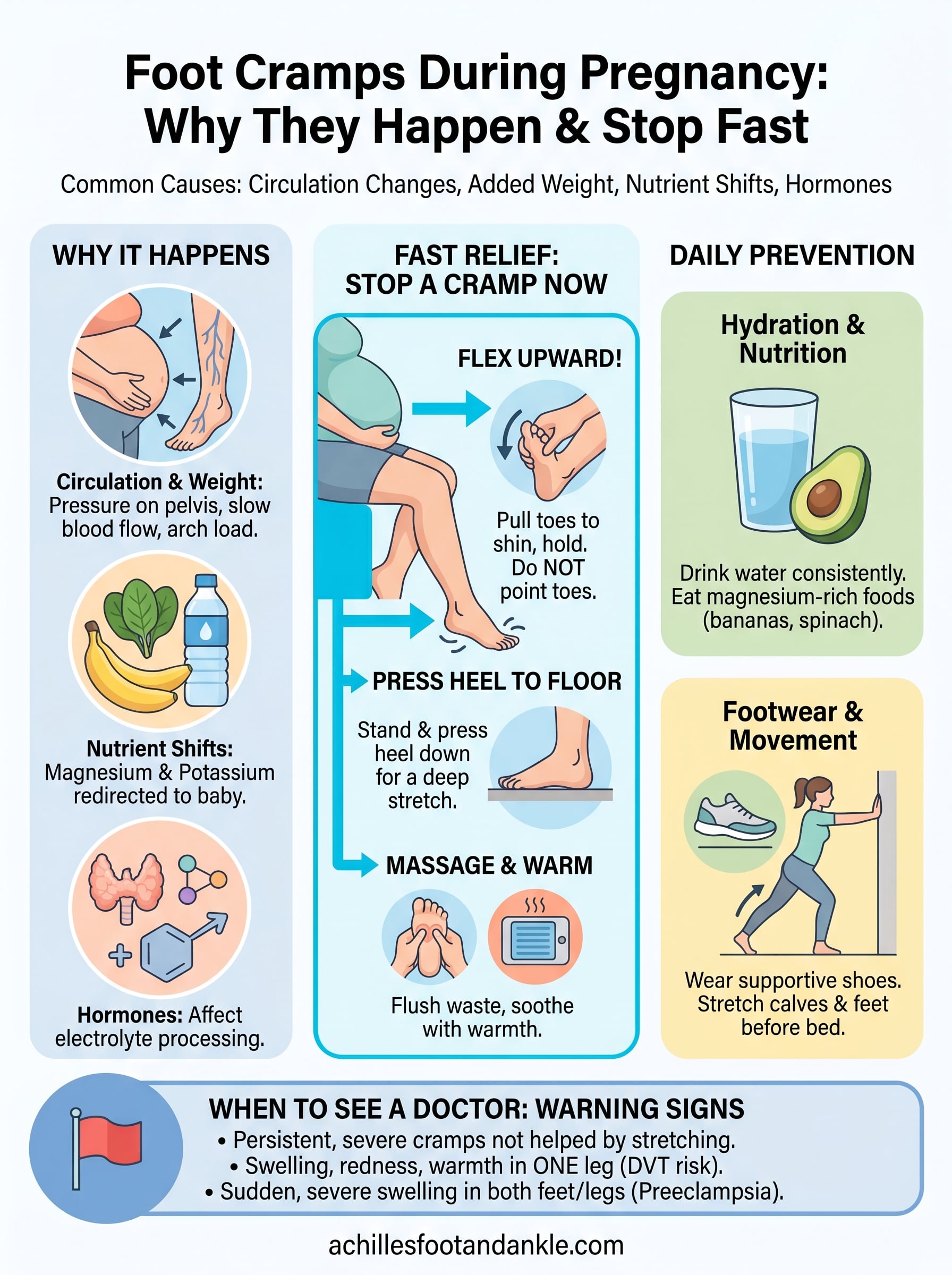
The fastest way to break a cramp is to flex your foot upward, pulling your toes toward your shin rather than pointing them away. Pointing your toes is a common reflex, but it tightens the very muscle that is already seizing. Instead, flex hard, hold for several seconds, and repeat until the spasm releases. If you can stand safely, pressing your heel flat into the floor while keeping your leg straight gives the arch and calf muscles a firm, sustained stretch that forces the contraction to let go.

