A stress fracture in your foot can stop you in your tracks, that sharp, nagging pain that gets worse with every step. Whether it happened during a run, from ramping up activity too quickly, or just from daily wear and tear, you’re probably wondering about stress fracture foot treatment at home and what you can do right now to start healing. The good news is that many stress fractures respond well to consistent at-home care when you act early and follow the right steps.
At Achilles Foot and Ankle Center, our podiatrists across Central Virginia treat stress fractures regularly, from weekend warriors to patients who spend long hours on their feet at work. We know that not every fracture requires surgery, and that proper self-care plays a major role in recovery. We also know when home treatment isn’t enough, which is why getting a professional diagnosis first matters more than most people realize.
This guide walks you through the specific steps you can take at home to manage pain, protect the bone, and give your foot the best chance to heal fully. You’ll learn what works, what to avoid, and the signs that it’s time to see a specialist before a small fracture becomes a bigger problem.
Before you start home treatment
Home care works best when you know exactly what you’re treating. Foot pain after repetitive activity can come from plantar fasciitis, tendinitis, bursitis, or a stress fracture, and treating the wrong condition the wrong way can set you back weeks. Before you commit to any stress fracture foot treatment at home, take a moment to confirm what you’re actually dealing with.
Get a proper diagnosis first
The most important step before icing your foot or loading up on anti-inflammatories is seeing a podiatrist or doctor for an evaluation. Stress fractures are tiny cracks in the bone, and they don’t always show up on standard X-rays in the first one to two weeks. A clinical exam combined with a detailed history of your symptoms is often enough for a working diagnosis that lets you start treatment right away.
If your pain came on gradually during or after repetitive activity, worsened with weight-bearing, and improved with rest, those are textbook signs of a stress fracture.
Signs that point toward a stress fracture rather than soft tissue pain include:
- Pain that is sharp and localized to a specific spot on the bone, not a broad, general ache
- Tenderness when you press directly on the bone
- Swelling or mild bruising over the painful area
- Pain that worsens with activity and noticeably improves after rest
Know which bones are most commonly affected
Stress fractures in the foot typically occur in the metatarsal bones (the long bones leading to your toes), the navicular bone on the top of the midfoot, and the calcaneus (heel bone). The location matters because some bones carry a higher risk of complications if they go untreated. For example, navicular stress fractures have a poor blood supply and often require stricter immobilization or even surgery, while second and third metatarsal fractures tend to heal well with consistent home care.
Your pain location gives you and your doctor critical information. If your pain sits on the top of your midfoot or the outer edge near the fifth metatarsal, do not skip a professional evaluation before starting home treatment. Those locations are higher-risk zones where self-care alone is frequently not enough to prevent the fracture from worsening.
Set realistic expectations for recovery
Most low-risk stress fractures take six to eight weeks to heal with proper care, and that timeline only holds if you follow through consistently, not just for the first few days when the pain is at its worst. Cutting rest short because the pain fades early is one of the most common reasons patients re-injure the same foot within weeks. Go into home treatment with a clear plan and a genuine commitment to seeing it through to the end.
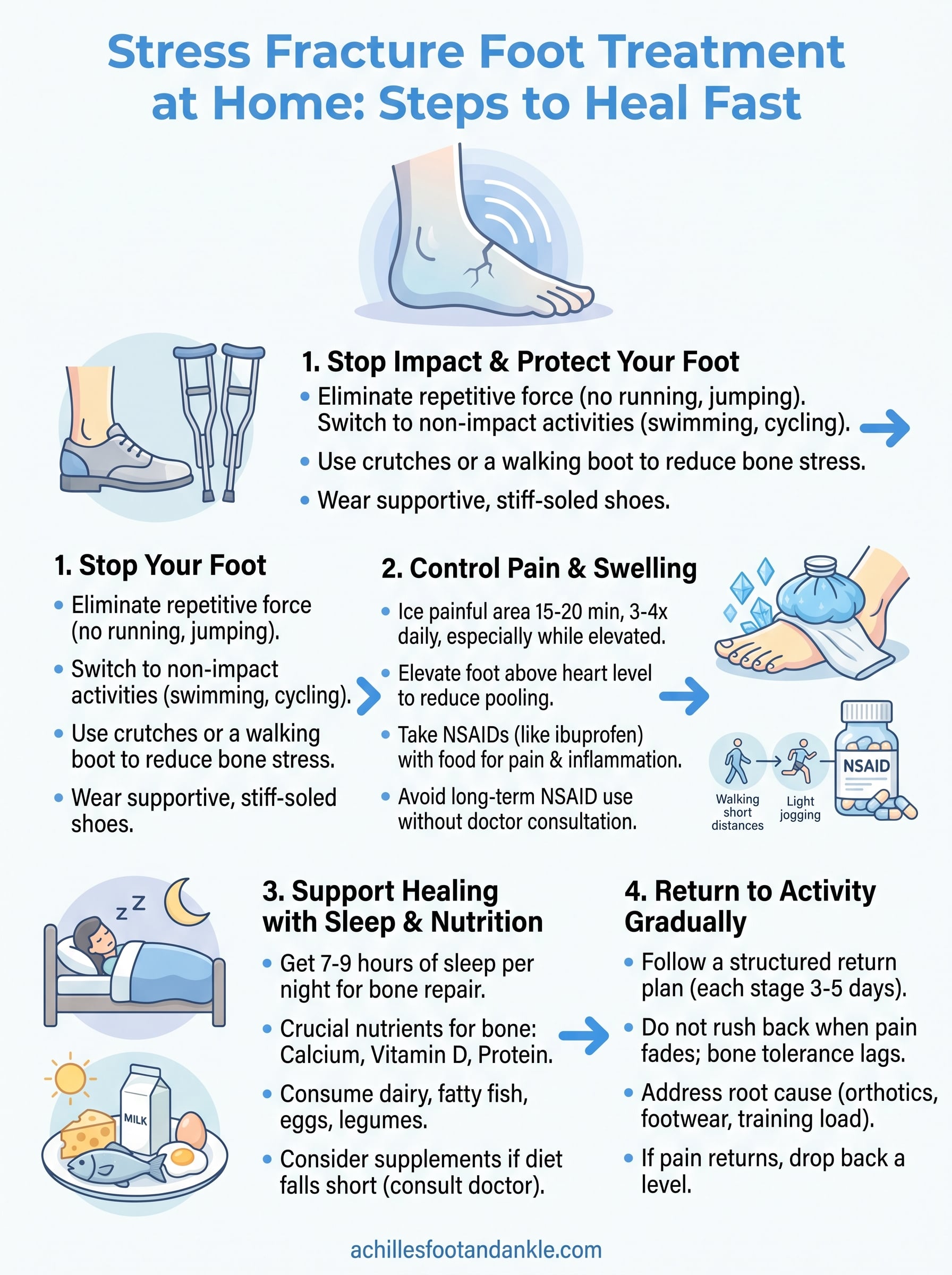
Step 1. Stop impact and protect your foot
The single most effective thing you can do for stress fracture foot treatment at home is to stop loading the injured bone right now. Every step you take on a fractured bone increases the risk that the crack widens, and a crack that widens can go from a manageable six-week recovery to a full break requiring surgery. Protecting the bone from further stress is not optional; it is the foundation of everything else in your recovery plan.
Cut out weight-bearing activity immediately
You need to eliminate any activity that puts repetitive force through your foot. That means no running, jumping, or extended walking until your pain has dropped significantly and a healthcare provider clears you to progress. Switching to non-impact alternatives like swimming or upper-body strength work keeps you moving without loading the fracture site.
Complete rest from impact activities for the first two to three weeks gives the bone its best chance to start healing without re-injury.
A simple activity modification plan looks like this:
| Current activity | Safe alternative |
|---|---|
| Running | Swimming or cycling |
| Walking long distances | Limit steps; use crutches if needed |
| Standing for long shifts | Seated work or supportive boot |
| Treadmill or elliptical | Upper-body ergometer |
Choose the right footwear and walking aids
Stiff-soled shoes or a walking boot dramatically reduce the flex and pressure at the fracture site during unavoidable weight-bearing. If your doctor has not yet prescribed a boot, wear the most rigid, supportive shoe you own until your appointment, and avoid bare feet on hard floors entirely.
Crutches are worth considering if every step causes significant pain. Using crutches for the first one to two weeks of recovery can meaningfully reduce stress on the bone and shorten your overall healing timeline by preventing repeated microtrauma to the fracture site.
Step 2. Control pain and swelling safely at home
As part of your stress fracture foot treatment at home, managing pain and inflammation is just as important as rest. Swelling at a fracture site increases pressure on the bone and surrounding tissue, which slows your recovery if you ignore it. The good news is that two straightforward tools, ice and over-the-counter medication, can keep symptoms under control when you use them correctly and consistently.
Ice the fracture site consistently
Apply ice to the painful area of your foot for 15 to 20 minutes at a time, three to four times a day, especially during the first 48 to 72 hours after your symptoms peak. Always wrap the ice pack in a thin cloth before placing it against your skin to prevent frostbite. Elevating your foot above heart level while icing amplifies the effect by reducing blood pooling and pressure at the injury site.

Icing while elevated works better than icing alone, so combine both whenever you have the chance to sit or lie down.