Standing on a cold floor can also trigger a reflex that helps the muscle release, so stepping out of bed during a cramp often works faster than stretching from a lying position.
Massage and warm the area
Once the initial spasm passes, firm massage along the arch and sole helps flush out the metabolic waste that built up during the contraction. Use your thumbs to apply steady pressure from the heel toward the ball of the foot. Following that with a warm towel or heating pad for five to ten minutes reduces the residual soreness and helps the muscle settle before you try to go back to sleep.
How to prevent foot cramps day to day
Stopping foot cramps during pregnancy before they start comes down to a few consistent habits. Small daily adjustments to what you eat, drink, and wear add up quickly and make a real difference in how often cramps occur.
Hydration and nutrition
Your muscles need adequate fluid and minerals to function without seizing. Aim to drink water consistently throughout the day rather than catching up in large amounts at night. Foods rich in magnesium and potassium, such as bananas, spinach, avocado, and pumpkin seeds, support normal muscle contraction and relaxation. Talk to your OB or midwife about whether your prenatal vitamin covers your magnesium needs, since many standard formulas fall short of what your muscles actually require.
Getting enough magnesium through food and supplementation is one of the most direct ways to reduce cramp frequency during pregnancy.
Footwear and movement habits
Wearing supportive shoes with adequate arch support throughout the day prevents your foot muscles from overworking and arriving at bedtime already fatigued. Flat, unsupported footwear forces your arch to absorb load without help, which sets the stage for nighttime cramping. Before bed, spend two to three minutes stretching your calves and feet, pulling your toes gently toward your shin and rolling your foot along a tennis ball. Elevating your legs for short periods during the day also helps circulation return from your lower extremities, reducing the buildup that triggers cramps overnight.
When cramps signal something more serious
Most foot cramps during pregnancy are uncomfortable but harmless. However, some symptoms that feel like cramping are your body signaling a condition that needs medical attention. Knowing the difference helps you act quickly rather than dismissing something that actually requires care.
Signs that warrant a call to your doctor
If your cramps are happening multiple times per day, lasting longer than a few minutes, or not responding to stretching, that pattern is worth reporting to your OB or a podiatrist. Severe or persistent cramping can sometimes indicate significant magnesium deficiency or a circulatory problem that needs direct evaluation rather than home management. You should also pay attention if the pain is localized to one leg and not symmetrical, which sets it apart from the typical bilateral cramping most pregnant women experience.
Deep vein thrombosis: what to watch for
One condition to take seriously is deep vein thrombosis (DVT), a blood clot in a deep vein that pregnancy significantly raises your risk for. DVT does not always feel like a cramp. Instead, you may notice persistent swelling, redness, warmth, or a dull ache in one calf or leg that does not resolve with rest or movement.
If one leg looks noticeably more swollen than the other, or if you feel sudden shortness of breath alongside leg pain, seek emergency care immediately.
Sudden, severe swelling in both feet can also indicate preeclampsia, a serious pregnancy complication requiring prompt evaluation.
Key takeaways and next steps
Foot cramps during pregnancy are common, but they are not something you just have to endure. Circulation changes, added weight, and depleted minerals are the main drivers, and each one responds to targeted action. Staying hydrated, eating magnesium-rich foods, stretching before bed, and choosing supportive footwear throughout the day will reduce how often cramps hit and how long they last when they do.
Pay attention to symptoms that fall outside the typical pattern. Swelling in one leg, persistent pain that does not improve with stretching, or sudden leg swelling paired with shortness of breath all require prompt medical evaluation rather than home care.
If your cramps are frequent, severe, or disrupting your daily movement, a podiatrist can help you identify what is driving them and build a plan specific to your situation. Schedule a same-day appointment with our team at Achilles Foot and Ankle Center today.