A practical daily icing schedule to follow:
- Morning: Ice for 15 to 20 minutes before you start moving around
- Midday: Ice again after any unavoidable walking or standing
- Evening: Ice before bed with your foot elevated on two pillows
- After any activity: Ice within 30 minutes every time
Use over-the-counter pain relief wisely
NSAIDs like ibuprofen (Advil, Motrin) reduce both pain and inflammation, making them a better choice for stress fractures than acetaminophen, which addresses pain only. Take them with food and follow the recommended dosage on the label; exceeding the dose does not speed up healing and can irritate your stomach with regular use.
Avoid taking NSAIDs continuously for more than ten days without talking to a doctor. Long-term NSAID use has been studied for its potential to slow bone healing, so use the lowest effective dose for the shortest time needed to stay comfortable.
Step 3. Support bone healing with sleep and nutrition
Rest and ice get most of the attention during stress fracture foot treatment at home, but what happens inside your body overnight and at the dinner table matters just as much. Bone repair is an active biological process that demands raw materials and energy, and your body carries out most of that work while you sleep and through the nutrients you give it consistently.
Get enough sleep for bone repair
Your body releases growth hormone during deep sleep, which plays a direct role in bone remodeling and tissue repair. Aim for seven to nine hours of sleep per night throughout your recovery, not just during the first painful days. Skimping on sleep disrupts the cycle of bone resorption and new bone formation, which stretches out how long you spend off your feet.
Consistent, quality sleep is one of the most underused tools in bone fracture recovery, and it costs nothing.
Poor sleep also raises cortisol, a stress hormone that slows the inflammatory cleanup your body needs to move into the bone-building phase. A cool, dark room and a consistent bedtime give your body the conditions it needs to run that repair cycle efficiently every night.
Eat and supplement for faster bone healing
The nutrients your bone needs most are calcium, vitamin D, and protein. Calcium provides the structural mineral for new bone tissue, vitamin D controls how efficiently your body absorbs that calcium, and protein supports the collagen framework that the new bone forms around.
Practical daily targets to hit during recovery:
| Nutrient | Daily target | Good food sources |
|---|---|---|
| Calcium | 1,000-1,200 mg | Dairy, fortified plant milk, sardines |
| Vitamin D | 600-800 IU | Fatty fish, egg yolks, sunlight |
| Protein | 0.7-1 g per lb body weight | Chicken, eggs, legumes, Greek yogurt |
If your diet falls short of these targets, a combined calcium and vitamin D supplement can fill the gap. Talk to your doctor before starting any supplement to confirm the right dose, since both nutrients have upper limits where excess intake causes problems rather than faster healing.
Step 4. Return to activity and prevent another fracture
Returning to full activity too soon is the most common mistake people make after a stress fracture heals. Pain fading is not the same as the bone being fully repaired, and rushing back to running or high-impact exercise before the six-to-eight-week window closes is a fast way to end up with the same injury. Your goal in this phase of stress fracture foot treatment at home is to rebuild gradually, not to make up for lost time.
Follow a structured return-to-activity plan
Your reintroduction to impact activity should move in predictable, small steps. Each stage should last at least three to five days before you progress, and any return of pain is a signal to drop back one level and hold there for another week before trying again.
A basic return-to-activity progression to follow:
| Stage | Activity level | Duration |
|---|---|---|
| 1 | Walking short distances, flat surfaces only | Days 1-5 |
| 2 | Extended walking, light daily activity | Days 6-10 |
| 3 | Low-impact cross-training (cycling, swimming) | Days 11-17 |
| 4 | Light jogging on soft surfaces | Days 18-24 |
| 5 | Gradual return to full training load | Week 5 onward |
Never skip a stage because you feel good; bone tolerance lags behind how you feel by several days.
Address the root cause to prevent recurrence
Most stress fractures have a cause you can change, whether that’s training load, footwear, gait mechanics, or nutritional gaps. Once you return to activity, work with a podiatrist to identify what set you up for the fracture in the first place.
Custom orthotics, a structured training schedule, and adequate calcium and vitamin D form the core of a strong prevention plan. Replacing your athletic shoes every 300 to 500 miles and avoiding sudden increases in weekly mileage above ten percent keep the bone stress inside a range your foot can handle.
If your foot is not improving, get help
Consistent stress fracture foot treatment at home works for most low-risk fractures, but some injuries need more than rest and ice. If your pain is not decreasing after two to three weeks of careful home care, or if it is getting worse despite following every step in this guide, the fracture may have progressed or there may be a different underlying problem that home treatment cannot fix.
Watch for these specific warning signs that require a professional evaluation:
- Pain that stays the same or worsens after two weeks of rest
- Visible deformity, significant swelling, or bruising that spreads beyond the initial injury site
- Numbness or tingling in your toes
- Pain that wakes you up at night
A podiatrist can confirm the fracture’s status, adjust your treatment plan, and prevent a small crack from turning into a full break. Do not wait and hope the pain resolves on its own. Schedule a same-day appointment with Achilles Foot and Ankle Center today.






